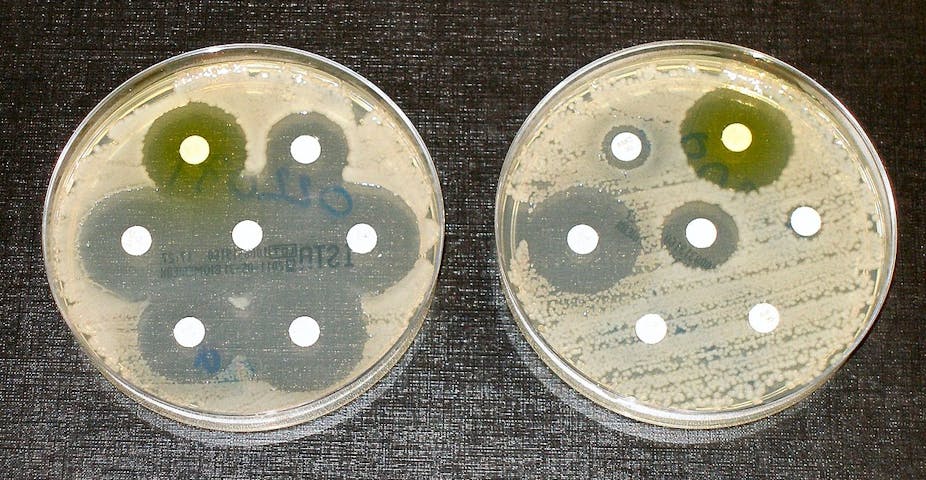
The development of resistant bacteria over the past 50 years stands testament to the power of evolution. While scientists have discovered or created hundreds of antibiotics to kill bacteria, those bacteria have almost as rapidly evolved to survive their use. The greater the exposure to antibiotics, the more rapid the evolution. This simple fact explains the urgent need to control the abuse of antibiotics used among people, and in agriculture.
Resistant bacteria – CREs, MRSA, and others – have become a significant threat to human health. Strains resistant to many drugs have grown rapidly in hospitals, and in the wider environment. Highly resistant pathogens are now found in the rivers of India and China, due to sewage discharge. Owing to the lack of effective drugs, treatment for those infected with these bacteria is very difficult, and their prognosis grim.
At the same time, there is a dearth of investment in new antibiotics: hospitals tend to reserve new antibiotics for infections that are resistant to older antibiotics or other drugs, and the potential market is very small. But there is a legitimate question of whether new antibiotics will be available at a large scale when they are needed.
This rapid spread of resistant bacteria is in part due to massive overuse of antibiotics beyond humans. While international data is not available, the evidence from the US is compelling: the country uses approximately 40 tonnes of agricultural antibiotics every day. Most of this is fed to livestock to increase growth, and the rest used to control disease caused by high-density factory farming lots. Antibiotics are also used in fish farms for the same reasons, and on some crops to control mold.
So, the risk that antibiotic overuse poses to human health by accelerating the process of resistance has provoked regulators to try to limit this practice. The EU has since 2006 banned the use of growth-promoting antibiotics. In the US, the FDA has been taking baby steps towards a voluntary ban on growth promotion. However, in much of the world – including China, India, and Brazil, which raise the most livestock – the restrictions on antibiotic use are weak or non-existent. Nevertheless, in most developed countries, it seems likely that farmers can anticipate increasingly onerous regulations that control how they use antibiotics. It will be costly for farmers to ensure and document compliance, since the regulations are likely to require more veterinary supervision, and enforcement will also have to be paid for.
In a recent article in the New England Journal of Medicine, Ziana Ahmed and I proposed a solution to the twin problems of excessive antibiotic use in agriculture and the increasingly desperate shortfall in investment in new antibiotics. Countries should apply fees to all non-human use of antibiotics. The higher prices faced by farmers would discourage low-value uses of antibiotics, and encourage farmers to look for alternative methods to speed growth and limit infection.
Applying fees instead of regulation has significant advantages. User fees would raise revenues that could support R&D into new antibiotics, and stewardship programs to help protect existing antibiotics. New drugs would be valuable for human patients and also for agriculture, which faces its own problems with bacterial resistance.
User fees would be more flexible, in the sense that farmers could decide whether they wanted to use antibiotics in a particular application, or not. Laws and regulations can at best prohibit certain uses, such as growth promotion, but they do nothing to discourage inappropriate use of antibiotics in other situations.
User fees would also be simple to administer and monitor, by applying charges at the manufacturer or importer level to all sales of antibiotics not destined for human use. This would be much easier than monitoring every livestock farmer and veterinarian.
Finally – and this is very important – applying a system of fees would be much more attractive internationally. The problem with a regulatory approach is that even if international agreement could be reached, different countries’ levels of enforcement would be variable. This would create cost advantages for some producers in countries without strict regulation, while still resulting in overuse of antibiotics.
So it seems the choice is arguably between applying an internationally agreed tax, or struggling to agree upon and implement a system of regulations that is then only haphazardly enforced, which ultimately brings us back to square one.