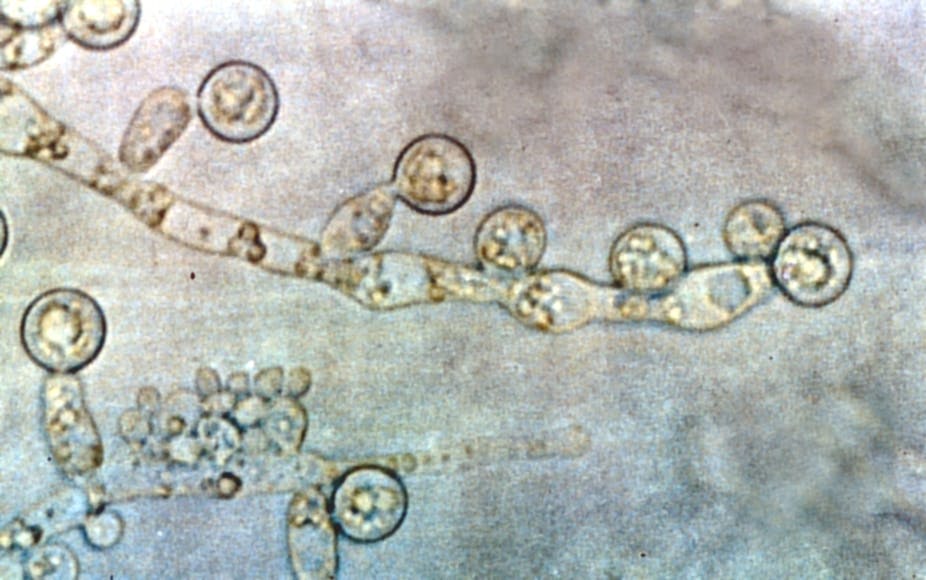
On hearing the word “fungi” most people will probably think of pizza al funghi or a portobello mushroom burger. Incidentally, roughly half of the people salivating about these dishes will also carry a fungus called Candida albicans in their mouths or digestive tracts where it lives quietly, invisibly to the human eye, without causing disruptions or symptoms.
But Candida albicans does not always go unnoticed. While most people carrying the fungus will go through life without ever learning the scientific name of their innocuous tenant, also called a “commensal”, some do encounter it as the common cause of oral thrush, nappy rush or vaginal yeast infections. Indeed, 75% of women will experience at least one episode of yeast infection throughout their lifetime.
It gets worse. Changes to a person’s immune defences can help Candida albicans cause life-threatening infections of the blood stream and the inner organs. Patients suffering HIV/AIDS or those undergoing cancer chemotherapy or solid organ transplants or babies with low birth weight are at risk of contracting this infectious disease. Candida albicans is the most commonly acquired fungal infections in a hospital setting, particularly among patients in intensive care units.
Global infection
The consequences are dire. Each year, around 700 patients die of Candida albicans infections in the UK alone. This is about as many as those that die of infections caused by Methicillin Resistant Staphylococcus aureus or MRSA. But while rates of MRSA have been falling, rates of Candida albicans infections remained steady over a five-year period. In addition to the human suffering, each Candida albicans infection adds about £16,500 extra to an adult’s hospital bill as it prolongs the time the patient needs to spend in the intensive care unit by more than five days.
However, Candida albicans infections, like many other fungal diseases, are a global problem. Around the world, 400,000 people suffer each year from infections of the blood stream and the organs – and this number is rising. With the advent of new medical procedures that has led to an increase in people with compromised immune systems, the incidence rate of Candida albicans infections is on the rise as well. A review of 750m hospitalisations in the US revealed that the rate of fungal bloodstream infections has increased by more than 200% within a couple of decades. With mortality rates of up to 75%, the human burden is substantial, demanding effective therapeutic strategies. There are, however, two major obstacles that severely hamper our ability to prevent or treat life-threatening Candida albicans infections.
Human colonisation

Preventing transmission of Candida albicans is next to impossible because the enemy lives within. While the spread of viral or bacterial infections can often successfully be averted by quite simple measures, such as washing the hands or using condoms, these are not an option for a fungus that colonises humans during birth or shortly after – passing through the birth canal, or possibly through nursing, or through the close mother-child relationship in general (for example by licking pacifiers) provide ample opportunities for the fungus to colonise our mouths as babies and for it to eventually enter our digestive tract.
From mouth mate to death rate
The transition between living in and on humans without causing trouble to suddenly causing a life-threatening disease is a puzzle. Scientists are only just now beginning to unravel how Candida albicans flips the switch that turns it into a deadly threat, requiring immediate medical intervention and the application of antifungal drugs. Recent research showed that Candida albicans co-opts a molecular signal that usually regulates mating in the fungus. This signal down-regulates any fungal features associated with causing disease. This way, scientists assume, Candida albicans can be present in the intestines without alerting the immune system to its presence. Curiously, this molecular switch is also controlled by the nutrient composition in the human gut. The exact nature of this, however, remains enigmatic.
Which leads to the second major problem associated with Candida albicans infections. They are difficult to treat because only few drugs that kill fungi exist. The reason for why there are so many fewer anti-fungal than antibacterial drugs lies in our shared evolutionary history. Fungi are more closely related to humans than bacteria, which means that there are less specific molecules in the fungus that can be targeted to stop the fungus from growing. This, in combination with the challenges of drug design in general, dramatically slows down the development of anti-fungal drugs. So much so that it has been almost ten years since the last anti-fungal drug class received approval.
Candida albicans is not the only fungus that threatens human health and life. The top ten most aggressive fungi kill as many, if not more, people as tuberculosis or malaria. Worldwide, an estimated 1.5m patients die from fungal infections each year.