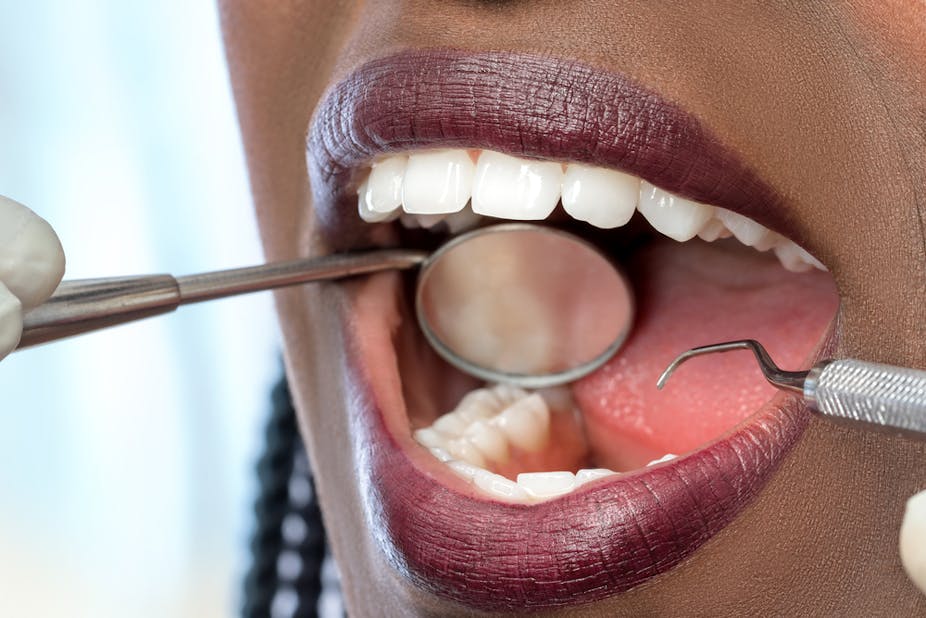
Women who develop severe mouth infections and suffer from bleeding gums when they are pregnant have a greater chance of delivering their babies preterm if they don’t treat the infection.
Up to 70% of women develop inflammation of the gums, or gingivitis, during their pregnancy. It’s commonly referred to as pregnancy gingivitis. This is due to the changes in a mother’s hormone levels during pregnancy. This promotes an inflammatory response which increases the risk of developing periodontal disease.
Periodontal diseases are infections of the structures around the teeth including the gums, ligaments and bone. They may cause bleeding of the gums and in severe cases, loss of teeth.
The challenge is that not many mothers seek dental treatment for bleeding gums during pregnancy. And antenatal clinics pay little, if any, attention to the mother’s oral health status. As a result, this complication often goes undetected.
Our research shows that incorporating a rapid point-of-care test into routine antenatal examinations could help diagnose periodontal disease. The test is simple and inexpensive and is widely used as a diagnostic test for periodontal disease.
If the test is set up before the patient is examined, it can deliver a result by the time her examination is complete. This would alert antenatal health care providers of the risk of adverse pregnancy outcomes. Mothers can then be referred to a dental clinic for prompt treatment to reduce their risk.
Premature babies
Across the world, about 6.9 million babies die due to prematurity. Many as a result of their birth weight being low. In the US about 7% of babies are born with a low birth weight while in the UK, this figure sits at 6%.
But in Africa up to 12% of babies are born with a low birth weight. In South Africa neonatal deaths account for about 40% of all deaths in children under the age of 5. In Angola and the Central African Republic, close to 100 babies in every 1000 die within the first four weeks of birth. These are the highest known rates of infant death in the world. This compares to the UK and the US where only seven in every 1000 infants die within the first four weeks of life.
Studies have linked babies born prematurely with a low birth weight to their mothers’ smoking habits, and her ethnicity. Other factors have also played a role such as the mother’s age, whether she previously delivered a baby that had a low birth weight, whether she had pregnancy complications and the type of delivery she had.
Some research found a link between periodontal disease and adverse pregnancy outcomes but other studies couldn’t establish a conclusive link. None of these studies were in the developing world.
But our research in South Africa and Rwanda has found a link between mothers with periodontal disease that deliver underweight preterm babies. Our study was the first in Africa to link periodontal disease to pre-term delivery.
What we found
As part of our research we did two studies. One focused on pregnant women during their antenatal visits to maternal obstetric units in Kwazulu-Natal. The other looked at mothers admitted to labour wards in Rwanda’s Butare Hospital.
One study showed there was a strong likelihood that there would be an adverse pregnancy outcome when a mother was clinically diagnosed with periodontal disease. Those who didn’t have periodontal disease were more likely to have normal pregnancy outcomes.
The other study focused on the specifics of the bacteria associated with periodontal disease.
In the immune system there are two sets of proteins called cytokines, which regulate the body’s response to an inflammation. There are pro-inflammatory cytokines and anti-inflammatory cytokines. In normal full term pregnancies, proteins that encourage inflammation in the body are regulated by those that dismiss the inflammation. This prevents the body developing an inflammation and rejecting the fetus.
But our studies confirmed that when a woman had periodontal disease there was an imbalance in these proteins which could create an inflammation in the woman’s body and induce preterm labour.
Changing testing patterns
The earlier periodontal disease is diagnosed in pregnant women, the less of a chance it has of having an impact on their delivery.
Surveys into practice behaviours of obstetricians in other countries show there’s growing awareness of the link between periodontal disease and adverse pregnancy outcomes.
But not enough is being done to forge the collaboration between the antenatal health care providers and oral health care professionals.
Obstetricians argue that they have no time to perform oral examinations during antenatal consultations. And, they argue, these would be better performed by oral health care workers.