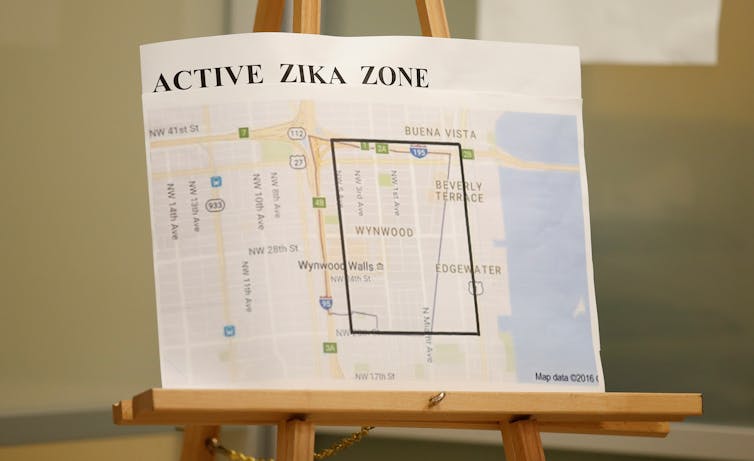
On Sept. 1, officials in Florida reported that mosquitoes carrying the Zika virus had been found in Miami Beach. The Florida Department of Health reports 49 non-travel related cases of Zika. There are almost 2,700 cases of travel-associated cases in the continental U.S. Things are worse in the U.S. territories, where more than 14,000 locally acquired cases have been reported.
So, how is the U.S. responding to Zika? The Centers for Disease Control and Prevention is doing what it can to support efforts to halt disease transmission and support state and local government. But on August 30 CDC Director Tom Frieden announced that the agency had almost run out of money to fight the virus. Congress has yet to pass a funding bill, leaving the Obama administration to redirect money earmarked for other purposes to support Zika research and response efforts.
The response so far seem fragmented, and even somewhat contentious. So why is that? We can look back to the Ebola crisis in the U.S. in 2014 for some answers. As my colleague Phillip Singer and I found in a case study, the response to that public health crisis was shaped by the fragmented and partisan U.S. political system, not by epidemiology or medicine.
How does public health in the U.S. actually work?
The United States is a tremendously fragmented political system, with about 90,000 local governments, in addition to the 50 states and federal government. Local public health policy is mostly overseen, created and funded at the state level.
And public health work from disease surveillance to health education to mosquito abatement is done by local governments and nonprofits that work with them. These include safety net health care facilities, mosquito abatement agencies (whose very presence is patchy), social services agencies and so on.
However, public health at the state and local level is often underfunded. If disease threats seem more distant, state and local governments may assume that there will be no threats or that the federal government will help them out if something does happen. Recessions are especially likely to lead to reduced funding in areas like clinics for the poor or mosquito abatement.
When a crisis does happen, the responses within individual states tend to be driven by governors, who will often take guidance from the federal government. However, we found that national political ambitions can influence how governors react. They can choose to show leadership, or challenge the president, in ways that aid their own ambitions.
For instance, New Jersey Governor Chris Christie tried to quarantine a nurse who had returned from work in West Africa, while Louisiana Governor Bobby Jindal threatened to quarantine any members of The American Society of Tropical Medicine and Hygiene who tried to attend their conference in New Orleans after working in affected countries. Both men announced presidential bids within the following year.
Who’s in charge during a public health crisis?
So who is in charge during a public health crisis? Formally, a wide variety of local governments under the aegis of states. But because public health in the U.S. is fragmented and often underfunded, the federal government’s money and expertise give it a great deal of influence to shape responses.
For instance, CDC guidelines and statements are tremendously influential in or out of crisis periods. States aren’t legally obligated to adopt CDC guidelines, but they generally do. For instance, within a week of the CDC releasing guidance for monitoring people with potential exposure to Ebola in the U.S., all 50 states, as well as New York City and Washington, D.C., had implemented them.
While politicians like Christie or Jindal can choose to defy federal advice, most prefer to fall into line. With Zika, states have already been working with the federal government to think through their responses.
And as we learned in our case study of Ebola, public health works through persuasion rather than hierarchy. For example, the White House’s “Ebola Czar” was telephoning hospitals trying to persuade them to take patients with Ebola in case there were new cases.
Federal money can also support disease control efforts on the ground, and compensate for the fact the local public health is underfunded. So, it poses a problem when the federal government isn’t supplying the money. Which, right now, it isn’t.

How is the Zika response shaping up?
When the link between Zika and microcephaly started to become clear in late 2015, the Obama administration responded quickly. By early February 2016 the White House sent a proposal to Congress for US$1.9 billion in supplemental funding to strengthen local public health responses, including in hard-hit US territories such as Puerto Rico, expand Zika testing in the United States and support research on a vaccine. About $400 million was earmarked to fight the disease abroad.
The House and Senate responded with bills of their of own. The Senate bill cut the allocation and would have put Ebola funds toward Zika response. The House bill offered one-third of the funding the administration requested.
While Congress stalemated, the Obama administration transferred almost $600 million, much of it from unused Ebola funds, to fight Zika. Congress didn’t send a bill to the president to sign, and in July, legislators recessed in July with Zika funding still in limbo.
In August, the Obama administration used its administrative flexibility to move $81 million from biomedical research, Ebola response and other health programs to keep a Zika vaccine study going and support to the local governments.
These executive actions reduced the pressure on Congress to act by funding Zika response and vaccine research, even if only shoestring budget. And because Congress hasn’t appropriated money for Zika yet, every dollar spent on it has been taken from some other priority.
And now the CDC, which has been supporting Zika response efforts (including giving money to partners organizations to support local, state, territorial and tribal efforts), is running out of the money that the administration reallocated from other uses to combat the virus.
Will Zika funding pass before November 8?
Pressure is mounting on Congress to act. Three-quarters of the public in a Kaiser Family Foundation survey think it is an issue that needs to be addressed when Congress returns from recess on Sept. 6.
Florida Republicans including Marco Rubio and Governor Rick Scott have already started to attack Washington’s inaction. Democrats, including President Obama, continue to attack Republicans in Congress over the slowness of the response.
Fear of Zika might start to overcome partisanship, but there is no guarantee that will happen before Nov. 8. It’s worth noting that even as Ebola became a major issue in 2014, it wasn’t until after the midterm elections that Congress actually passed a funding bill. Before the elections, politicians, especially Republicans who hoped to make gains in Congress, linked it to immigration and border security, emphasized biological threats and attacked the executive branch’s response.
Looking at Washington might make us glad that all does not depend on federal politics. But that is not so comforting when we consider the funding and capacity of local and state governments in the areas, particularly along the Gulf Coast, that are most endangered. This spring Miami-Dade County had a mosquito control staff of 17. It is now under a domestic travel advisory.

