It is often cited that one in three people on the planet are thought to be infected with Mycobacterium tuberculosis – the organism that can cause TB – but this figure is surprisingly uncertain. We live in an age of increasingly sophisticated diagnostic tests and yet there is still no definitive test for TB infection.
Only around 10% of infected people go on to develop the disease (and potentially infect others) but this still means around 8.6m people develop TB and each year 1.3m die.

In adults, it is often the classic lung form of the disease, depicted in poetry, opera and literature, with a cough (sometimes bloody), weight loss and fever – symptoms that give rise to the disease’s vivid traditional name: consumption.
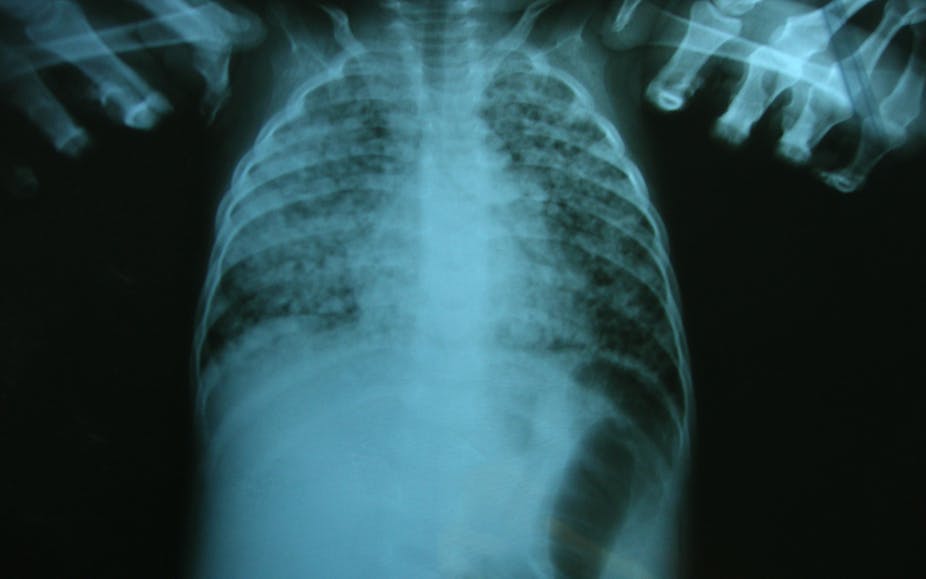
Children are particularly vulnerable to developing TB disease after becoming infected because their immune systems are immature. But tuberculosis disease in children is more changeable in how it presents – it is often not the classic lung disease seen in adults, and can be spread throughout the body or cause deadly meningitis if it gets into the brain. Because of this variety of symptoms, and due to the difficulties in obtaining samples containing the bacteria, establishing a correct diagnosis in order to determine an appropriate treatment is very challenging.
Interpreting reported numbers
It also means that knowing just how many children are affected by TB is difficult. Most estimates of burden are based on the number of cases that are reported, or “notified”, to central authorities in different countries. It can certainly be hard to make a diagnosis of TB but if a child is correctly diagnosed, it may not even be reported. Historically, there has been a perception that reporting TB in children is not important as they are not likely to be infectious to others.
There are signs that this is changing, however, and the World Health Organisation (WHO) is now encouraging countries to report child TB cases. In 2012, the WHO began to publish the first annual estimates of global TB incidence in children as part of their overall global report into the disease.
The difficulty with basing estimates on notifications is in knowing the gap between the reported numbers and the true incidence. For TB in adults, audits of clinic records, and comparisons with data from population prevalence surveys mean we have a handle on this – WHO estimates that about two-thirds of TB cases get reported worldwide.
For children, under-diagnosis and under-reporting mean the gap is likely to be larger, but there is much less evidence on which to base a figure.
Using a different model
One approach to this problem is to estimate the burden in children indirectly, starting from the estimated TB prevalence in adults. This is what we did in a study published in The Lancet Global Health. We used data relating adult prevalence to infection risks in children to model how many children become infected with TB in a given country. Data from historical studies of disease progression in children could then be used to assess how many of these children would go on to develop disease.
Mathematical modelling approaches like this avoid the need to make assumptions about the gap between notifications and incidence, but the price paid is a larger uncertainty that comes from our imperfect knowledge of the infection and progression processes.
These estimates come with large uncertainty ranges, but they do indicate that around 650,000 probably developed TB in the 22 highest TB burden countries in 2010. This means that TB in children typically makes up between 10% and 20% of the total burden in these countries, and deserves attention from public health programmes.

This modelling study also estimated around 15m children in these countries were sharing a household with an adult TB case.
This represents a huge group of children at high risk of developing TB, who are potentially identifiable. And these children could benefit from preventive medicines that reduce their chances of developing the disease.
Better numbers are a catalyst for action. Without a good idea of the number of children who develop TB each year, it is hard to set goals, assess progress, allocate resources appropriately, and motivate investment in diagnostics and treatments aimed at children. As traditional estimates based on notifications improve, together with complementary approaches like mathematical modelling, we should move towards a more complete and accurate understanding of the patterns, causes and effects of TB in children.