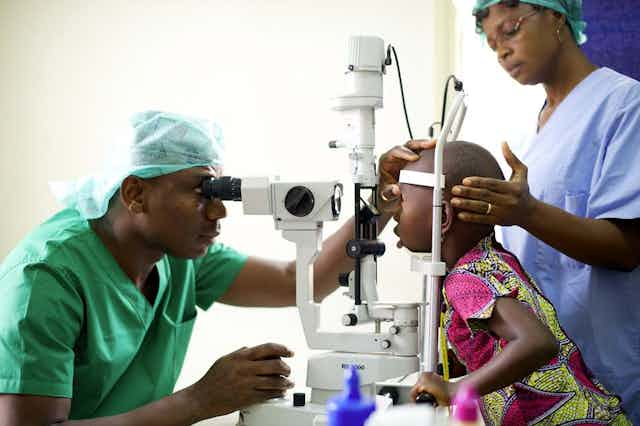
Each year in the United States more than three million people undergo procedures to remove a cataract. A cataract is a medical condition where the eye’s natural lens which lies behind the iris and the pupil is clouded. It is the principal cause of blindness in the world.
In the US, most people only experience mild visual impairment before they seek care. Insurance companies or medical aids almost always cover the cost of surgery, which amounts to a total of several thousand dollars per eye. For older patients, especially those over 60, the process is a standard – even expected – procedure.
But for patients in the developing world, the facts could not be more different. 90% of the estimated 20 million people blinded by untreated cataracts live in lower income areas where they lack access to care.
In some parts of Africa, such as Chad, Niger, Gabon, Central African Republic and Equatorial Guinea, there are fewer than 10 ophthalmologists for the entire population. France and many European countries, in contrast, have about 50 times that figure.
Cataract surgery is a two part procedure. First patients must be screened to determine if they need surgery. Then, if necessary, the surgery can be performed. Africa lacks both these resources.
The shortage of surgeons extends to Asia and some parts of Latin America. It results in millions of people going blind from a condition for which a cure exists.
Why cataract blindness is a problem
There are more cases of cataracts worldwide than there are of other eye conditions such as glaucoma where the optic nerve in the eye is damaged; macular degeneration, when parts of the retina deteriorate; and diabetic retinopathy, which is a diabetes complication that affects eyes – combined.
Cataract blindness continues to affect tens of millions for two main reasons. The first is the lack of access to care. When there is only one certified cataract surgeon in a country with several million people, there is no way all patients can receive the care they need.
In places where there are more surgeons, clinics often focus their care on those people who live in larger cities. As a result, patients from less-developed rural areas are even less likely to receive care than those living in the cities. When these patients do hear about the surgery, they often cannot afford to travel to hospitals that may be hours or even days away. In Africa, there are on average 2.7 surgeons for every million people.
Compare that to the US, where there are over 58 surgeons for every million people.
The second reason is poverty, both in terms of awareness and financial resources. Many patients in need of cataract surgery –- especially those in remote communities –- do not even know that the care exists. Those that do simply cannot afford it.
The World Health Organisation cites cataract surgery among the most cost-effective health interventions. But if patients cannot afford it or find assistance, they will never receive care.
Cheaper treatment expands access

Our work at HelpMeSee, a non-governmental organisation, is to train cataract specialists within their communities to solve this problem.
Treatment exists in the form of a cost-effective, high quality procedure called Manual Small Incision Cataract Surgery. This involves a self-sealing incision, which is what allows this sutureless surgery to be so efficient.
It costs significantly less than phacoemulsification, which is the standard in the US and requires an ultra-sound machine that needs expensive maintenance.
The small incision surgery delivers very similar results to the phacoemulsification. Surgeons familiar with other procedures can be taught the small incision surgery in two to three months.
There are two examples where our training has worked well. In The Gambia in West Africa, HelpMeSee identified more than 5 700 people in need of care. This is less than 1% of the population. But working with the country’s leading eye hospital, we expanded capacity for screening and surgical delivery.
With its smaller geography and population of about two million, we adopted a similar approach in The Gambia to what we achieved in districts in India which had about the same population size. We focused on a set geographic region, identified all those who were blind because of cataracts and connected them to the care they deserve. Once this phase is complete, the focus shifted to providing sustainable community care.
In Madagascar, where nearly 100 000 people – or less than 1% – are blind because of cataracts, our approach includes both health care policy at the government level and nationwide partnerships.
The need to improve access to care
The public health crisis of cataract blindness has not received the same coverage or awareness as malaria or polio. It should. Cataracts as a health issue will not go away. But cataract blindness can, if access to care is expanded to all those in need. Only a significant expansion in the number of specialists providing care will ensure that no one needlessly goes blind.
For the tens of millions who remain blind from untreated cataracts, a brief procedure to restore sight can return lost hope and opportunity.