The 2019 report from Canada’s Chief Public Health Officer Dr. Theresa Tam focused on addressing different forms of stigma. Included in the report was one form of stigma — obesity or weight stigma — that has proven remarkably difficult to overcome. We are hoping to change that.
As a team of researchers from across Canada, we have previously written about the harm that weight bias causes. Now, and for the first time, we are ensuring that the newly updated Canadian Clinical Practice Guidelines for obesity management include explicit guidance to reduce weight bias and obesity stigma among health professionals and policy-makers. The newly released guidelines also provide information for the public on advocating for change.
New guidelines reframe weight debate
With recommendations and key messages aimed at health professionals, policy-makers and people living with obesity, we hope that this guidance will help to reframe the weight debate. Shifting the emphasis from weight to health will help us reduce the prevalence and impact of weight bias and stigma.
The guidance is an important step forward because of the systemic nature of stigma and how different stigmas intersect, as highlighted in Dr. Tam’s report. In the United States, the prevalence of weight-based discrimination has increased by 66 per cent over the past decade, and is comparable to rates of racial discrimination, especially among women.
Our health-disrupting environment
Misrepresentations abound that frame obesity as a problem arising from a lack of willpower, or from laziness or greed. We use the language of war, viewing obesity as a battle, or something that needs to be fought.
The danger with this language is that it demonizes obesity and by extension, those experiencing obesity-related complications. This, in turn, affects their care. The new guidance seeks instead to humanize people with obesity, and ensure that they receive appropriate support.
The thing is, it’s not just about obesity. It is now well established that a complex web of factors affect every single one of us, regardless of weight status. We are all exposed to a health-disrupting environment. This manifests as excess body fatness in some, or as chronic disease markers in others.
None of us is immune to these powerful environmental prompts. Just like Sisyphus in Greek mythology was doomed to keep pushing a rock up a hill, only for it to roll back down again, our health-disrupting environment means that, as individuals, we are constantly pushing a boulder of health hazards up a ramp of social determinants.
It takes an enormous amount of cognitive effort to adopt and maintain healthy behaviours, such as being active or eating healthy foods, when everything around us is modelling the opposite. In essence, healthy behaviours are abnormal behaviours within our modern environment and unhealthy behaviours the default.
Furthermore, body weight and energy regulation are significantly controlled by genetics and neural networks, more so than our personal food and exercise choices.
Supporting health
Rather than focusing on a person’s weight status, we should turn our attention to supporting every individual to achieve their best health.
Health-care providers, and others, need to:
Become more aware of the biases they hold towards individuals living in large bodies, and ensure that individuals are not defined by their weight status but as a whole person with physical, emotional and spiritual needs. Use person-first language when communicating, as this avoids labelling people by their disease. For example, use “people with obesity” rather than “obese people.”
Recognize that obesity is a complex chronic disease, that people experience challenges with their weight for many different reasons, and that a one-size-fits-all approach to addressing chronic diseases like obesity is not only unhelpful, it is also harmful.
Counter the social narrative that consistently conflates health and weight. Weight is not a behaviour and should not be a target for behaviour change interventions.
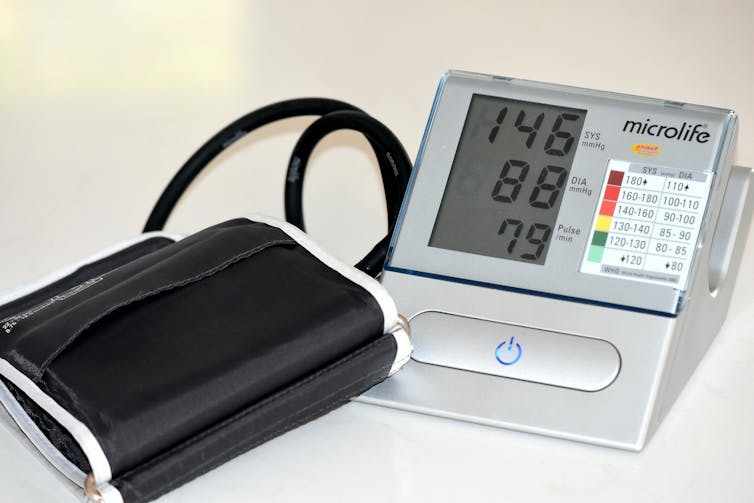
Focus on positive changes in health status (such as lower blood pressure or improved mood), or health behaviours that can be modified (e.g., increased vegetable intake) instead of the negative (such as no weight loss).
Learn to appreciate improvements in health regardless of weight status. Obesity management should not be about how much weight a person can lose or how fast a person can lose weight, but about improving health and well-being.
Dr. Tam notes in her 2019 report that “stigma affects us all. We are all vulnerable to the slow and insidious practice of dehumanizing others and we are all responsible for recognizing and stopping it.” We hope that, by including explicit guidance on reducing weight bias and stigma in the Canadian context, we can help make obesity stigma a thing of the past.
The authors gratefully acknowledge the contributions of Dr. Ximena Ramos Salas, Director of Research and Policy for Obesity Canada, to this article

