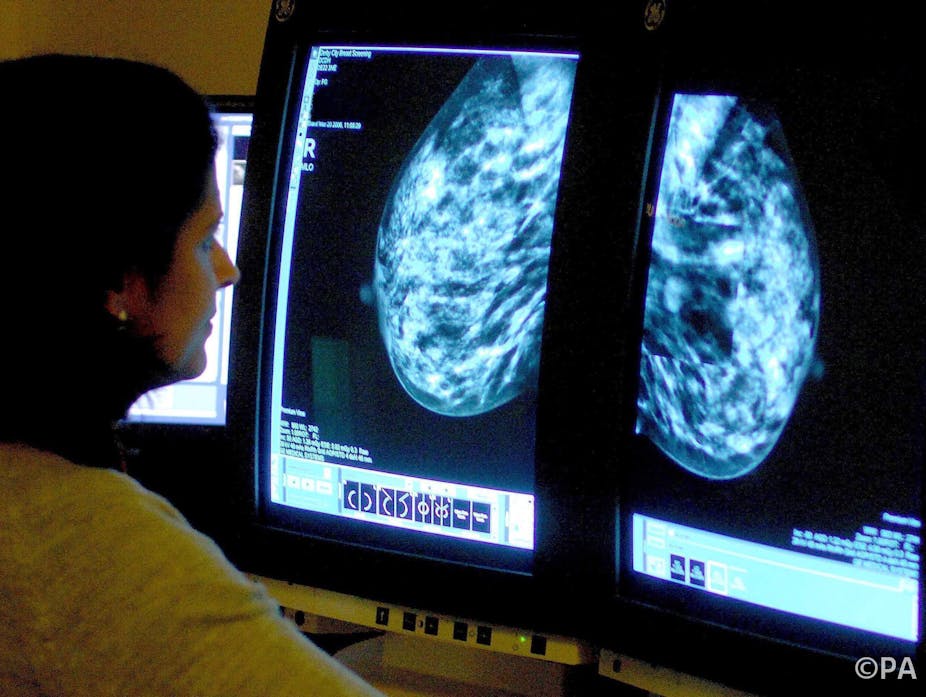
A large study on the benefits of breast cancer screening has cast doubt on the value of mammograms in reducing deaths from the disease in women aged 40-49 compared to other methods such as physical examination.
The study, carried out by researchers in Canada and published in the British Medical Journal, found that annual screening did not cut mortality rates and suggested that screenings instead resulted in a large number of cancers being over-diagnosed. It is the third paper from the team, concluding research into mammography begun in 1980.
But the findings from the 25-year study stand in stark contrast to the majority of other investigations into the benefits of breast cancer screening and some experts have called the conclusions into question.
The study compared the incidence of breast cancer and mortality in nearly 90,000 women aged 40-59 – some had received breast cancer screening, while others hadn’t. After a five-year screening period, the women’s health was then tracked for the next 20 years. Over this time the study found that 3,250 women who were screened and 3,133 in a control group who didn’t receive screening were diagnosed with breast cancer and 500 and 505, respectively, died of the disease. The researchers at the University of Toronto concluded that “cumulative mortality from breast cancer was [therefore] similar” between the two.
Over-diagnosis risks
The researchers also said their results implied that over a fifth of screen-detected cancers were “over-diagnosed”. Over-diagnosis happens when tumours that wouldn’t cause problems for a woman in her lifetime if left untreated are detected by a mammogram. This then leads to unnecessary treatment including surgery and in many cases radiotherapy and medication. The problem is that there is currently no way of determining whether or not the cancers that are detected through mammograms will be harmful or not.
Peter Sasieni, professor of biostatistics and cancer epidemiology at Queen Mary University of London, questioned the claim that other methods such as physical examinations were just as effective. “It’s definitely the case that you can find cancers on mammography that you can’t feel, and identifying tumours early on is extremely important for treatment,” he said.
While the problems around mammography sensitivity and potential over-diagnosis aren’t new, the study’s conclusions were called into question by Stephen Duffy, professor of cancer screening at Queen Mary University of London. “For the last 15-20 years, it has been the case that all the breast screening trials except the Canadian ones have shown either a significant or a strongly suggestive reduction in mortality from breast cancer with the offer of mammography screening, ” he said. There were numerous reasons why “the Canada trial results are out of line with the other trials,” Duffy said.
One major reason suggested by Daniel Kopans, professor of radiology at Harvard Medical School, was the screening technology that was used, which he said was of poor quality. In a commentary that accompanied the Canadian study, Kopans said: “Poor quality mammography does not find breast cancers at a smaller size and earlier stage and so would not be expected to reduce deaths.”
Benefits and harms
To weigh up the pros and cons of mammograms, an independent review was commissioned in 2012. It took into account earlier versions of this latest study (which had similar findings) and recognised the occurrence of over-diagnosis. Despite this, the independent panel concluded that “screening reduces breast cancer mortality” and that the UK breast screening programme “probably prevents about 1,300 breast cancer deaths every year”.
“With the publication of the latest follow-up from the Canadian trials, the situation remains unchanged,” Duffy said.
Mammogram technology has improved significantly since the trial began in the 1980s and experts argue that results are better now than they used to be. But until a sure-fire way is found of determining whether or not cancers that are detected pose a risk to women in their lifetimes, over-diagnosis and treatment will result from screening. In spite of this latest publication, experts are adamant that screening remains worthwhile and key to reducing the number of deaths from breast cancer.