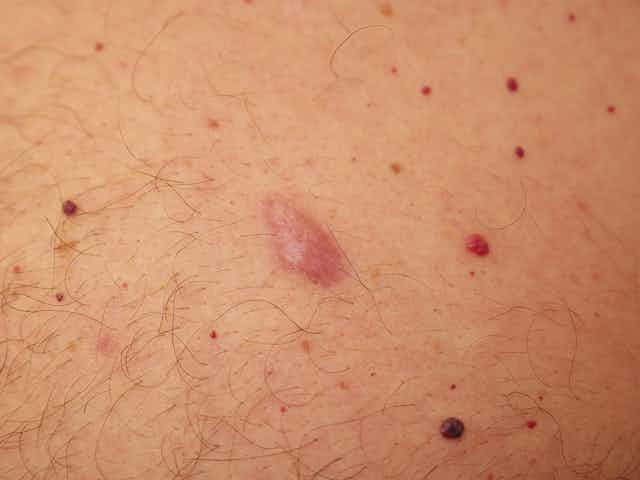
As we age, the smooth skin of childhood gives way to all sorts of mysterious lumps and bumps. In a high-UV environment like Australia, we need to be very alert to the possibility of skin cancers. But most of the skin lumps we develop will be benign. Here are some of the most common, and how to tell them apart.
Moles
Moles, or naevi, are the most common skin lesions. They are formed by a cluster of melanocytes, the skin’s pigment-producing cells. They can be brown, black, pink, the same colour as the surrounding skin, or even blue if the melanocytes are clustered deep in the dermal (inner) layer of the skin. Most moles are flat but they can also be raised.
While some people have moles at birth, they usually begin to appear during childhood and keep developing through to your 40s, when they start to slowly disappear again. The number of moles you have is partly controlled by genetics, but is also influenced by your environment. Lots of sun exposure leads to more moles, and so can using certain medications, such as those that suppress your immune system.
Moles themselves are harmless, but around 25% of melanomas arise in an existing mole. Many more look like moles in their early stages.
It’s a good idea to get any new or changing mole checked by a doctor, who will usually examine the mole with a dermoscope, a hand-held microscope that uses polarised light to see just under the skin surface. If the lesion is asymmetrical, multi-coloured or has other signs of melanoma, the doctor will excise it for further testing.
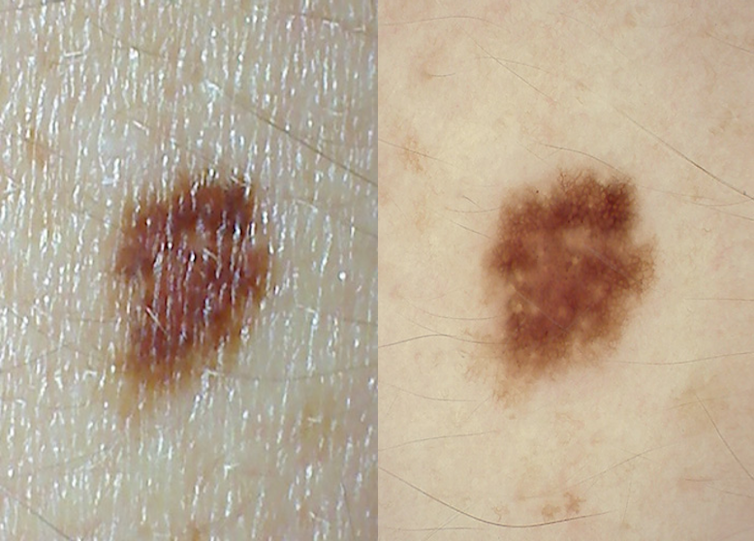
Having many moles is the strongest predictor of a high melanoma risk, so people with many moles are often advised to have regular skin checks with a dermatologist. For the rest of us, self-examinations are recommended.
Seborrhoeic keratoses
Seborrhoeic keratoses, sometimes inelegantly called senile warts or barnacles, are another common benign skin lesion. These are considered part of the normal skin ageing process.
These wart-like growths can begin to appear in your 30s and 40s. By the age of 60 around 90% of people will have at least one seborrhoeic keratosis. They can erupt suddenly after a sunburn or a bout of dermatitis, or gradually appear for no discernible reason.
If many itchy seborrhoeic keratoses erupt suddenly, it is occasionally a sign of an internal cancer. Very rarely, basal or squamous cell carcinomas arise within a pre-existing seborrhoeic keratosis. Seborrhoeic keratoses themselves are harmless, but can be prolific – some people have hundreds – and they increase in number as the years go by.
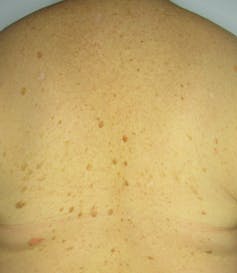
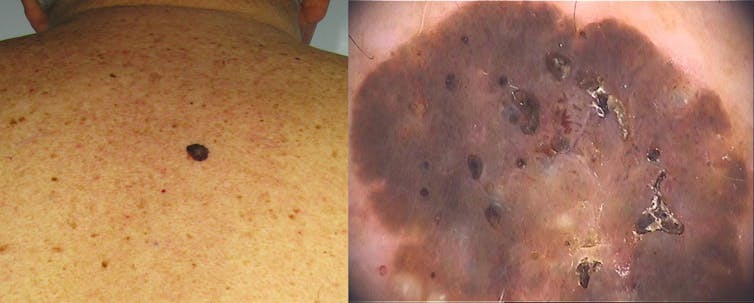
Seborrhoeic keratoses can be flat or raised, and often look as though they’ve been glued onto the skin instead of growing out of it. Their colour ranges from pale yellow to black. They can be waxy, warty or scaly, and anywhere between 1mm and several centimetres across.
Those that are dark and large can look alarming, but when seen under a dermoscope they usually have a characteristic brain-like or banksia-like appearance and are easily distinguished from skin cancers. If in doubt, your doctor will take a biopsy to investigate further, since a melanoma can occasionally simulate a seborrhoeic keratosis.
Seborrhoeic keratoses can be annoying if they snag on clothes or get in the way of your razor, and some people find them unsightly. In these cases they can be removed by freezing, cutting them off, burning, laser surgery, chemical peels or excision with scalpel or scissors.
Cysts
A cyst is a round lesion made of a capsule filled with keratin (the structural material that makes up the outer layer of our skin), sebum (the oil from our skin), fluid or pus-like material. Firm or squishy to the touch, they are totally benign. At least 20% of adults will have a cyst of some sort in their life.
Sometimes cysts form when injured skin gets tucked in to form a pocket and the maturing and dying skin cells build up inside it. Other cysts are formed when epidermal cells, normally found on the surface of the skin, proliferate in the deeper dermis and fill up in a similar way.
Some cysts form when a hair follicle, sweat duct or mucous gland becomes blocked and fluid builds up behind the blockage. Ganglion cysts form when fluid from nearby joints leaks into a capsule under the skin. Several genes can make you more susceptible to forming cysts of various sorts.
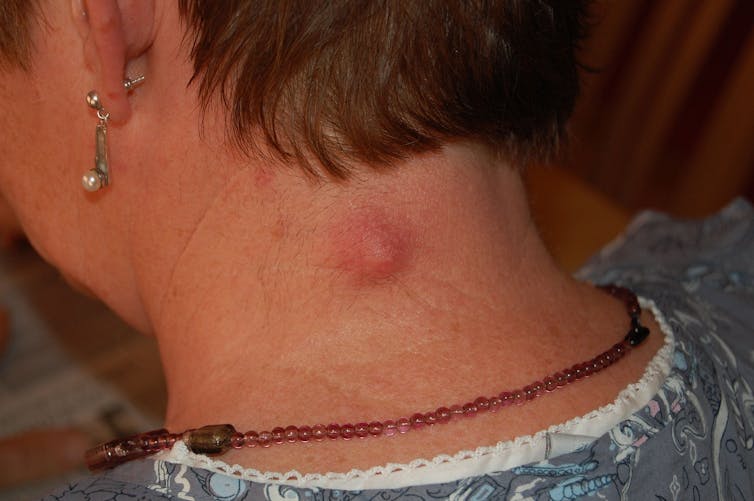
The material inside a cyst can range from watery to soft-cheese-like, and can be odourless or smelly. A central pore may be visible on the cyst, but beware of trying to pop and drain the cyst yourself – it can become infected if you don’t clean it adequately.
Usually the only way to get rid of a cyst permanently is to surgically remove its encapsulating wall. If it is only drained of fluid, it will just fill up again.
Fortunately, a dermatologist can usually remove a cyst in a short procedure with a little local anaesthetic. This is demonstrated in the weirdly popular videos of Dr Pimple Popper (which, by the way, you might not want to watch at lunch).
Haemangiomas
Haemangiomas are another benign, usually painless skin lesion, formed from an excessive growth of blood vessels in the skin. They are usually firm lumps and can present as cherry angiomas, venous lakes or spider angiomas. Depending on how deep in the skin they are, they can be red, purple or even deep blue.
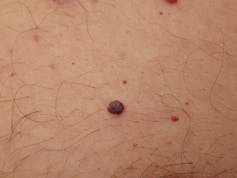
Cherry angiomas are round or oval, sharply defined, bright red bumps, usually less than half a centimetre wide. If found on the lip, they are called venous lakes.
Spider angiomas also have a tiny central red lump, but with red lines (capillaries) wriggling outwards like the legs of a spider. They usually appear on the face and upper body.
If many spider angiomas suddenly appear, it can be a sign of high oestrogen or poor liver function, but, as a rule, isolated spider angiomas are not a cause for worry.
Rarely, angiomas mimic amelanotic (non-pigmented) nodular melanomas. These need to be excised for further testing.
The rest don’t require treatment except for cosmetic reasons. In that case, the angioma can be frozen with liquid nitrogen, burnt off with electrosurgery, or treated with lasers.
Dermatofibromas
Dermatofibromas are firm small nodules, which are sometimes itchy and might be mistaken for an insect bite. In fact, most probably they also evolve from some types of insect bites.
They are usually 1cm across or smaller, seem to be in the surface layer of the skin and, if you pinch one, a dimple will appear in it. On pale skin, they range from pink to light brown, and on darker skin from dark brown to black, and can be paler in the middle.
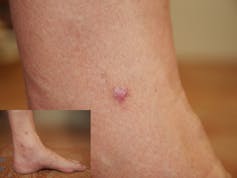
They are caused by a benign proliferation of fibroblast cells (the main cells in connective tissue), perhaps in response to a mild skin injury, but it’s not clear why this happens. The immune system seems to keep them in check, as several new dermatofibromas can appear when a person’s immune system is suppressed.
Like seborrhoeic keratoses, dermatofibromas are harmless but can be annoying. In this case, they are removed by simple surgical excision. If they are ulcerated, have recently become bigger or are unusually coloured, your doctor will excise them to check they aren’t melanomas or basal cell carcinomas.
Lipoma
Lipomas are not, strictly speaking, a skin lesion at all. Often appearing similar to cysts, lipomas are actually slow-growing tumours of fat cells surrounded by a fibrous capsule. They don’t actually grow in the skin, but in the subcutaneous layer underneath.
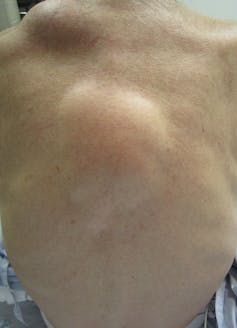
Like cysts, they are very common and not malignant. Many people with lipomas have a family history of lipomas, so there’s probably a genetic cause. Some lipomas might arise after a blunt injury to the site, but the mechanism causing that is not well understood.
The egg or dome-shaped lipoma usually feels rubbery and moves around easily under the skin. This makes them easy to diagnose clinically, though doctors sometimes use a deep skin biopsy to be sure.
Most lipomas are not painful to touch, but they can grow as big as 10cm across and restrict movement of nearby muscles or joints. If that’s the case, or you are bothered by its appearance, lipoma can be treated by surgically removing the whole tumour, liposuction to drain the inside, or simple squeeze technique, where a doctor makes a small incision in the skin and squeezes out the fat tissue.
When to get it checked
Any lump, bump or lesion on your skin is worth showing to a doctor if it’s worrying you, but there are some red flags that should prompt you to make the appointment sooner rather than later.
A newly appeared mole or an existing mole that starts growing or changing colour should be checked. If the lesion bleeds very easily – at a touch – get it looked at as soon as possible. Painful lumps are another sign all is not right.