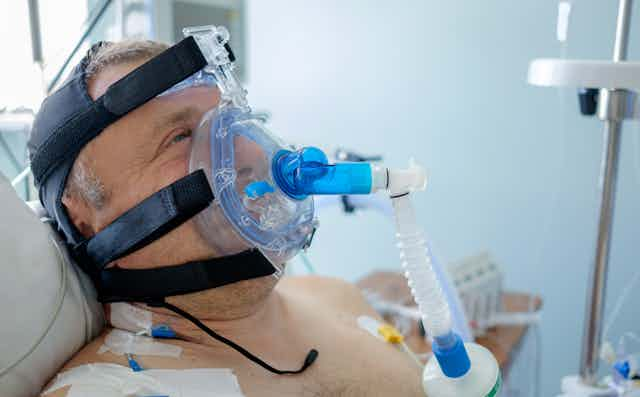
As the second wave of the coronavirus pandemic hits hospitals, the hiss and bubble of advanced respiratory support is an increasingly familiar sound on medical wards. This is because some patients who become severely unwell with COVID-19 suffer from respiratory failure and so require breathing support.
This support can be both “invasive”, where a ventilator delivers air to the patient via a tube inserted into the windpipe, or “non-invasive”, where patients are assisted using devices that remain outside the body. Non-invasive techniques are not new, but the pandemic has transformed how they are used. Previously not in routine use outside of the intensive care unit (ICU), they have become a standard of care.
With clinical opinion changing so quickly, it’s worth reflecting on how and why this has happened – particularly as the scientific evidence to back up this change is lagging behind clinical practice.
Non-invasive techniques in a nutshell
Non-invasive therapies come in two main forms: continuous positive airway pressure (CPAP) and high flow oxygen (HFO).
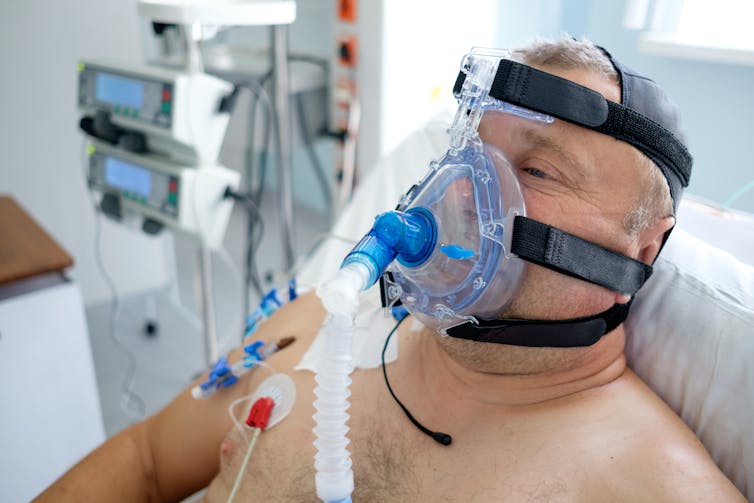
CPAP increases the pressure in the airway by using a mask, delivering oxygen more widely in the lungs and helping it transfer into the blood. CPAP is sometimes likened to breathing while facing into a strong headwind, such as out of a car window.
HFO is delivered either via a face mask or (now more commonly) through a snugly fitting nasal cannula. It provides a high flow of an air-oxygen mix, allowing exhaled air to be more effectively washed out of the lungs. It also provides a small degree of pressure to the airway, similar to CPAP.
Rapidly changing practices
As the pandemic unfolded, it became clear that conventional oxygen therapy provided routinely on hospital wards was insufficient to overcome the effects of respiratory failure for some patients. In such cases, transfer to the ICU for invasive ventilation was required. Guidance during the first wave emphasised the need for prompt action in these situations, and recommended that CPAP or HFO shouldn’t be used to delay transferring patients to intensive care.
This was partly based on uncertainties about these techniques’ effectiveness, but also because they might generate respiratory aerosols that could infect healthcare workers. However, at the same time, we began to hear frightening accounts from Italy and China of hospitals running out of ventilators or ICU beds, and of doctors having to make life-or-death decisions about who should receive treatment.
In the UK, these reports had particular resonance because of the lower number of ICU beds we have compared with many other developed nations. Suddenly, using non-invasive support might become a necessity.
But early reports also suggested that these non-invasive techniques might be effective in treating COVID-19. So, in many UK hospitals, staff with the necessary skills began treating patients with non-invasive support on non-ICU medical wards. The NHS procured more CPAP and HFO equipment, modified to minimise the viral transmission risk.
What followed was a rapid evolution and improvement of clinical practice as the pandemic unfolded. Non-invasive support that was not in routine use outside of the ICU has become a standard of care. Initial concerns have been tempered by experience on the ground, which suggests that CPAP and HFO are effective strategies to improve oxygenation and avoid the need for invasive ventilation – an intervention associated with high mortality in COVID-19.
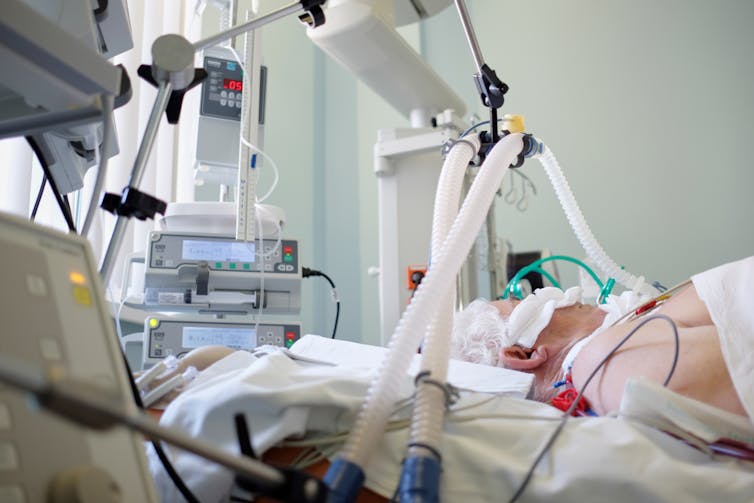
Data also emerged indicating that the infection risk posed CPAP and HFO was lower than initially feared. UK guidance has therefore been updated to support their use. Meanwhile clinical teams – particularly nurses and physiotherapists – have developed expertise in providing non-invasive support. This has been critical for patients who remain conscious, who are often anxious and frightened.
The need for caution
Despite this undoubted progress, some caution is required. ICU audit data suggests that fewer patients are receiving invasive ventilation during the second wave, and that as a result, mortality might be lower. However, it is too early to be certain about this, and other developments such as the use of dexamethasone will be having an influence.
Improvements in oxygen levels are frequently seen shortly after respiratory support is provided, and such observations have been used to make the case for CPAP and HFO. But conclusions drawn from simple observations over time can be subject to bias. COVID-19 often runs a variable course over a period of several days, with fluctuating oxygen requirements. It can be hard to determine whether short-term improvement following treatment is due to the intervention or part of this pattern of variation.
There are possible harms too. Intuitively, delaying or preventing invasive ventilation ought to be beneficial, but we don’t know if this truly results in better outcomes. Indeed, one of the reasons for the reluctance to use non-invasive techniques at the outset was the lack of high-quality evidence that they reduce mortality from respiratory failure in other scenarios.
And while CPAP and HFO are allowing the management of critically ill patients outside the ICU to become more widespread, the wards where this is being done have substantially lower nursing and medical staff ratios than ICUs. They cannot provide the same level of physiological monitoring. Management of other complications of severe COVID-19, such as heart and kidney problems, might therefore be less effective.
This is a story of rapid adaptation to a new clinical problem at scale, with improvements to clinical care shaped by necessity and experience. Many of the outstanding questions about how best to treat respiratory failure can only be answered through rigorously conducted clinical trials, and a key lesson of the last few months is that these can be successfully undertaken in the heat of the pandemic. In the case CPAP and HFO, such testing is underway in the UK through the RECOVERY RS trial – and we should wholeheartedly support it.