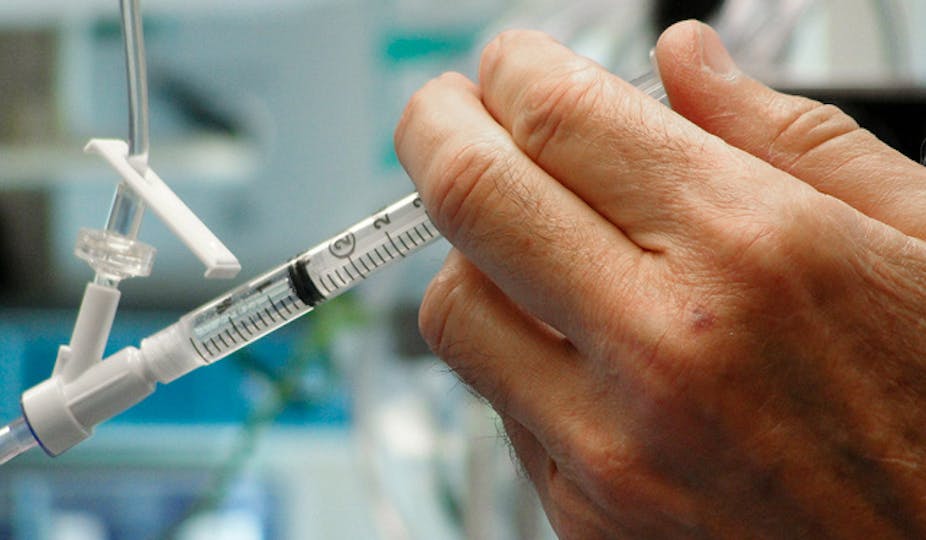
Doctors, just like the rest of the population, make personal choices about drug use. Some choose to use legal drugs such as tobacco and alcohol; others take illicit substances like cannabis and amphetamines. Doctors also have access to controlled drugs, which creates the potential for misuse of prescribed medicines.
The extent of drug misuse among doctors is difficult to assess accurately, and estimates vary widely. But compared with the general community, doctors have relatively high rates of mental illness, substance abuse, burnout and suicide. This increased vulnerability is due to a range of factors, including high-stress jobs, personality traits, characteristics of the medical culture and time pressures.
We require doctors to be adequately trained, to continually update their knowledge, to maintain a standard of professional behaviour and, since 2010, to report colleagues they believe to be impaired. But impairment of doctors remains difficult to detect.
The question of whether doctors should face random drug tests has been raised again this week – this time, in relation to the risk of abuse of propofol among anaesthetists. Propofol, an hypnotic drug used in anaesthesia, achieved fame through its association with Michael Jackson’s death. But compared with alcohol, it’s responsible for very few cases of drug misuse.
First, do no harm
In responding to the question of drug testing, let’s first identify the critical issue: the risk to patient safety when a doctor is impaired.
Impairment can be due to alcohol and other drugs, mental illness, physical illness (such as cognitive impairment due to a brain tumour), psychological and physical factors (emotional stressors, lack of sleep, pain, for example).

So how do we prevent and detect impairment in doctors to reduce the risk for patients?
Patient safety systems recognise that health-care professionals are fallible human beings who make errors. The goal is to reduce the risk of adverse outcomes through systems which detect and correct human errors.
Quality health systems have processes to ensure staff are appropriately qualified and communicate effectively – with the patient and between members of the health-care team. This allows staff to detect and correct potential risks, to monitor outcomes and identify potential problems. The organisation can also learn from mistakes and near-misses to implement ongoing improvements.
The process of employment requires checking that a doctor is qualified, registered and has good standing with the Australian Health Practitioner Regulation Agency (AHPRA). Doctors’ annual registration renewal includes a declaration that they’re not dependent on alcohol and drugs, and don’t have a mental illness which can impact on their ability to practise medicine.
Random drug testing
So will random drug testing of doctors improve patient safety? Well, it might detect recent alcohol and other drug use. But some legitimate medications might be detected in drug tests. And false positives and negatives add complexity to their interpretation.
We would also need to define acceptable drug use. For instance, is it acceptable for a shift-working doctor to use a sedative drug for insomnia?
A random drug testing policy would need to consider the response to such situations and have clear processes triggered by the detection of a positive test: how is an initial positive test handled when it might be a false positive? And how would this impact on the health care provided to the patient? Cancelling appointments and surgical lists is an inconvenience but may ultimately protect patients from harm.
There are logistic challenges in the implementation of drug testing. Drug tests need to balance sufficient frequency – to effectively detect drugs that may only remain in the body for one to three days – and the cost of testing. A negative test does not, of course, exclude impairment from other causes.
Another confounding factor is that many doctors are self-employed. So how would drug testing policies work in this context? Who would ensure that this occurs?
Clearly there are challenges in implementing these policies, some of which are unique to the medical role. But drug testing has been successfully introduced in other safety critical occupations such as pilots and mine-site workers, so it has the potential to work in the medical profession.

There are many different options for preventing patient harm; drug testing is but one. Other options that should be considered include better auditing of drugs, different medication storage systems and, perhaps most importantly, education and support programs that encourage doctors to seek help.
We’re yet to see the impact of the legislation which requires registered health professionals to report colleagues they believe to be impaired. But in the interests of patient safety, we need to consider ways of early detection, before impairment occurs. And this detection should extend further than impairment from restricted substances.
Alcohol is the drug that causes the most impairment among doctors so there’s a greater rationale to support its testing. It would also be the most easily implemented since breathalysers are commonly used and provide immediate results.
Strangely, this is the drug that appears to be immune to the calls for drug testing.