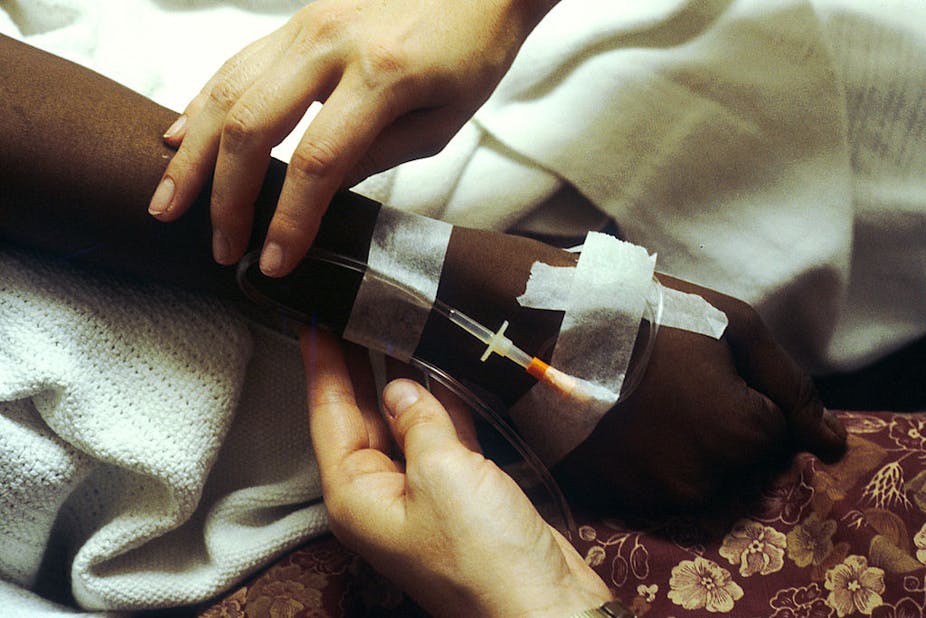
In spite of a major drive to develop targeted drugs to “personalise” cancer treatments, children with cancer still have to put up with drugs that have remained largely unchanged for decades.
Currently it’s too easy for pharmaceutical companies to focus their research only on adults. The result is that children with cancer are denied access to new developments in cancer treatments.
An EU law was introduced in 2007 to address this imbalance, but companies can too easily seek waivers to get around considering children when they develop cancer drugs. And experts have been calling for EU rules to be changed so that more potentially life-saving cancer drugs can be tested on children.
Personalising treatment
Personalised medicine is being heralded as the modern approach to treat cancer. The ultimate aim would be to identify the molecular Achilles heel of a particular cancer in a particular individual and use drugs specifically aimed at this target. The pharmaceutical industry is investing heavily in this field but only in common cancers that affect adults while rare cancers that affect children are largely ignored.
The aim of the Paediatric Regulation was to encourage drug development for children, to ensure safety information was available for younger age groups, and to develop child friendly formulations and clinical trials.
But the reality has been disappointing: most companies still focus just on the adult market and concentrate on cancers or leukaemias that are predominantly diseases of adults.
Waivers too easy
The law mandated that all applications to license a drug should include a paediatric investigation plan (PIP) that described what information the licensee would give on the safety and efficacy of the new drug in children. There was even an added financial reward – namely an extension of the drug’s market exclusivity.
But “class waivers” allow companies to argue exemptions if the adult cancer the drugs are aimed at doesn’t occur in children. But as the Institute of Cancer Research rightly pointed out – these waivers are often granted even when a drug might have a broader action that has potential applications in children.
So there have been no PIPs for cancers that only happen in children, for example neuroblastoma. This is not because the drugs couldn’t work in childhood cancer; 90% of new cancer drugs have a molecular target that could be relevant, but through a system of legitimate waivers and deferrals, these drugs can be licensed without meeting a requirement for any paediatric development.
We need the legislators to focus on biology-driven drug development, rather than disease-driven drug development. This means before granting a waiver, they consider what the drug is targeting, which will be wider than the specific disease that is being proposed, this would significantly open up the access to new drugs for childhood cancers.
No surprise
We should not be surprised that there is little motivation in the pharmaceutical industry to invest in expensive drug development programmes for very rare diseases, such as childhood cancers. But before we lay all the blame at their door, we should consider the complexities of the current legislation.
And the differences between the legislative requirements in the EU compared to the US also act as a deterrent for global companies.
There are differences in when children need to be considered in a drug’s development timeline and the EU, for example, requires a submission very early on in the process that describes in full how they intend to go about developing the drug for children, from safety trials through to the trials to determine if the drug is effective (and more effective than current treatments). This is an unrealistic expectation, both for pharmaceutical companies and those working on non-commercial trials run by clinicians and researchers who are specialists in this field.
So, while those of us who want better cancer treatments for children call for the European Medicines Agency to close the loophole in the EU law that allows waivers, we also need to be more pragmatic in what we expect companies and researchers to include in their paediatric development plans. Otherwise the 1,600 children that are diagnosed with cancer in the UK each year will be denied potentially life-saving drugs.