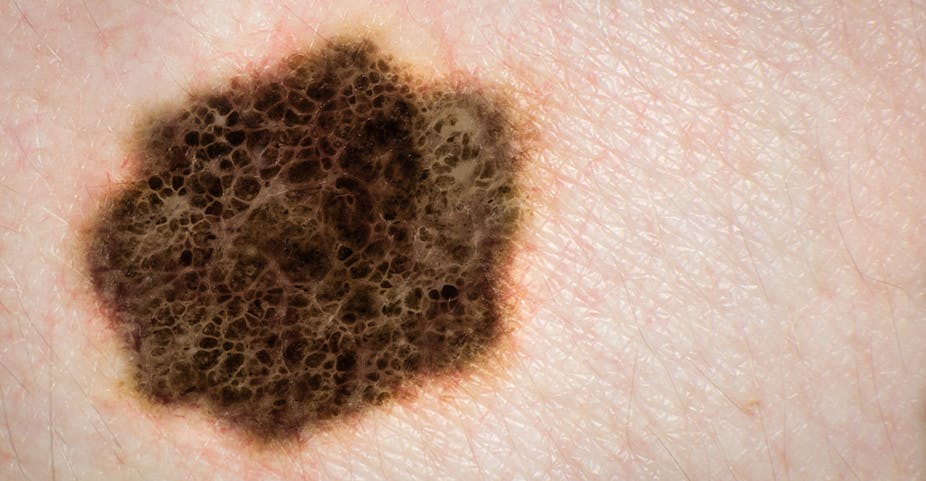
Keytruda® (pembrolizumab) is the latest drug to be registered in Australia for the treatment of widespread melanoma. This is the third class of drugs that improves survival in widespread melanoma to be registered since July 2011. Prior to this no chemotherapy drug prolonged survival once melanoma had spread.
The first of the new drugs, Tafinlar® (dabrafenib), targets an alteration in the BRAF gene, which signals the melanoma cells to divide more quickly. This altered gene was found in half of all melanomas.
The second drug, Yervoy® (ipilimumab), is an immune therapy. It is an antibody against a protein (CTLA-4) on immune T cells that stops that protein from preventing the T cells from attacking the melanoma.
Keytruda® also works by targeting a protein on the surface of immune cells that stops them from attacking the melanoma cells. The drug is an antibody which blocks the protein called PD-1 (programmed cell death 1) on the surface of the immune system T-cells. This prevents an activated PD-1 protein from stopping the immune response against the melanoma.
Initially, Keytruda® was found to prolong survival and outperform older chemotherapy drugs for patients whose melanoma had progressed after the other drugs.
Most recently, Keytruda® has been directly compared to Yervoy® in patients with advanced melanoma who had either not received previous drugs or had only previously received Tafinlar® because the altered BRAF gene was present. The 834 patients with widespread melanoma from 16 countries were randomly allocated to Keytruda®, given every two weeks or three weeks, or Yervoy®.
In one-third of those treated with Keytruda®, their melanomas shrank, compared with only 12% of those on Yervoy®. Up to 74% of those treated with Keytruda® survived to 12 months compared with 58% of those on Yervoy®.
Those treated with Keytruda® also reported fewer side effects. These commonly included fatigue, diarrhoea, rash and itch, and more serious thyroid problems and inflammation of the bowel and liver.
The results indicate that Keytruda® could be used as the first drug in the treatment of widespread melanoma.
The decision to register a drug in Australia, and thereby make it available, is based on whether the beneficial effects are sufficient to justify the side effects.
However, there is another hurdle for a new drug: whether it gets approved for subsidy by the Pharmaceutical Benefits Scheme (PBS). Evaluators assess cost-effectiveness and how it compares to other treatments. PBS subsidisation effectively makes a drug affordable for a wide population.
If Keytruda® is not subsidised, the estimated cost is A$150,000 per patient for each year of treatment.
Why so expensive? The pharmaceutical industry points to the costs of research and development, including the expense of the large clinical trials needed to confirm efficacy. Often effective patent protection may last for only 15 years before competitors are allowed into the marketplace.
However, more likely, the price is set internationally by what the market is prepared to pay and that is often the American market, which can afford to pay more than many other nations. Australia has little leverage here as it represents less than 1.5% of the world’s pharmaceutical market.
What needs to be done?
In cancer, Australia has one of the highest survival rates in the world, so until now the most important cancer drugs have been subsidised on the PBS. However, with the very high cost of each new targeted therapy, the PBS clearly cannot continue to subsidise every new drug.
The bar needs to be set so the most effective drugs will continue to be made available. Examples would include drugs for which no alternative treatments exist, or drugs that demonstrate a large increase in survival over those currently used.
As now, there should always be special funding streams for drugs for rare diseases, which would otherwise not be commercially viable.
Drugs for life-threatening diseases should be made available as quickly as possible after efficacy is established. Here it would be desirable to have a managed entry scheme so that a drug could be approved on earlier endpoints than overall survival. Response rates or disease-free survival are examples.
For such a scheme to be feasible, there would have to be agreement that the subsidy could be removed or reduced if the drug did not subsequently meet its survival targets.
We must wait to see if Keytruda® will meet the cost-effectiveness targets.