Thousands of women across the world have been left in terrible pain after being implanted with transvaginal mesh – a device to treat urinary incontinence or prolapse. How did a medical implant that has caused so much damage to these women’s bodies and lives come to be sold?
Most people probably have a good idea of how drugs are tested and approved – through clinical trials and placebos – but they probably don’t know how medical implants make it onto the market. If a headache pill that works for four hours has undergone clinical trials, what about an artificial hip that has to last for 40 years inside you?
The truth is, that for most medical implants, no clinical trials are undertaken. Instead, most medical implants are approved on the basis of “substantial equivalence”. In other words, if your new implant is substantially equivalent to an implant already on the market, then it likely gets approved.
Clearly someone has to decide how close one implant is to another. And in my experience, they can be quite different from each other and still get approved. Indeed, when independently reviewed in the US, the substantial equivalence process was said to give no evidence that “the cleared device was safe or effective”.
Three recent scandals
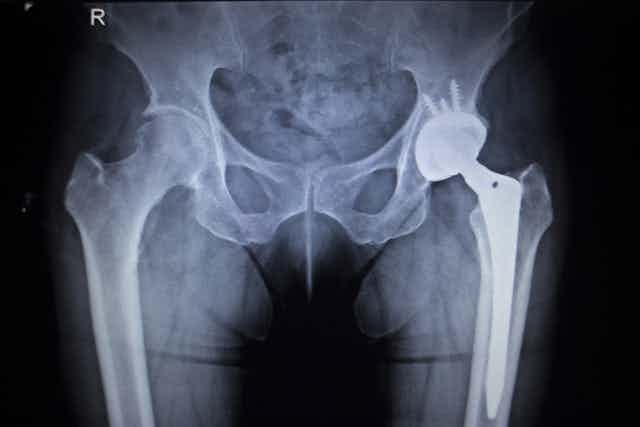
Many implant makers highlight the regulatory “burden” required to bring a new implant to market. However, despite these regulations, there have been three recent scandals involving medical implants: metal-on-metal hips, breast implants and mesh implants. Arguably, this shows that medical implant regulation isn’t working. At the very least, these scandals have left hundreds of thousands of people worrying about the long-term effects of defective implants in their bodies.

Many thousands of people have been left in pain, perhaps unable to work. Others have seen relationships break down and feel that their lives have been ruined.
There are many heartbreaking stories from patients who were told their lives would be changed for the better, not worse, and it seems reasonable to ask how this situation came about so that it can be prevented in future.
Why do we have these scandals?
I think there are three main factors. First, despite some companies’ claims of a primary responsibility to their patients, most companies exist to make a profit, which means bringing implants to market quickly and selling as many as possible. Why spend money on a long, expensive clinical trial when regulations say you don’t have to?
The second factor is the regulators themselves. These organisations are often guided by their government to work with industry to bring innovative medical implants to market, both to benefit manufacturers (who provide jobs and pay taxes) and patients. If the pull is too much towards industry, this is known as “regulatory capture”. This is where a regulator that has been set up to act in the public interest, instead advances the concerns of the sector it is charged with regulating.
It is also interesting to consider the word “innovative”; why do medical implants need to be innovative rather than safer or longer lasting or less expensive? Innovative means that a patent can be obtained, which can then be used to generate income. A safer implant doesn’t appear to carry the same potential financial reward as an innovative implant.
The third factor is a lack of transparency over the approval process. If the implant was approved in the EU, the information is confidential. This makes it very difficult to assess how an implant was tested and what the test results were. So the main judgement on an implant’s performance will come only after implantation – maybe two, five, even ten years down the line. To me, if the implant is deficient, that’s too late. By that time, thousands of people will have been implanted with a substandard device.
How to fix it
Of course, there are ways to make the system work better. For example, there could be phased introduction of new medical implants undertaken at specialist centres where all details of the implants and the procedures are fully tracked. Once the efficacy is shown after a certain amount of time, then the implant could be introduced more widely.
It is also important that regulatory capture is acknowledged. The priority for regulators should be stated as patient safety. If that means regulators stopping medical devices being implanted while patient concerns are investigated, then so be it.
Finally, transparency needs to be improved. We need to know what tests were done on implants and what the results were. With these changes in place, we might make implant scandals a thing of the past, not ongoing news.