Physicians, health care experts and the media spent considerable time focused on hospital capacity since the start of the COVID-19 crisis. Nursing homes received less attention, until thousands of deaths revealed a shocking risk for older adults and those who care for them.
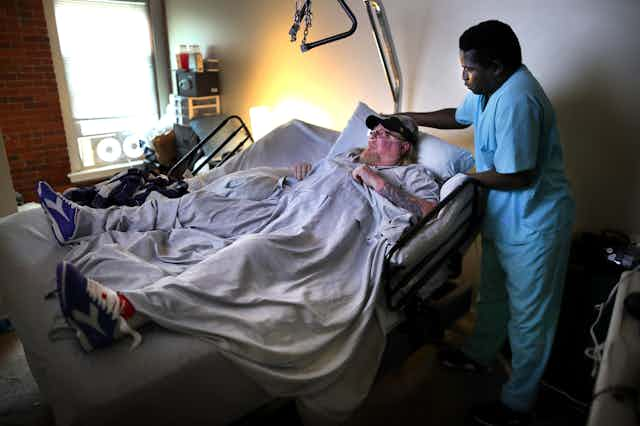
Another sector receiving little attention are home care services – direct care workers, including personal care assistants and home health aides, nurses and therapists – those who render treatment in the patient’s home. Over 5 million people in the U.S. currently receive paid home care. And now, not only must home care continue for older adults, and for those with disabilities, but many people with COVID-19 will need it too.
We are geriatricians who have worked in acute and post-acute care settings. We have all witnessed the stress COVID-19 is placing on our health care system. And we appreciate the incredible need for home care workers. But how can workers, and those they care for, stay safe? COVID-19 could complicate and compromise care for millions of people whose care already was imperiled.

An increased demand for home care
Even before COVID-19, there weren’t enough home care workers. Thousands of people with COVID-19 who don’t require hospitalization may need home care, and those who are hospitalized with the virus will need home care post-discharge. Some older adults, less willing to move into nursing homes in view of the tens of thousands of deaths in nursing homes, may opt for home care. And people with underlying medical conditions, perhaps now less inclined to go to the hospital, may choose home care too.
The immediate expansion of home care services will lessen the stress on our health system during the pandemic – and also let us envision what health care might look like after the pandemic is over.
One thing to consider is the health of the home care workers themselves.
Those caring for vulnerable older adults are often themselves vulnerable. About 90% of the home care workforce are women who have not completed college. Nearly 60% belong to racial or ethnic minority groups with a disproportionately high rate of illness and death from COVID-19. One in five lacks health insurance. And only one-third of home care workers are employed full-time. The median age for home care workers is 49 years of age; they are paid a median of US$12 an hour; and more than 1 in 4 have no health coverage themselves.
Consequently, many workers travel to multiple homes to piece together full-time work. That increases the risk of bringing the virus into the homes of frail older adults. At the same time, these essential workers are themselves at risk because of their exposure to multiple individuals. These factors limit the number of workers willing and able to provide home care.

The 10 recommendations
It’s crucial to care for the health of these workers as well as the recipients of their care. Until this is fixed, there clearly is a public health problem. Based on our research, here are 10 recommendations we think could help:
Home care workers need access to personal protective equipment (PPE).
Home care workers and their clientele need regular COVID-19 testing.
Home care workers need full-time positions with paid sick leave. Federal funds are needed, because most home care agencies can’t cover these costs.
Particularly during a pandemic, more flexibility is needed as to how care is given. Already, there have been changes: Telehealth is now allowed for home health agencies. Non-physician practitioners can now order home health services. Allowing virtual training for home health aides would go further.
The Centers for Medicare and Medicaid Services (CMS) could expand the definition of “home health” to include “personal care.” This would help clients who are socially isolated and perhaps free up the overcrowding in nursing homes. Right now, Medicare does not currently pay home care workers if they provide only personal care (e.g., bathing, dressing).
CMS could expand its definition of “homebound” so more could qualify for home care services.
Federal funding for community health workers (CHWs) should be implemented.
More home care workers need to be recruited, perhaps from industries experiencing significant layoffs such as retail and food services. These individuals would need to be trained for their new roles.
With the needs of an aging population becoming more complex, home care workers are doing more complex tasks once reserved for RNs (registered nurses) and LPNs (licensed practical nurses). As they perform these tasks, home care workers need to be trained, authorized and compensated.
Overall, there is a profound deficit in training for home care workers. With our new normal upon us, this new workforce needs a career ladder with growth opportunities. For example, these workers can obtain baseline training with additional expertise and competencies, such as how to care for a COVID-19 patient or one recovering from it, that can then be compensated.
The quality of patient lives depends on the quality of the caregiving they receive. We cannot return to past ways of doing business. The pandemic offers us the opportunity to expand the home care workforce to benefit those they serve. After all, a crucial part of valuing our older adults is to value those who care for them.
[The Conversation’s newsletter explains what’s going on with the coronavirus pandemic. Subscribe now.]