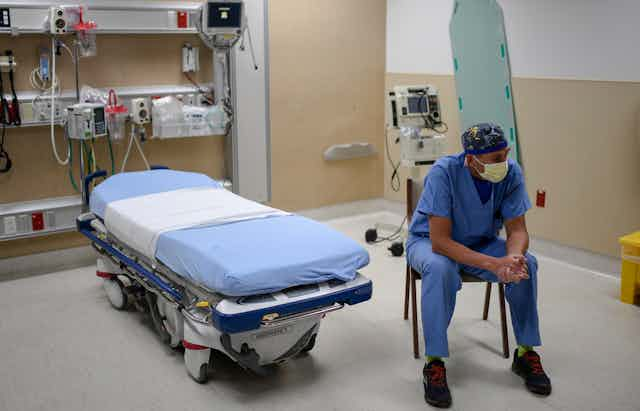
“Where have all the patients gone?” That’s what doctors in our West Virginia University hospitals began asking as the coronavirus pandemic spread.
We were prepared for a rise in COVID-19 patients, but we didn’t expect the sharp decline we saw in everyday cases. Our emergency department visits fell by half in early April, a time when we would normally see growth as flu season overlaps with an increase in trauma as the weather improves. Inpatient stays fell by nearly two-thirds during the same time period.
Did the population of a state that ranks in the bottom of most health indicators suddenly get better? Did their lung disease, heart disease and vascular disease improve?
In the emergency room, we heard the reason: “I thought I could wait this out,” patients told us.
In hospitals across the U.S. and Europe, people fearing contracting COVID-19 have been choosing not to seek the emergency treatment they need. One survey conducted in April found that nearly a third of U.S. adults had delayed medical care or avoided seeking care because they were concerned about getting COVID-19.
The numbers reported by hospitals seem to bear that out. U.S. emergency room trips for heart attacks fell 24% in the 10 weeks after the government declared a national emergency, according to data released June 22 by the Centers for Disease Control and Prevention. Visits for strokes were down 20%, and visits for hyperglycemia, or uncontrolled high blood sugar, were down 10%. Children’s vaccinations also dropped off significantly, according to CDC data, raising new concerns after last year’s measles outbreak.
This has certainly been our experience as physicians and faculty at the West Virginia University School of Medicine. The patients we saw in the emergency room this spring were a lot sicker, and the proportion of emergency room patients who needed hospitalization increased.
The costs of delaying emergency care
Delaying treatment for acute and chronic conditions comes at a cost, both human and financial.
A patient with appendicitis who gets treatment early will usually undergo laparoscopic surgery, using small incisions and a camera, and can go home two days later. If the same patient waits too long, however, and a pocket of infection known as an abscess forms, that means more complex surgery. We will have to insert a tube for several days to drain the abscess, and the patient will be hospitalized longer, in addition to going on antibiotics. In the worst case, the appendix could burst and lead to diffuse peritonitis and sepsis, a medical emergency with severe abdominal pain and low blood pressure.
Similarly, if a diabetic with a foot infection that is early in the stages of cellulitis, a painful localized skin infection, waits a week to two longer than usual, there’s a greater chance the infection has reached the bone, becoming an osteomyelitis that could require amputation.
The ultimate cost for delaying treatment can be loss of life. Data from the CDC shows the U.S. had 66,000 more deaths than expected from January through the end of April, with only about half of those linked to COVID-19. In April and May, the U.S. saw about 13% more non-COVID-19 deaths than would have been expected.
In some cases, clinics have tried to balance the risks. For example, many clinics delayed preventative care such as cancer screenings because of the risk of COVID-19. One U.S. study found an abrupt drop in preventative cancer screenings of between 86% and 94% through April. Treatments for cancer patients continued, but with hospitals taking extra precautions to protect patients while their immune systems are compromised.
The hospital experience is changing
COVID-19 is not going away anytime soon, nor will heart attacks, strokes or appendicitis.
If you feel you need to see your doctor, go. If you feel you need to go to the emergency department, call 911. It’s better than the pain and costs that can come with delay.
Your experiences during hospital visits going forward will definitely be different for a while. People arriving for hospital care that doesn’t require staying overnight should expect some kind of screening process to make sure that they are not ill with COVID-19. The health care system will encourage social distancing at check-ins, as well as in the waiting rooms, and everyone will be wearing face masks.
While these unprecedented times have upended our care processes, they also offer patients and health care systems new opportunities.
When we talk to our patients, many of them appreciate the opportunity for virtual visits, especially those at highest risk for complications from COVID-19 infection. The ability to establish virtual urgent care as well as offer many clinical services through virtual visits is here to stay.
The past few weeks have seen very significant changes at all points of patient entry into a hospital or clinic. However, clinical medicine’s fundamental principle of primum non nocere, “first do no harm,” prevails, and we remain committed to making sure that patients who need care get it on time and do not have to delay their visits or ignore their symptoms.
This article was updated June 23 with new data from the CDC.
[You need to understand the coronavirus pandemic, and we can help. Read The Conversation’s newsletter.]