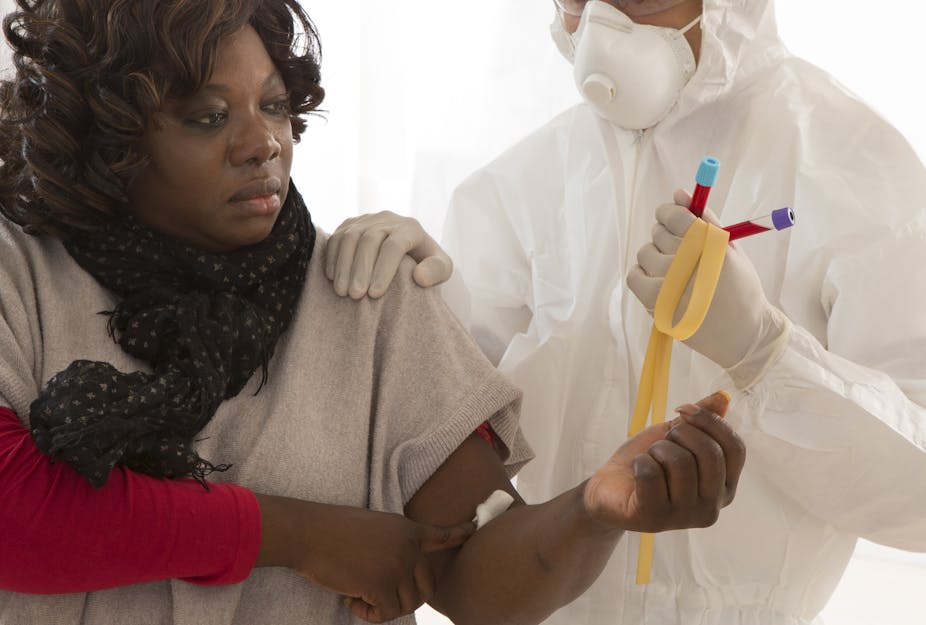
Giving HIV-positive people access to antiretrovirals as soon as they become infected is an important step in controlling the infection. The challenge lies in making sure people who know they are infected actually take the drugs.
Taking antiretrovirals results in viral suppression by lowering the amount of virus in the bodily fluid of those infected with HIV. This makes them less infectious to other people. It is key to reducing HIV infection rates.
The World Health Organisation’s new recommendation is that a person who tests HIV positive should start treatment immediately. But in South Africa, at the moment, only patients with a CD4 count of 500 receive antiretrovirals. This policy is due to change in September 2016, when all those diagnosed with HIV will be eligible for treatment. As a result it is hoped that many more people will move onto treatment, towards the estimated six million people in the country living with HIV.
We undertook a clinical trial in KwaZulu-Natal province to find out whether the rate of new infections in a certain geographical area where everyone was tested and treated with antiretrovirals would be lower than in those areas where only people with CD4 counts of 500 were treated.
The trial was one of four treatment-as-prevention studies around the world. The KwaZulu-Natal study is the first to report its findings. The others are in Botswana, Kenya, Uganda and Zambia.
It was hypothesised that the KwaZulu-Natal study would demonstrate a 34% drop in new infections.
But our study found that there was no difference in the rate of new infections between people who have access to antiretrovirals from the get-go, and those who only have access at a certain stage of immunological decline.
Instead, we found that only 50% of the people who were tested and found to be positive visited a clinic within a year of being diagnosed HIV positive. And this tells us that even when people have access to treatment, the challenge lies in making sure they collect the medicine as soon as they are aware of their status.
While the biological approach is important, it is insufficient on its own. Our study highlighted many social and infrastructural barriers to getting people onto treatment. A series of social and behavioural factors needs to be considered in the context of preventing HIV.
The findings are important because they come months before South Africa begins implementing the new treatment policy.
How we did it
The trial took place in an area around the Africa Centre for Population Health. The centre is based in the Mtubatuba, a town in northern KwaZulu-Natal. The area around the centre has one of the highest prevalence of HIV in the world: about 30%.
We identified 22 geographical clusters of 1,000 people per cluster. Everyone in that population of the cluster was recruited and tested for HIV in their homes.
The clusters then fell into one of two groups. Depending on the cluster, people were either offered treatment according to the South African National Department of Health’s current national guidelines. This is based on their immune status. Or they received treatment for HIV regardless of immune status.
The care and mobile clinics were located near people’s homes.
But there were two significant factors at play. First, even after people were tested in their homes, found to be infected and provided with local clinics to access treatment, we found it difficult to get them to attend the clinics. Only 50% of those who tested positive got to clinics within a year of being diagnosed HIV positive. As a result they didn’t benefit from early treatment and reduction of infection.
Second, a large number – even up to about 50% – described that their most recent sexual partner was outside the study area.
Reduction in viral loads
The trial participants who were tested and who got into care and were treated showed significant reduction in their viral loads. This means that they could be considered non-infectious.
The big challenge we encountered was that the number of people who got into care was lower than we wanted. This may be the explanation for the fact that the rate of new HIV infections was not affected in ways we had anticipated.
A number of factors contributed to this. One of our findings is that it was more difficult to test men for HIV and, second, it was more difficult for those men to get into care. When they got into care, they did just as well as women.
There remains a significant stigma around HIV in this population. Not wanting to be seen in a clinic may have been a contributing factor.
What’s missing
With the national guidelines in South Africa changing, the trial highlights how to best treat everyone to maximise the effect. It shows that unless this policy is associated with increased effort to provide care and treatment and encourage people to come for treatment, then the benefit of treating everyone won’t materialise.
What this means is that we need to look at whether treatment can be given in people’s homes – or if there are other things that will encourage people to come to clinics, such as mobile phone technology that reminds them to do so. Even incentives to come to clinics may be an option.
Those clinics also need to be more friendly and efficient. They must be run in a way that ensures that waiting periods are minimal so that people aren’t required to take time off from work. And the stigma issue needs to be addressed to ensure that people aren’t uncomfortable and worried about coming to the clinic.
Positive lessons
There were also positive things that came out of the trial. These included:
research teams having no challenges accessing the homes and households of all 22,000 people in the 22 clusters. This means the approach to gathering information at this level is feasible;
people accepting our approach; and
participants being happy that clinics were near their homes so they did not have to spend a large amount of money on transport to get to clinics. Transport costs were previously identified as a barrier in access to care.
The research has provided valuable insights into what needs to be done to reduce the HIV infection rate in South Africa, which remains the highest in the world. This, as the country prepares for one of the biggest changes in policy since antiretrovirals were first introduced.