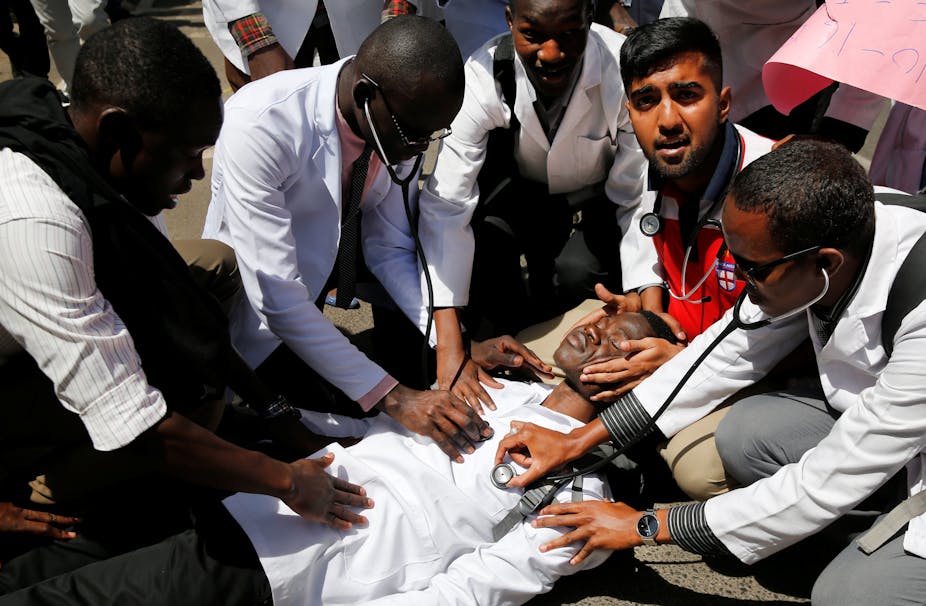
Kenya’s striking doctors are telling their horror stories on social media using the hashtag - #MyBadDoctorExperience. Many relate to emergency situations and how doctors are suffering from having to deal with poorly staffed and under-equipped hospitals. The Conversation Africa’s Samantha Spooner asked Benjamin Wachira about the state of the country’s emergency medical services and what can be done to improve them.
How are Kenya’s national medical emergency services structured and how do they work?
Kenya, a country of nearly 50 million people, provides healthcare to its citizens through a network of public and private facilities under a system called the Kenya Essential Package for Health. Only approximately 25% of Kenyans are covered by public, private or community based health insurance schemes which means that the majority have to pay for healthcare out-of-pocket.
But despite the system, emergency care remains under developed, under-equipped and unsophisticated even in private facilities.
First there’s the issue of skilled professionals.
Despite the existence of emergency medical services personnel and institutions that train them, they are still not recognised as medical professionals in Kenya. Therefore there are no national standards or regulations on their training by the government.
Emergency Medicine has just recently been recognised as a medical speciality by the Kenya Medical Practitioners and Dentists Board as well as the Clinical Officers Council. This will hopefully lead to the development of the speciality in the country. Currently, most public emergency centres are staffed by clinical and medical officers who lack specific training in emergency care.
The second big issue is resources. The majority of counties in Kenya lack ambulance services, others have contracted private companies. In most cases though, patients are transferred to hospitals by private means. For instance by car, truck or taxi. Few people make it by ambulance given their cost, scarcity and the lack of a well connected, reliable central dispatch system.
This is a big problem as over the last couple of years Kenya has seen an increased number of major incidents and disasters. The rise in global terrorism and lack of enforcement in traffic and building regulations have contributed to this. Without a coordinated response to these incidents, there is the potential of an unnecessary increase in morbidity and mortality.
The third problem is that Kenya doesn’t have an organised national emergency or trauma care system.
The draft National Policy on Disaster Management in Kenya (2009) highlights the need for emergency care systems. However there has been little progress in actually implementing these interventions despite the formation of a National Disaster Operation Centre and National Disaster Management Unit. This is largely due to the delayed recognition of the need to develop emergency care systems in Kenya as a priority.
What are the major incidents that require Kenya’s emergency services the most?
The major incidents are transport accidents, building collapses and fires.
In a research study I participated in across the country, we found that 70% of participants had personally witnessed one or more accidents. The most common trauma emergencies were; road traffic accidents, assault/mob justice, burns and blunt trauma.
How would you rate Kenya’s preparedness to deal with major emergencies?
The biggest failing is that the country doesn’t have an organised national emergency care system. Emergency centres are often poorly equipped and unprepared. Patients with different types of complaints are evaluated by health care providers with no specialised emergency care training.
Unfortunately, due to the high cost of medical treatment at private health care facilities, people are forced to turn to government facilities. Here they are met with a lack of emergency care and significant delays in getting care.
The country also lacks basic adequate resources - like ambulances. According to the World Health Organisation, there should be at least one ambulance per 70,000 to 100,000 people. The purpose of an ambulance is to reach any place within 15-20 minutes after the distress call and transport the patient to a health facility within 20 minutes. But this rarely happens.
What are the biggest challenges facing emergency services?
I would say the main ones are:
A lack of integrated emergency services that the public can easily access to receive timely emergency care.
A lack of adequate resources to handle emergencies.
A lack of specific training for emergency services personnel. For example participants of the study I was involved in felt that healthcare providers were untrained in the basics of emergency care – in many emergency situations they thought care was provided primarily by students.
Poor coordination of major incident management activities. A lack of a national incident command system and a lack of national standard emergency operational procedures often leads to uncoordinated efforts.
Are there ways to make them work more effectively or efficiently?
Access to emergency care can be improved by better delivery at health facilities and the creation of new policies at a national level.
Specifically, Kenya needs to recognise emergency services as an integral component of the healthcare system. The government needs to prioritise the development of a national emergency services policy. This should include integrated policies on major incident management.
It also needs to strengthen service provision both at national and county levels, using government and private providers for all citizens who need emergency services.
Kenya also needs an authority to regulate emergency services and there needs to be county level legislation and funding.
The country also needs to develop national as well as county communications that would support countrywide, integrated, toll free telephone access for emergency services and the dispatch of emergency services.
Finally, government must supply a framework for training personnel involved in providing emergency services.