PANACEA OR PLACEBO – A weekly series assessing the evidence behind complementary and alternative medicines.
Acupuncture has been practiced in China for over 2,500 years. During the reign of Emperor Huang Ti, some 800 hundred years ago, the practice was formalised into a medical system as part of Traditional Chinese Medicine (TCM).
TCM promoted health and well-being practices using herbs, physical therapies such as massage and exercise (Tai Chi and Qigong) and acupuncture. Mind-body interactions were recognised as central to good health, and this holistic approach was also applied to patients being treated for ailments.
TCM spread to nearby Japan and Korea then further afield to Europe via the Old Silk Road. Today, France, Austria and Germany are among the many European countries well known for their research into the scientific evidence for acupuncture and its clinical applications.
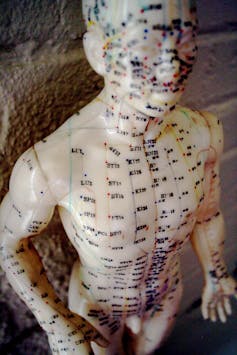
The World Health Organization (WHO) has recognised acupuncture as an effective treatment modality for over 20 years, and established an international nomenclature of acupoints to be used by the scientific community. And in the United States, the National Institutes of Health (NIH) has accepted acupuncture as a valid treatment strategy since 1997. More recently, the NIH has also supported neuroimaging research into acupuncture mechanisms.
Acupuncture is part of the teaching programs of several medical faculties in the United States and Canada. Integrated with standard medical care, acupuncture can be helpful in many clinical conditions from analgesia in painful conditions to alleviating depression.
Most importantly, its minimal adverse effects profile is attractive to both patients and health-care providers.
Current and emerging evidence
In the 1980s, acupuncture was recognised to work via the spinal pain pathways to the brain. Manual and electro-acupuncture were investigated for their usefulness for managing pain. The results were mixed and many studies concluded that acupuncture was only as good as sham or placebo – but better than no intervention.
Two decades later, the neurophysiological evidence base for acupuncture’s effectiveness is a little clearer and it has been integrated into some disciplines of medicine. There’s some positive evidence for using acupuncture in headaches and lower back pain. Acupuncture has also been shown to be useful in arthritis of the knee.
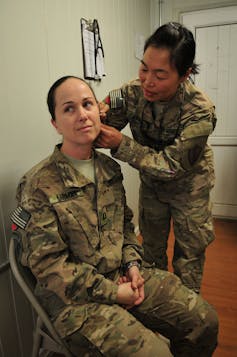
For sub-fertility, acupuncture has been helpful in increasing the “take home baby” rates, as shown by investigators in Sweden and in the United States. In cancer care, acupuncture has been shown to help in minimising the adverse effects of cancer treatment regimes. And on the battlefield, the US Defence Force uses ear acupuncture to manage pain from injuries and post-traumatic stress disorder.
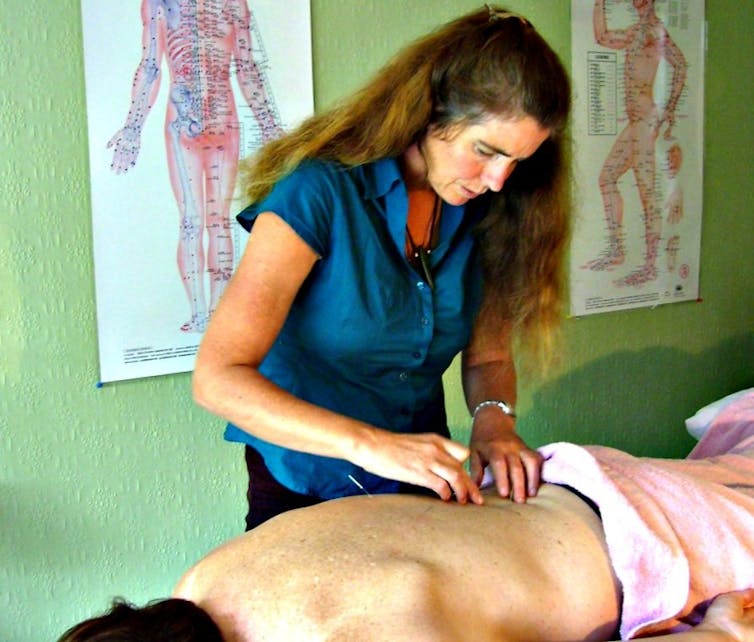
Functional magnetic resonance imaging (fMRI) research into acupuncture has uncovered how acupuncture works on the brain. The limbic-paralimbic brain region that is modulated by acupuncture is also known as the affective or emotional cortex. The affective cortex is where placebo works but the acupuncture effect has been demonstrated to be significantly greater than placebo alone in the above fMRI studies.
There has been some investigation of the properties of acupoints and classical meridians. And there’s emerging evidence that appropriate selection of acupuncture points for a specific condition is important.
The use of acupoints relevant in depression modulated mood-relevant brain regions whereas acupoints not relevant to depression did not significantly activate or deactivate the brain. Also evident is the role of acupuncture in the modulation of the autonomic nervous system.
But overall, past clinical studies were found to be inconclusive in a 2010 Cochrane review of the place of acupuncture in depression treatment. The review covered studies conducted over three decades and the variety of methodologies used in the research made the task complex.
Clinical trials in acupuncture have now been made uniform with the Standards for Reporting Interventions in Controlled Trials of Acupuncture.
Science or pseudoscience?
The dilemma confronting acupuncture researchers include study design, sample size and conducting studies under experimental conditions alone. There’s some recognition of the need to test acupuncture’s effect in primary care under “real conditions” – out in the community rather than in the laboratory.
That’s because factors such as environmental pressures, co-existing disorders and medication load are accounted for under real conditions. And this would more closely match how traditional Chinese medicine was utilised 2,500 years ago, when such factors were considered carefully before acupuncture treatment regimes were implemented.
These methodological conundrums are gradually being addressed. Measuring the effects of acupuncture is more complex than measuring drug or placebo effects. In the last few years, these complexities are gradually being recognised, carefully recorded and analysed.
In Australia, the growing scientific evidence base for acupuncture has seen its gradual integration into clinical settings from primary care to adjunct therapy in IVF, and even in emergency rooms.
There’s now a growing understanding of where acupuncture may be useful in improving patient health outcomes alongside standard medical care. And the incorporation of neuroimaging evidence to support clinical acupuncture studies may certainly be useful to more definitively evaluate the acupuncture effect in the future.
Read the first instalment of panacea or placebo:

