After five weeks in the strictest lockdown, Auckland will move to level 3 restrictions from midnight on Tuesday, for at least two weeks.
Prime Minister Jacinda Ardern said the decision was based on low community spread and an accelerated vaccination rollout. A targeted vaccination campaign will now focus on about 23,000 people in Auckland who are older than 65 but have not yet received their first dose.
GPs and pharmacies are offering vaccinations, walk-in or drive-through vaccination centres have been set up, and mobile vaccination buses are delivering doses throughout Auckland.
According to the Ministry of Health, 37% of New Zealand’s eligible population are now fully vaccinated, while 72% have received their first dose. But as our new research shows, about 20% choose not to be vaccinated, often because they remain unsure about vaccine safety.
Barriers to vaccination uptake
While the vaccine rollout has been criticised for being sluggish, it picked up pace since the start of the outbreak in August.
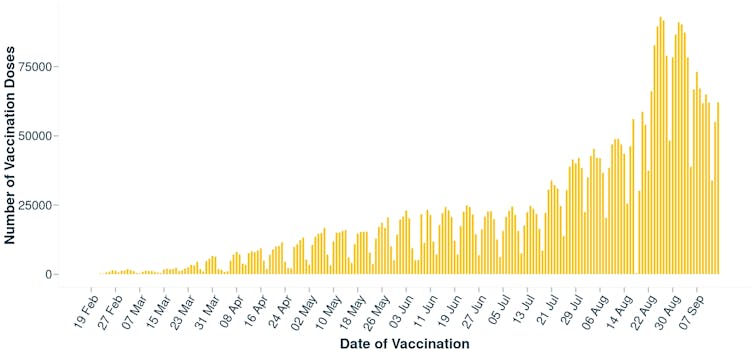
But a significant number of people continue to say they are not likely to get the vaccine. A recent report commissioned by the Ministry of Health shows 71% of those unvaccinated at the time were intending to get vaccinated. In this group, 67% of Māori and 62% of Pacific respondents said they would get vaccinated.
But 20% of unvaccinated people said they were unlikely to have a vaccine, and of those, 11% would “definitely not” get vaccinated.
A similar study in July showed only four in five New Zealanders said they planned on getting vaccinated.
Both studies point to numerous barriers to uptake, such as lack of exposure to the virus, misinformation about vaccination and lack of confidence in the vaccine. The main reasons for being unsure continue to be concerns about long-term effects, safety and waiting to see if others have side effects.
Our work, conducted between June and August 2021, examined two of these barriers: misunderstandings about the vaccine and confidence in the vaccine.
We found 76.2% of our participants identified as physically able to be vaccinated. The remainder (23.8%) identified as physically unable to receive a vaccine due to pre-existing medical conditions or philosophical views.
But of the latter group only 28.9% actually meet the criteria set by groups such as the Ministry of Health or the US Centers for Disease Control and Prevention (CDC).
The people in this group most often asserted they could not get the jab because they have asthma, want to get pregnant or their doctor or a religious leader told them they shouldn’t. This lack of understanding about who can get the vaccine is a challenge for the vaccination rollout and the government.
Vaccine confidence is key to uptake
As the rollout continues and the government pursues its elimination strategy, it must clearly address issues about who can and cannot be vaccinated for medical reasons.
When asked if they would get the COVID-19 vaccine, 70.9% of those who said they are physically or medically unable to do so said they would eventually get it if they had to.
Of those who said they are able to get vaccinated, 76.9% said they would get the jab. Split by political affiliations, 42.5% of National, 66.4% of Labour, 49.5% of Green, 67.5% of Māori Party, 40.6% of “other” political party and 73.7% of non-affiliated voters said they would get vaccinated.
In terms of demographics, 65.2% of Pākehā, 57.7% of Māori, 33.5% of Pasifika and 72.4% of the “other” group (Indian/Asian) said they were likely to get vaccinated. These results for Pākehā, Māori and Pasifika are marginally lower than those reported in the Ministry of Health study.
The critical element to understanding the patterns in our research was vaccine confidence. We found significant differences in confidence in COVID-19 vaccines between ethnic groups in New Zealand. Pacific respondents had the lowest levels of confidence, while those who identified as “other” had the highest.
Māori and Pasifika communities are particularly vulnerable to COVID-19. There is a growing anti-vax movement within some parts of the Pacific community, which Pacific leaders and communities are currently addressing.
Recent modelling has shown that unless New Zealand can get its vaccination rate up to 90% and above, the threat of large-scale outbreaks, mass hospitalisations and thousands of deaths is possible once borders reopen.
To improve our nation’s vaccine rollout, the government should expand messaging on who can and cannot get vaccinated. Further messaging about the safety of the vaccine must continue with Pacific communities.
While the government has discussed the safety of the Pfizer vaccine, it’s clearly not enough. Additional work must be done at the grass-roots level (community centres, churches) to demonstrate the safety and increase confidence in the vaccine.

