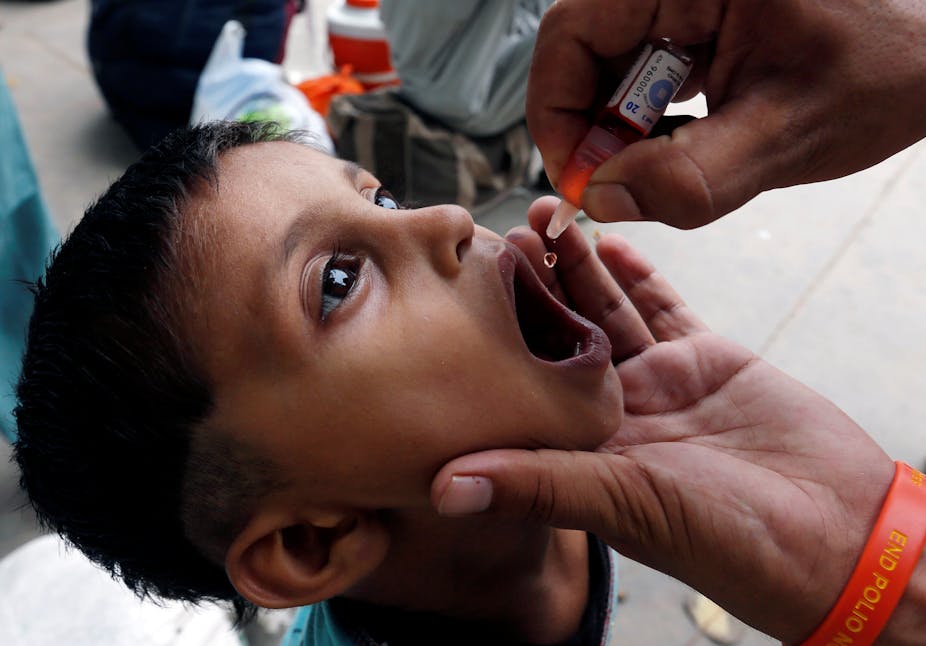
Decades of innovation, collaboration and old-fashioned sweat and tears have yielded the fewest polio cases to date, with the world on the cusp of complete eradication of polio. Yet to date, smallpox is the only disease that has been eradicated.
Those of us who work to eradicate polio have been extremely pleased that the number of polio cases has been reduced by 99.9 percent since 1988 and that we are closer than ever to eradication. The recent discovery of two cases of polio in Nigeria is very disappointing, but we know that we can overcome this challenge. Polio will be eradicated.
Eradication is no small feat. In order for a disease to be declared “eradicated,” there must be a permanent reduction to zero of cases worldwide as a result of deliberate control efforts. Eradication differs from elimination, which refers to absence of a disease in a certain geographic area. For example, polio has been eliminated in the U.S., but it has not been eradicated worldwide.
It takes years of tracking a disease and countless workers, including epidemiologists, doctors and health care personnel, to administer vaccines to eradicate a disease. Political, financial and geographical barriers often interfere.
As researchers who worked on smallpox eradication and who have spent years in the effort to eradicate polio, we believe this setback in Nigeria is small. So much already has been accomplished, and the world health community has a vast pool of knowledge to move us forward.
Humans should be the only hosts
Not all diseases are the best candidates for eradication. Commonly known diseases such as measles, mumps and rubella are considered potentially eradicable.
In order for a disease to be considered a target for eradication, it should meet certain biologic and technical feasibility criteria. First, humans should be the only reservoir (no animal hosts) and the organism must not be able to live for prolonged periods in the environment. If the organism can survive and reproduce without humans, it may be very difficult or almost impossible to eradicate.
Next, there must be a practical and sensitive way to detect the infection and an effective intervention to interrupt transmission. In other words, the disease must be so unique that a clinical diagnosis can be made with certainty.
If this is not possible, a laboratory test such as a blood test measuring antibodies can confirm whether the illness was caused by the organism for which eradication is being attempted or by another organism. A great intervention to stop transmission is a vaccine. Smallpox was eradicated through the use of smallpox vaccine.
Finally, success of the strategy must have been seen in a large geographic area.
Smallpox, eradicated in 1980, met all of these characteristics. The virus replicates in human cells only and cannot survive in the environment. Infected individuals are easily recognized by their characteristic rash. No laboratory confirmation is needed.
One dose of smallpox vaccine delivered by bifurcated needle provides long-term immunity. Success in interrupting transmission in parts of the world indicated it was possible everywhere.
Based in part on the success of smallpox eradication and also due to available vaccines effective in preventing the poliomyelitis virus, polio was targeted for eradication by the World Health Assembly in 1988.
Hidden symptoms a challenge

Similar to smallpox, poliovirus requires cell receptors expressed only in human cells. Oral polio vaccine (OPV) and inactivated polio vaccine (IPV) are effective tools in preventing infection and interrupting transmission. Industrialized countries achieved success in eliminating polio early on in the effort.
Polio differs from smallpox, however, in that most of the infections are either without any symptoms at all or with minor illness that is indistinguishable from many other causes. Thus, for polio, in contrast to smallpox, a clinical diagnosis is unreliable. While those with smallpox develop a telltale rash, only one in several hundred people infected with poliovirus displays symptoms.
Instead, there is a need to collect stool samples from suspected cases, get them to a laboratory, and assess whether poliovirus is present in the stool in order to confirm the infection as polio.
This difference requires active and intense surveillance of individuals who experience a disease characterized by the sudden onset of paralysis where the muscles are limp. This is known as “acute flaccid paralysis,” or AFP, in medical terminology.
Then virologic testing of stool and genetic sequencing is needed to understand disease dynamics. The ability to poliovirus to “hide” in populations, or circulate undetected, has made eradication efforts difficult.
The reduction of polio by 99.9 percent since 1988 has been made possible due to high coverage in routine vaccination with high-quality vaccines like OPV, and, more recently, IPV. Supplemental Immunization Activities, or mass campaigns, ensure missed children are reached and population immunity is boosted.
High-quality AFP surveillance identifies polio virus and directs immunization activities. Political will, effective management and dedicated staff make it possible, even in the most difficult of places.
In India, a place some thought would never succeed in eradicating polio, strong accountability among polio workers combined with vaccination and surveillance program quality-improvement efforts and a strong community mobilization program contributed to polio-free certification awarded in 2014.
Success is close, even with a setback

Three years of no cases with high-quality surveillance are required for an eradication certification. Africa was close. In August 2016, the entire continent had gone two years without a single case of polio. Just when spirits were high, the two cases were detected in Nigeria.
These cases were detected in Borno state and are genetically linked to a case found in 2011, hinting at what may be going on beneath the surface. This area of northern Nigeria has struggled with widespread insecurity for some time. Access to health services has been compromised. While vaccination campaigns have been conducted and surveillance has been ongoing, the quality and comprehensiveness of these activities have been compromised.
Dr. William Foege, who was one of the major leaders of the smallpox eradication effort, aptly described an important lesson from smallpox eradication. He said, “Decisions must be based on good science, results are based on good management. Continued evaluation is critical.”
Ongoing research and evaluation is necessary to any successful eradication program. The cases in Nigeria represent a setback to the program. They also provide an opportunity to reassess and reconsider.
Nigeria has built a strong polio program and was poised to react to the information of new cases. With support from the World Health Organization and other agencies, Nigerian health authorities have launched an aggressive response expected to terminate transmission successfully. Additional campaigns are planned in neighboring countries of Chad, Cameroon, Niger and Central African Republic.
Technological advances over the last few years including satellite mapping and GPS tracking have made Nigeria better equipped than ever to respond. The two polio cases detected in Nigeria do represent a hitch in the momentum of the polio program.
However, the world has never had more knowledge, experience and ability to fight back stronger and add polio to the list of diseases never to plague humanity again.
For more information on disease eradication, smallpox and polio, view the following TedEd video.