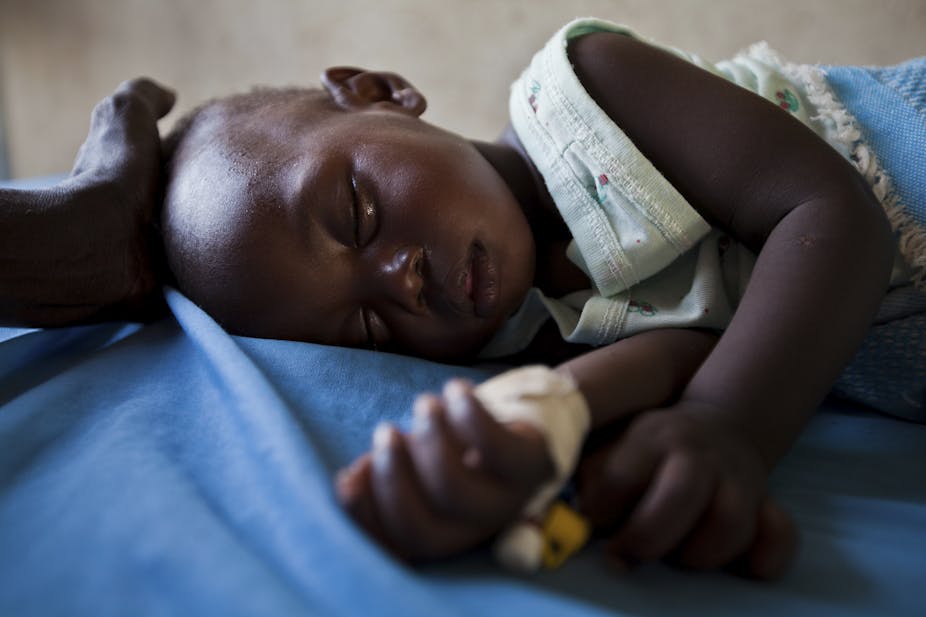
A malaria outbreak has killed 26 people in Marsabit in northern Kenya over the past one month. Over 1,000 people have been treated for the disease.
The outbreak, which is worse than previously recorded in the area for this time of year, can be attributed to a number of factors. These include a dysfunctional health service: there aren’t any qualified health workers to test for malaria and there is a shortage of drugs to treat the disease. The situation has been made worse by a four-month long strike by nurses in public hospitals.
But the main reason for the spike in cases seems to be that health services were caught off guard by off-season rains. Unlike in the highlands of Western Kenya, there are no malaria epidemic early warning systems for arid and semi-arid regions in the country.
Malaria in low risk areas
Malaria control in low risk areas like Marsabit is mainly based on prompt diagnosis and effective treatment rather than preventative measures such as the use of treated bed nets and indoor residual spraying.
Unfortunately during the rainy season, there is a surge of malaria cases and deaths due to people’s low immunity and delays in seeking treatment. Other factors that affect people being treated successfully is poor access to health facilities. It’s not uncommon for health centres to be 10 kilometres or more apart.
The availability of drugs at the primary health care facilities also influences whether patients seek medical help.
Malaria should be treated within 24 hours of the onset of symptoms. But some health workers in low risk malaria areas are not familiar with the symptoms. Improving malaria diagnosis should be a top priority in all rural health centres.
On top of this is the fact that facilities are poorly staffed. Managing malaria relies heavily on functional health facilities. These health facilities rely on skilled workers such as doctors, clinical officers, nurses and laboratory staff. The ongoing four month nurses’ strike has affected health services. Patients have been forced to go to private facilities and those that cannot afford to pay return home unattended.
Additional challenges that communities in Marsabit face is the fact that there’s poor drainage which increases malaria mosquito breeding areas. Drains should be properly designed and maintained to ensure that water flows away quickly, smoothly and is properly disposed.
Climate change and increasing malaria cases
Climate change is predicted to increase the severity of droughts and floods. This increases the risk of epidemics and outbreaks. Arid lands are prone to flooding and their aquatic systems have become reservoirs of diseases like malaria and cholera.
Changes in climatic conditions have also led to an increase of malaria cases in the Kenya’s east African highlands. Highland areas were considered free of malaria cases during the 19th century. But in the last two decade malaria has spread to the central Kenya highlands including Nyeri county which is 1,800 metres above sea level. The annual temperature has increased from 17.1°C to above 18°C which is suitable for local malaria transmission.
Moving forward
There should be functional health facilities countrywide to effectively control malaria. This can be done by ensuring that an effective vector control programme and active field based malaria surveillance programme are in place. This complements the existing passive health facility surveillance system.
The surveillance system should be designed to identify malaria transmission hot spots for the roll out of preventive measures like insecticide treated bed nets or indoor residual spraying. The use of long lasting chemicals that kill mosquito larvae to discourage breeding in homesteads should also be explored more keenly.
Community based health facilities should be improved to avoid long distance travels to seek health services. Enhanced public health education may also contribute to more people recognising the malaria symptoms and seeking treatment immediately. It could also reduce reliance on ineffective herbal medicines.
The use of radios and other forms of communication should be used to educate people about impending malaria outbreaks. Residents could learn to associate unusually heavy rains and flooding to an expected malaria outbreaks so they can take precautionary measures.
And the feasibility of increasing mobile health clinics in remote arid areas should be explored.
A combination of these actions would help minimise malaria outbreaks.