The adverse effects of maternal smoking during pregnancy are well known. Pregnant women who smoke are at higher risk of miscarriage, fetal death, prematurity and low birth weight. Smoking during pregnancy also affects the health of the child, as it increases the risk of asthma, psychiatric disorders, and obesity.
Even if pregnant women are aware of the health risks, they may continue to smoke. Nicotine replacement therapies, such as patches, appear to be less effective for pregnant women than in the general smoking population. Other support methods, such as counselling by specialists or cognitive-behavioral therapy, do not work well for pregnant smokers. Thus, 25% pregnant women smoked at least occasionally (and 22% were daily smokers) in France in 2017.
This long-standing trend is too high given the health risks for the newborns and the mothers. It is therefore necessary to explore other therapeutic avenues to help pregnant smokers quit. Economic theory indicates that a financial reward can lead to a change in health behavior.
Why would providing financial rewards change a health behavior?
Although smoking is above all an addiction, smoking cessation, like any other decision, is the result of a trade-off between the costs such as the loss of the satisfaction derived from smoking and efforts required to stop, and the benefits such as the money saved from not buying cigarettes and the perception of health improvement due to smoking cessation.
Providing financial rewards to quitters could compensate for their efforts and loss of satisfaction derived from smoking. The financial rewards would affect the trade-off such that the benefits of quitting would outweigh the costs.
Would it then be effective to offer a financial reward to help pregnant women quit smoking? To find out, we set up a randomized trial involving 460 pregnant women in 18 maternity wards in France. Our study, published in the British Medical Journal, aimed to test the effectiveness of conditional financial incentives for smoking cessation in pregnant smokers.
The participants, all in their first trimester of pregnancy, were randomly assigned, into two groups of equal size: a financial incentives group receiving financial incentives conditional on abstinence and a control group that did not. Monthly face-to-face visits were planned that included routine medical and smoking cessation counselling up to the end of the pregnancy. At each visit, the pregnant women met with health care professionals specifically trained for smoking cessation skills.
The participants’ smoking abstinence was assessed by self-report of smoking, and by a test measuring carbon monoxide level in the expired air, a standard measure of smoke exposure. At each visit, participants of the financial incentives group received vouchers whose amount depended on their current abstinence, and on their past abstinence. The more times they were abstinent, the larger was the amount of financial rewards. The maximum amount that could be earned in the study was 520 euros. Each 20 € voucher could be redeemed in many shops (including groceries, childcare equipment, etc.) but they could not be used to purchase tobacco or alcohol.
The financial incentives schedule was specifically designed to encourage continuous abstinence throughout pregnancy, as only continuous abstinence might have a major impact on the newborn’s health.
Financial incentives doubled the number of pregant women who stopped smoking
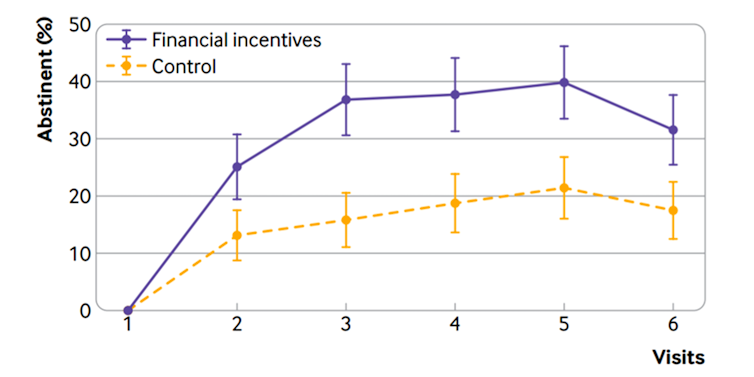
Financial incentives conditional on abstinence helped women quit smoking throughout their pregnancy and improved some major birth characteristics. With no financial incentives, 7.42% of the participants quit smoking throughout their pregnancy. Among those who benefited from financial incentives, this rate reached 16.45%. Hence, financial incentives were associated with doubling continuous smoking abstinence rate. The figure below shows that smoking abstinence was also systematically higher at each medical visit in the group that received financial incentives.
These results translate into better health outcomes for the newborns. Newborns were less likely to have a low birth weight, a known predictor of perinatal and infant adverse health events. Poor neonatal outcomes (transfer to neonatal unit, convulsion, malformation, and deaths) decreased by 5.3 percentage points between newborns of participants who were in the financial incentives group compared to those in the control group. The intervention had no effect on prematurity.
Benefits long after pregnancy
Would public health authorities implement financial incentives into the health care routine of pregnant smokers? Our results show that providing financial incentives conditional on abstinence is effective in increasing smoking cessation rate throughout the pregnancy and improve birth characteristics. But the evaluation of the impact of this measure should not be limited to this period of life. Healthier newborns may also become healthier children then adults.
Before choosing to implement such an unusual policy, public decision-makers may ask themselves how it would be perceived by the general population. We had precisely evaluated its acceptability before carrying out our study, by surveying a representative sample of the French population. More than 50% of respondents were in favor of this type of policy. As other studies from other countries have shown that acceptability of financial incentives increases when proof of effectiveness is provided, we are confident that this policy could be widely accepted in France.


