The COVID-19 pandemic is not the only crisis facing the health-care system right now. Vaccines have begun to offer hope that the pandemic will eventually wane, but another potentially devastating issue looms: By 2030, the World Health Organization projects a worldwide workforce shortfall of about 18 million health-care workers, with deadly consequences for patients, economies and our communities. We must focus on those who deliver care if we have any chance of tackling this shortfall.
I recently completed a study that looked at how health-care leaders foster psychologically healthy and safe workplaces, specifically how they address the fourth aspect of the Quadruple Aim: caring for providers.
The Quadruple Aim builds upon a well supported trio of goals already adopted by health-care organizations worldwide — better health, better care experience and better value for money — by including the well-being of health-care providers as its fourth objective.
As a primary care researcher I was particularly interested in what supports were in place for family physicians, whose burnout rates are alarmingly high. As independent professionals, they are often left to fend for themselves when it comes to mental wellness.
Leadership that is too far removed from front-line service delivery often cannot see the stressors. However, work satisfaction, stress and burnout are associated with attrition and contribute to a shortage of doctors.

The pandemic has fuelled public interest in the health-care system, but will it be enough for leaders to see the gravity of the situation and act? Leadership is needed in order to cultivate environments that limit the stressors that affect job performance, not only at a system-wide policy level, but also at the organizational level.
Leaders have not just a moral responsibility but an obligation to decrease the liability that is associated with an unhealthy work climate. A positive workplace culture is one that enables health-care workers to feel significant and purposeful in their work.
The front lines of COVID-19
The pandemic brought health-care worker roles to the forefront. Pot-banging, applause from balconies worldwide and signs of appreciation for front-line health-care workers were everywhere early in the pandemic. Soon after, articles related to exhaustion, burnout and mental distress were abundant.
Read more: Heroes, or just doing our job? The impact of COVID-19 on registered nurses in a border city
Health-care professionals are at greatest risk of exposure to the novel coronavirus and are witnessing first-hand its human toll. Many front-line workers are suffering moral injury, a term used to describe soldiers and firefighters after battling the enemy and flames.
In areas where resources were already limited, staff shortages managed before the pandemic now present as perilously dangerous situations. The gaps in health human resources are now crater-sized holes that won’t easily be fixed.

This type of “wicked” problem — those with complex social and policy aspects and conflicting priorities — calls for multiple solutions that require effort at all levels. Governments and health-care organizations have critical roles here.
Addressing the pipeline of workers means increased attention on education and training, but this means nothing if we don’t retain those workers. This requires significant focus on the workplace. Psychologically safe workplaces are those where people are at the top of their game, using their skills wisely, and where people want to come to work each day.
Leaders at all levels are tasked with ensuring that those who care for others are also cared for. Entrepreneurial thinking, seeking innovative solutions and looking to other countries to gain from what’s working elsewhere can guard against reverting back to same old, same old once this pandemic has passed. Now is the time for leaders to recognize the urgency of health human resources and double down on efforts at retaining professionals.
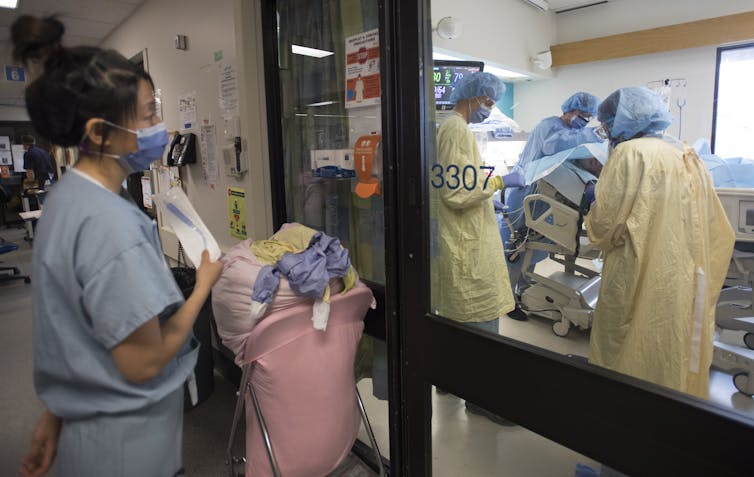
Those attracted to a profession in health care are not lightweights. Long hours, difficult work and dealing with challenging patients are anticipated in advance, but they pale in comparison to the rewards that come with patient care.
If, however, professionals are not supported in their work, challenged and given opportunities to develop or to perform at their best, then motivation decreases. How can you care for others when the system — the organization you work in — seems not to care for your well-being?
The looming health-care workforce shortfall requires a collaborative approach. The answers will not be easily found but that doesn’t mean we stop looking or stop asking the hard questions. In fact, we must ask more and fast. Let’s not let myopia get in our way. Let’s all get better glasses and look into the distance collectively.

