
Articles on health system
Displaying all articles

National Cabinet is meeting today to discuss hospital funding, and the interconnected issues of NDIS reform and GST allocation. But how are hospitals actually funded? And what’s GST got to do with it?
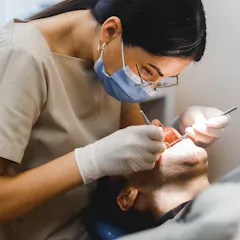
Access to dental care in Australia is worse than ever and is simply unaffordable to many.

Publicly funded primary and home care should be accessible to all older adults, regardless of where they live.

Each encounter that health-care students have with patients and families helps them understand real-world patient needs. That means all Canadians have a role in educating future health-care providers.

Now is the time to learn from the COVID-19 response through an action-oriented independent inquiry focused on accountability. Reforms to data generation, access and use are essential.

Health outcomes continue to be influenced by geography, with local communities having to plug gaps in services. The health reforms offer a chance to strengthen local networks to respond better.

There are concerns about how health data are used, but research shows support for uses with public benefits by health-care providers, governments, health-system planners and university-based researchers.

Immigration might be making it easier for doctors to enter New Zealand, but if the licensing process doesn’t change we still risk losing much-needed skills to other countries.

Hospitals are struggling, with ambulances ramping outside emergency departments and patients facing long waits for care. But doing more of the same won’t fix the problem.

Adding more beds won’t fix emergency department pressures. Neither will one-size-fits-all processes. But improving patient flow and addressing staff shortages might.

To prevent a shortage of health workers, public expressions of appreciation need to be backed by policies that provide dignity, decent working conditions, accountability and appropriate remuneration.

The need to transfer 2,500 COVID-19 patients around Ontario, and bring in extra doctors from other provinces, exposes two fallacies about Canada’s health-care system.

There are many initiatives around Australia designed to keep people with chronic conditions out of hospital. But to take these further, the health system needs a ‘license to innovate’.

Structural stigma is in the rules, policies and procedures of organizations and society. It’s reflected in systems that treat people with mental illness as less treatable or less deserving of care.

People living in long-term care facilities have been disproportionately affected by COVID-19 in Canada. A new report analyzing long-term care around the world assesses Canada’s pandemic performance.

A loose patchwork of measures and systems has left millions at risk of slipping through the cracks as the pandemic’s economic downturn hits.

Fear of contracting coronavirus in hospital means people could be suffering in silence at home without getting the essential care they need.

Climate change is anticipated to cause a rise in the incidence of several diseases in sub-Saharan Africa.

Sharing expertise and experiences of different health and social care professionals can improve health care.
