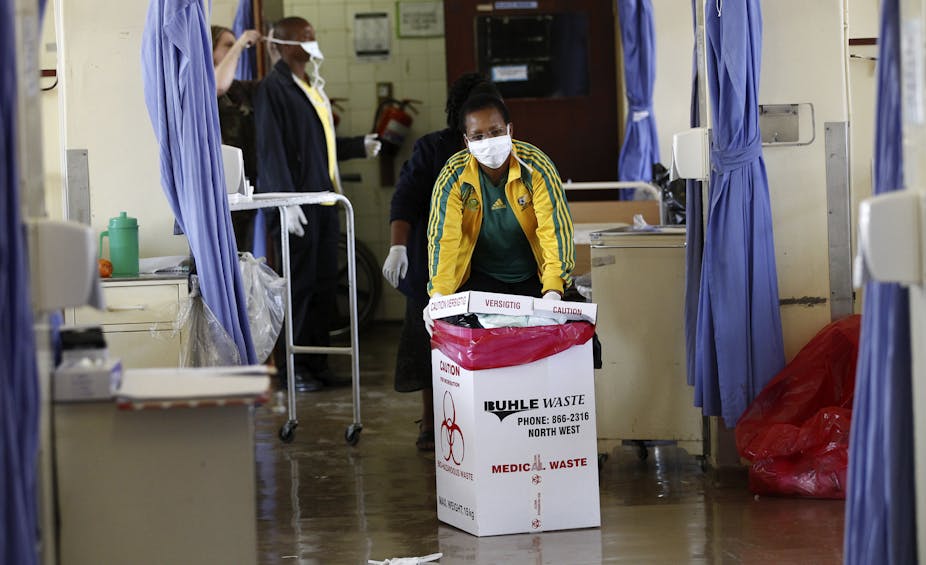
Moderate strides have been taken to make South Africa’s public health services accessible and affordable. But problems of quality persist. Evidence of this is that people still prefer private healthcare providers.
Post-1994, the emphasis has been on making healthcare services more available, and payment systems have been redesigned to increase affordability. This has seen an increasing share of government spending channelled into public health care.
But this fiscal shift has not made big improvements to South Africa’s health. Many critical health indicators, such as infant mortality rates and life expectancy, are below those of other middle-income countries that spend much less on health care.
Availability and affordability interventions are largely aimed at achieving universal health access. “Health for all” is one of the goals of South Africa’s National Development Plan. It is the main aim of South Africa’s pending major health reform – a national health insurance plan.
The government has taken a supply-focused approach to reducing health inequities – an appropriate approach in view of the extreme polarisation of the country’s private and public healthcare systems. But the focus on availability and affordability has overshadowed an equally critical issue – the demand side of access. In other words, what do people want? Do South African consumers find the public health services acceptable?
Acceptable levels of service
About 60% of those who attended public health facilities were satisfied with the service they received, irrespective of their illness, injury or socioeconomic status. However, acceptability is subjective and therefore hard to measure. Differing expectations of service levels, based on prior exposure to private health care, make economically empowered individuals more likely to complain than their less affluent counterparts. This bias could skew the findings of the analysis.
The “very satisfied” responses in the GHS data showed that the poor were apparently more satisfied with services than the more affluent. But because these data are self-reported and subject to bias they should be interpreted with caution. More rigorous analytical techniques and research methods are needed if we are to understand patient satisfaction levels.
Some people preferred to consult a private doctor rather than go to a public health facility. Clearly they opted for what they perceived to be better quality. The validity of this perception is debatable though. It can be argued that public health facilities are better equipped and their staff more experienced than private doctors when it comes to tuberculosis and HIV/AIDS treatment.
Levels of acceptable service could be gauged by complaints in the GHS about dirty facilities and rude staff. This was the subject of less than 15% of the complaints about public health facilities, with incivility being a bigger issue than uncleanliness.
These complaints came more from the affluent than the poor, perhaps implying different expectations about cleanliness and friendliness and different norms for the appropriateness of complaining about a “free” public service.
The private sector
More than 95% of the respondents felt public health facilities were affordable. This was expected, as primary health care is free for all and public healthc are is free for children under five and pregnant women. Other public health services are billed according to ability to pay, and certain services are offered free of charge to select groups.
Yet a study of the general household survey data showed that public health care is perceived as an inferior good. Even some of the poorest and most marginalised are prepared to spend their own money to see a doctor, although the services of their nearest clinic are virtually free.
While affordability remains an issue, it was not the main reason that stopped people from consulting a healthcare provider when ill or injured. But it was clearly more of a barrier for black people than for white. This highlighted a disturbing public-private split along race lines.
Affordability was the main reason why people did not join a medical aid. A large proportion – irrespective of socio-economic status – still paid personally for health care, albeit very small amounts proportional to household income. Encouragingly, this trend decreased for all race and socioeconomic status groups during the period under review.
Change is needed
A multi-dimensional approach to interpreting access to health care has gained traction in recent years. But most of the interventions to improve access remain supply oriented.
Access to public health facilities seems to be fairly equitable and well targeted in terms of affordability. The same cannot be said of availability, and particularly acceptability, which are lagging behind.
The government must continue to increase physical access to health care, especially in rural areas. Public health role-players must use resources efficiently to deliver a high quality service that all consumers will find acceptable.
Failure to do so could undermine health policies designed to achieve “health for all”. Particular attention must be paid to the overlooked and under-researched issue of acceptable levels of service. The current scenario does not bode well for South Africa’s major health reform – the implementation of the national health insurance plan.