
Articles on Health reform
Displaying 1 - 20 of 99 articles

We now have a sensible pathway to improve access to health care, using the skills of nurses, pharmacists and GPs appropriately.

The Māori Health Authority is gone, but a law remains that puts primary focus on reducing health inequities – meaning the government may struggle to bridge the gap between rhetoric and policy priority.

Rather than bold reforms that will safeguard Australians’ aged care services into the future, the taskforce largely recommends tidying up and keeping the status quo. And getting users to pay more.

Australia’s aged care system is undergoing significant change, but is still governed by an act more than 25 years old. Can the government meet its mid-year deadline for the next round of reforms?

National Cabinet is meeting today to discuss hospital funding, and the interconnected issues of NDIS reform and GST allocation. But how are hospitals actually funded? And what’s GST got to do with it?
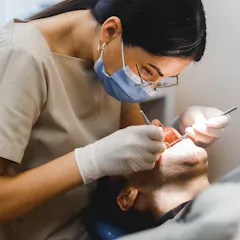
Access to dental care in Australia is worse than ever and is simply unaffordable to many.
Yes, savings from increased participation in private insurance outweigh the costs the government incurs by subsidising private health insurance rebates. But rebates can be better targeted.

Nurses make up more than 50% of the health workforce and have untapped and under-used skills that could ease the skills gap in our health system.

A new review of Australian health care workers’ scope of practice should focus on expanding pharmacists prescribing for stable conditions and long-term medications, under the direction of a GP.

MyMedicare is a new voluntary scheme that allows patients to register with their usual GP. How will it work? And how might it benefit patients? Here’s what we know so far.

The big news on budget night was a tripling of the bulk-billing incentive. It’s hoped to stem the decline in bulk billing – but it’s unclear if it will increase it.

The Pharmacy Guild head wept at the thought of pharmacies losing income from a change that allows people with chronic diseases to halve their prescription costs. What’s going on?

In Australia’s bulk-billing ‘deserts’, it’s incredibly difficult to find a doctor who will bulk bill. The government should step in to support or set up clinics so locals have access to health care.

Health outcomes continue to be influenced by geography, with local communities having to plug gaps in services. The health reforms offer a chance to strengthen local networks to respond better.

New research suggests GPs aren’t routinely defrauding Medicare, and in fact have saved the system hundreds of millions of dollars by under-billing.

Medicare access could be restricted to GPs who agree to bulk bill all patients, while allowing those who don’t bulk bill to rely solely on out-of-pocket payments.

More Australians are delaying care or going to emergency departments because they can’t see a GP. Here are six reasons why.

A new Grattan report recommends making general practice a team sport, using the skills of other clinicians and health-care workers.

If we want people with complex care needs to prioritise their health, cutting patient fees, providing flexible hours and paying attention to their social circumstances would be a good start.

How can we get better primary health care access, quality and affordability that Labor has promised? We need to learn from what’s worked and failed overseas.
