
Articles on PrEP
Displaying 1 - 20 of 48 articles

When appropriate care is available, several studies have shown, gay Black men are more likely to test themselves for HIV and engage in less risky sexual behaviors than gay men of other races.

Two-thirds of new HIV infections are among gay and bisexual men. Although cases have decreased among white men, they have stagnated among communities of color.
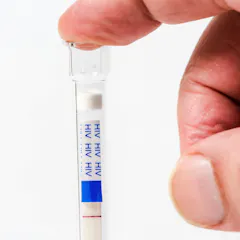
Many people at heightened risk for HIV have never been tested. Those who have self-tested for HIV often don’t go on to receive care or change their sexual behavior.

On the basis of government appointment technicalities and religious freedom, Americans may lose free coverage for cancer and blood pressure screenings, HIV prevention medication and other essential services.

The next step in HIV prevention — long-acting injectable pre-exposure prophylaxis (PrEP) — is not yet available in Canada, a year after its approval in the U.S.

Dec. 1 marks World AIDS Day. Canada has the tools and means to end the epidemic. The question remains, are we up to the task?

Experts across the board have identified inequality as a major challenge to efforts to end AIDS.

The benefit of an injectable product is that it avoids the adherence issues related to taking a pill daily.

Some countries, like Kenya, Uganda, South Africa, Zambia, and Nigeria, have been more proactive than others, but it is still hard for many to get PrEP.
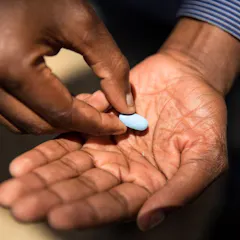
Judge Reed O'Connor ruled in a case that coverage for HIV prevention medicine PrEP violated the religious freedom of the plaintiffs. It is unclear whether the order will extend nationwide.

PrEP enables adolescent girls and young women to protect themselves from HIV without having to convince a partner to use a condom at the time of sex.

Adolescents and young people should get involved early in the design, planning and scale up of interventions.

This finding suggests public health efforts will have to address the treatment barriers these men face – like poverty or homophobia – to meet the nation’s goal of ending the HIV epidemic by 2030.
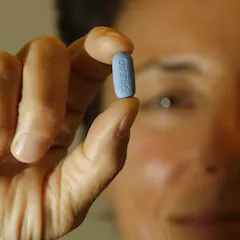
World AIDS Day on Dec. 1 this year comes at a time when a key step to removing financial barriers to PrEP access in the U.S. faces legal challenges.

Stigma and criminalisation of same-sex relationships makes it difficult for transgender women and men who have sex with men to seek preventive services. This compounds their risk for HIV infection.

It is urgent and overdue to implement PrEP in pregnancy and during breastfeeding. Failure to do so allows ongoing avoidable HIV infection among women in South Africa and their infants.

Current HIV criminal laws increase HIV stigma and discrimination against marginalized people – and negatively affect public health.

The Affordable Care Act has allowed many preventive health services, including cancer screenings and vaccines, to be free of charge. But legal challenges may lead to costly repercussions for patients.

Microaggressions are more subtle than outright discrimination. But they can directly affect HIV treatment outcomes.

Not achieving the targets for children and adolescents in sub-Saharan Africa means that new infections will continue to increase and HIV related mortality will be a reality for decades to come.
