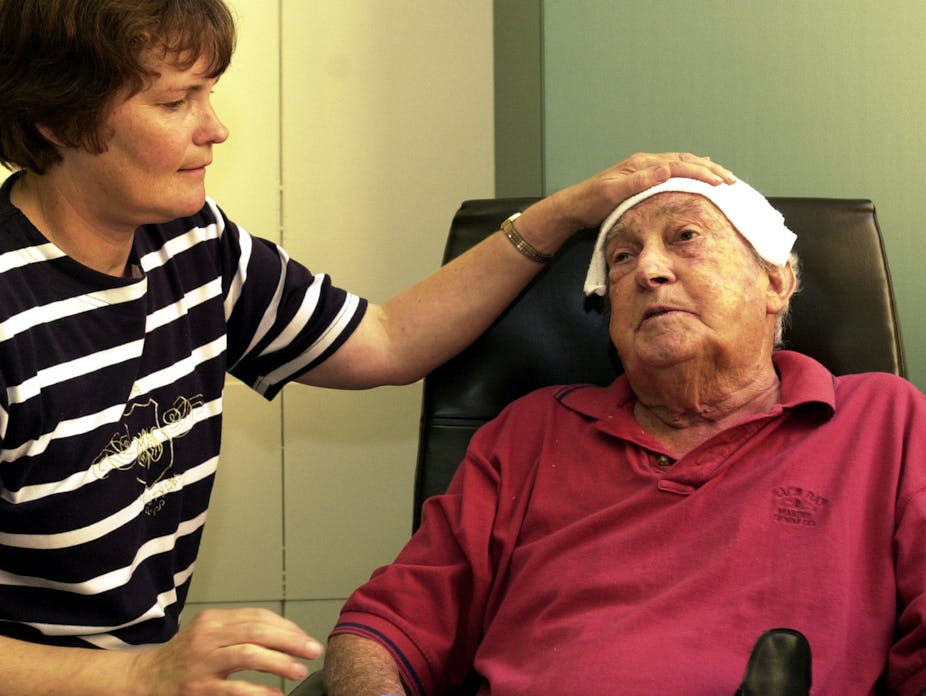
It’s no news that Australia is undergoing structural ageing – as is the rest of the developed world. Today 14% of Australia’s population is 65 and over. By 2061 this proportion is expected to rise to 22%.
Despite the doom, gloom and scaremongering that surrounds the mention of older adults and the aged care agenda, 90% of older people live at home and continue to do so into very old age. While nearly half of people aged 65 years and over have a disability or health condition that can restrict or limit their daily activities, the majority of older adults continue to live out their lives independent of residential aged care.
The reason they are able to do so is often the ongoing assistance of informal carers. Wives, husbands, daughters, sons, grandchildren and friends – all can be carers – provide help or supervision on an “informal” basis, as opposed to someone who is paid to provide care.
In 2012, carers made up 12% of our total population, equivalent to 2.7 million people: 770,000 of whom were identified as primary carers. Notably, the majority of carers are also older, often women, and over one-third are likely to have a disability too.
The costs of being a carer
For many, keeping their partner or parent living at home as they age is a priority. While they might find joy and satisfaction in providing care for someone who needs extra help and support, it can also be stressful and exhausting – especially if they’re getting older themselves.
The burden of caring for someone can come at a high personal cost. Research shows that it can lead to depression, anxiety and a decrease in wellbeing. One study found that over 50% of carers were depressed. Another found that once they become depressed, older adults are at higher risk of suicide than those who are younger. Even more compelling is the finding that 25% of people caring for a family member with dementia have contemplated suicide.
Many lifestyle changes – such as physical exercise and improved diet – can help combat depression but these changes can be difficult to implement when people are busy caring for someone else. Studies have indicated that physical exercise can help improve mood but it can be difficult to find the time to exercise when busy looking after an older person, particularly when people have an illness or increased frailty that stops them from exercising the way they used to.

One NHMRC-funded study underway in Australia is unique in that it targets both the carer and the person they are caring for. The study tests the effectiveness of an individually tailored in-home exercise program to reduce depression and improve the wellbeing of carers, as well as the people they care for.
It is hoped that exercise will improve the mood and physical function of the carer. It might also improve the physical abilities and mood of the person being cared for and, in so doing, take some of the stress and effort out of the care relationship.
As well as being stressful and increasing the likelihood of depression, caring for another person can have huge ramifications on an individual’s life. It can lead to a decrease in hours of employment (and consequent wages and superannuation) and can have an ongoing effect on future career prospects.
Budget adds to carers’ burden
In Australia, caring for people as they age is not just a pressure for individuals, but for society as a whole. Our health system and policy makers rely on informal carers to provide the assistance and supervision needed to keep people at home as they age.
While it’s difficult to place a dollar value on unpaid labour, it is estimated that in Australia the annual value of the assistance provided by informal carers is A$40 billion. This will only rise with the ageing population. It is therefore in everyone’s interest to support the wellbeing and health of those providing care.
The proposed federal budget changes to pensions and allowances will have a direct negative impact on carers. Tying increases to the CPI, which is lower than rises in average male weekly earnings, will effectively reduce the carer payment in real terms. As Carers Australia CEO Ara Cresswell has said:
The government is failing to recognise that caring is contributing.
The proposed changes to the Medicare system will have a profound effect on carers and their care recipients, particularly those who are ageing. They often have multiple conditions or disability. Co-payments of $7 for GP visits and other tests that don’t come under the hospital system will reduce incomes further, as will the increase in prescription costs.
The redirection of grants this year from the National Respite for Carers Program will compound these financial imposts. Reducing funding to such a vital support does little for carers’ wellbeing and health. Initiatives to improve support for carers, like that recently undertaken by the National Ageing Research Institute (NARI) and Carers Victoria, will become even more important.