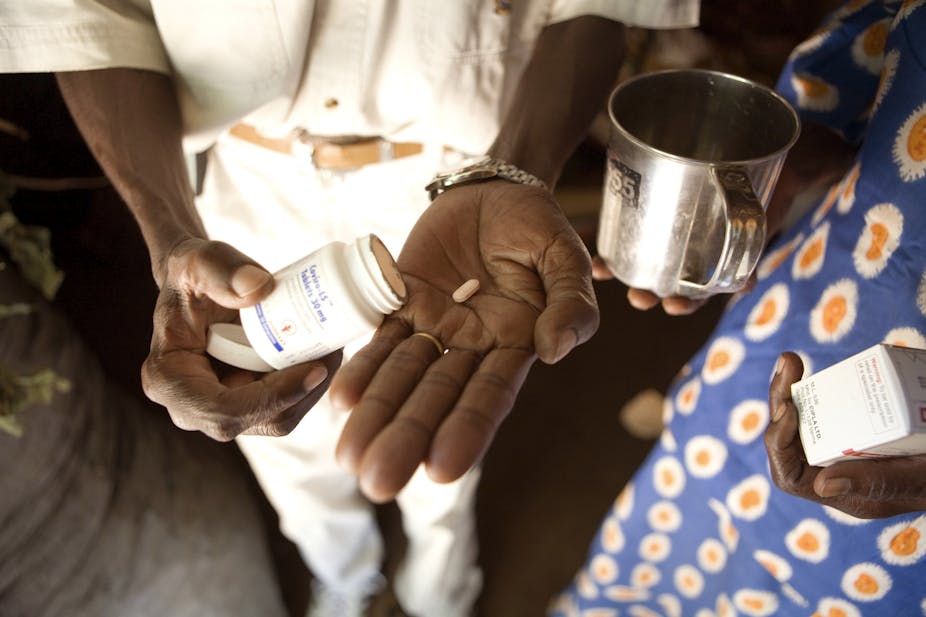
In the years after the “slim disease” or HIV was first recognised in southwestern Uganda in 1982, access to treatment was for a privileged few. At the time, only a handful of clinics such as the Joint Clinical Research Centre could offer any relief for those living with HIV. Because only a small number of patients could afford the prohibitive fees for HIV services, care was almost entirely provided by medical doctors.
Even when antiretroviral medicines such as AZT became available 14 years later in 1996, only a select few Ugandans such as top government officials and high-income individuals could afford them.
Many Ugandans with HIV died premature deaths as the virus ravaged their bodies with no medicines to stall it. Then the game-changer came in June 2004. The United States government, through the PEPFAR initiative, provided substantial external donor aid to enable the provision of free antiretroviral therapy (ART) at national and regional referral hospitals across Uganda.
But then the “medicines without doctors” predicament emerged as a new challenge. From the 2,700 who were enrolled on treatment in 2004, there are currently 1.2 million Ugandans accessing ART.
The giant leap in the number of people accessing HIV treatment would not have been possible without task shifting from medical doctors to less-specialised cadres such as nurses and midwives. Task shifting to nurses was, however, done informally without a guiding policy framework. There is still no such policy.
A national policy on task shifting is critical. Nurses need legal protection against litigation in the course of executing delegated tasks. This policy could also serve as a blueprint for overcoming Uganda’s health workforce shortages and help the country reach health-related sustainable development goals.
Task shifting to nurses
As the world commemorates 2020 as the International Year of the Nurse and Midwife, we reflect on findings from a study we conducted across Uganda that revealed the true extent of task shifting to nurses in HIV care. We found that in the nearly 200 hospitals we visited across Uganda’s 10 geographic sub-regions, 93% of them permitted nurses to initiate and manage ART.
Our study reveals for the first time that nurses have the highest representation in the leadership and governance of HIV clinics across Uganda. This trend was more pronounced in rural areas but was seen in both rural and urban settings.
The facility managers perceived nurses to be a more dependable cadre as they “tend to stick around for years”. There was a common perception that “higher grade” cadres, such as young doctors, tend to leave for further training and better-paying jobs. Because of the shortage of medical doctors, nurses were depended upon as the backbone of HIV service delivery in HIV clinics across Uganda.
Nurses were empowered to be “all-rounders” in HIV care, from testing to ensuring viral suppression. We were told that nurses could do “big things” if they receive regular training and supportive supervision. Over the past decade, several studies have demonstrated that nurse-managed HIV care and treatment is not inferior.
The dramatic expansion in access to HIV treatment in Uganda revealed the competence of nurses in managing more advanced roles in HIV disease management. But task shifting to nurses is still not yet formally recognised by policy. The official “scope of practice” of nurses has not been revised to reflect the extension in their roles in HIV service delivery.
Furthermore, pre-service training of nurses has not been revised to reflect their increased responsibilities in HIV disease management and hospital administration.
Although Uganda has lagged, other countries in Africa have not. In 2010, South Africa unveiled an official policy known as “Nurse Initiated and Managed Antiretroviral Therapy”, which permitted nurses into clinical HIV disease management.
Way forward
Task shifting to nurses should not only be about HIV but in response to the burgeoning noncommunicable diseases epidemic as well. This is why policy reforms must be geared towards recognising what nurses are capable of as a cadre to achieve broader public health goals, including advancing progress towards universal health coverage.
Newer and more efficient forms of HIV service delivery approaches known as “differentiated service delivery”, approved by the World Health Organisation in 2016, emphasise tailoring HIV care to patients’ individual needs instead of a “one size fits all” approach. For instance, whereas patients stable on ART can be managed by nurses, those with advanced HIV disease can be managed by clinicians.
Our study adds to an accumulating evidence base from across sub-Saharan Africa and the mounting calls for nurses to be sufficiently recognised for their prominent role in making HIV treatment more widely available over the past decade.