
Articles on Flu
Displaying 41 - 60 of 151 articles

Recent computer modeling shows the upcoming flu season might see a surge in cases. Coupled with COVID-19’s continued threat, doctors are again urging Americans to get their shots.

For decades, US schools have been common sites for vaccine clinics to respond to outbreaks and provide catch-up immunizations. So why are they suddenly controversial?

Comparisons with flu are unhelpful – these diseases need to be treated differently.
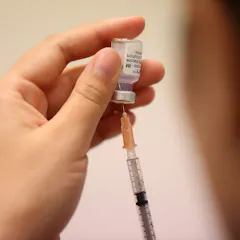
Age and education level are the main factors associated with vaccine hesitancy. While this affects Māori and Pacific communities, basic access to health care and information is more important.

Americans were tired of social distancing and mask-wearing. At the first hint the virus was receding, people pushed to get life back to normal. Unfortunately another surge of the disease followed.

You need a new shot every year because current flu vaccines provide limited and temporary protection. But researchers’ new strategy could mean a one-and-done influenza vaccine is on the way.

Going out in the cold won’t necessarily lead to you getting a cold. But cold weather in general is more hospitable to viruses, so it’s wise to take steps to keep your immune system strong.

Millions of Latinos may not get the influenza shot this year, which could be an indicator of whether they will get a COVID-19 shot. A rural clinic shows how building trust can help overcome reluctance.

Resistant bacteria aren’t the only risk posed by overprescribing antibiotics. A more immediate risk is side-effects and reactions, which a new review shows are surprisingly frequent and often severe.

Many people object to the added ingredients in vaccines. But pharmacists explain why those fears are unwarranted.

These drugs may help slow or reverse immune system decline.

A new study is the first to identify sex differences in inflammation and immune cell activation in response to SARS-CoV-2 infection, which causes COVID-19.

The pandemic has exposed many of us to new statistical concepts, on the news, in everyday conversations and on social media. But how many are you getting wrong?

A team of experts argues that after taking care of essential workers, COVID-19 vaccinations should be given to the greatest transmitters of the virus, who are mostly the young.

Those opposing vaccinations often mistrust government, science and the news media. There may be better ways to persuade them than by offering facts only.

Although it can sometimes be challenging, there are ways to distinguish respiratory symptoms caused by a virus and those caused by an allergy.

The COVID-19 death toll in the US is now over 130,000. What do 130,000 fatalities look like? A biostatistician provides some perspective.

It’s excellent this virus has been found early, but there is no evidence yet of human-to-human transmission.

A century ago, the influenza pandemic killed about 50 million people. Today we are battling the coronavirus pandemic. Are we any better off? Two social scientists share five reasons we have to be optimistic.

CC BY-NC-ND5.32 MB (download)
Thinking about getting the flu shot? This may help you decide.
