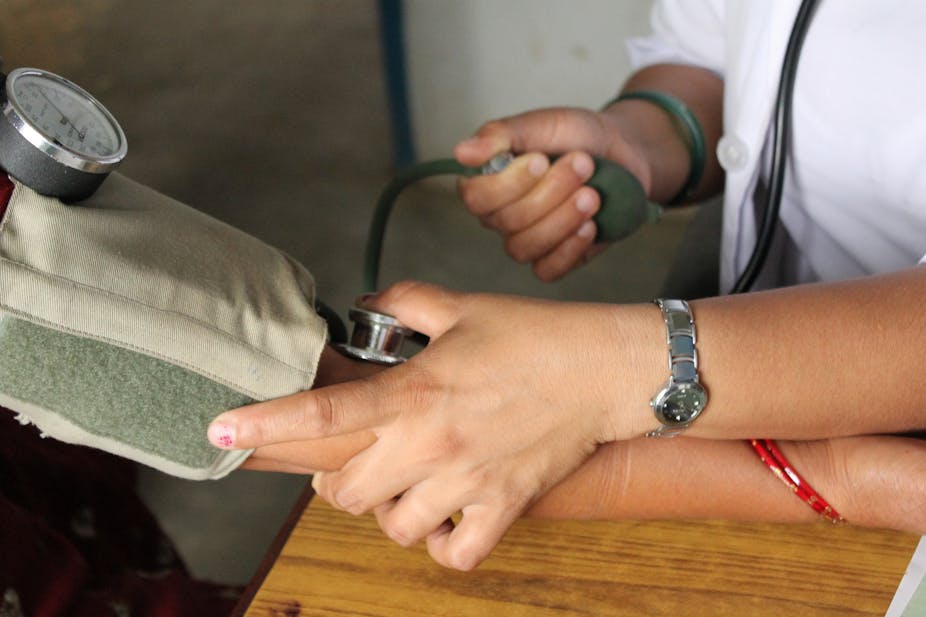
Britain’s National Health Service has spent much of its lifetime trying to get GP services right. The answer lies in a simple combination of scale and specialisation that could bring efficiency as well as improved care. As the NHS hunts even more savings during a spending squeeze, the need has rarely been greater.
The local doctor’s surgery is most people’s point of first contact with the NHS and is all important in the modern world of health care. It is where demand and need management meet and where flaws in the system can be solved at source. Expanding what is available by building networks of surgeries would make that easier. Once someone enters the more complex health systems up the chain, costs rise rapidly if they are misdiagnosed or sent for inappropriate treatments.
Building scale
There are some easy wins to be had. Building a better and beefed up GP system would help to address the anxieties that many people have around contacting medical services. And anxiety delivers dysfunctional results. Some go too often, but never get enough time to explain themselves and end up feeling more anxious and guilty each time they return. Others might put off going and ignore dangerous symptoms. Late diagnosis is one of the biggest causes of escalating costs; earlier diagnoses could save the NHS billions.

And those who do go when they should don’t always get the right help, and keep going back around the system. This reduces its capacity to do other things. Not everyone contacting their GP needs expensive medical help. But a GP visit should be an opportunity to provide them with what they need and to prevent other major health problems escalating later in their lives.
So how do we address this? First, build clusters by creating networks of smaller surgeries. This would make good creative use of generalists who can also develop their own part time specialities. With good management and leadership, GP surgeries could pool resources and each provide a different but complementary specialist diagnosis and treatment element to the cluster. There would also be a flow of specialists and treatment visits from area hospitals, and investment in higher quality diagnostic equipment in each cluster.
So, instead of having one local surgery, you might have access to three or four which were set up to tackle more effectively a wider range of medical complaints. Add in the excellent community relations with patient and charity groups that an efficient cluster of surgeries would pursue and the offering looks even stronger. It would also help smooth out inequalities around the country in terms of patient to staff ratios. There would be issues with this model in more dispersed parts of the countryside, of course, but this looks entirely workable in urban areas.
Regular visitors
Such a system would help tackle some key issues for the NHS. A broader offering which pulled in community health services, charities and counselling services would help particularly to address the high proportion of visits to the GP which are for psychological problems, or for long term chronic conditions. Standards can only go up if these organisations are sharing how they do things in a cluster and learning from each other.

These clusters of GP services could also form part of ambitions for a 24-hour NHS, plans which have seen strike action threatened by junior doctors recently. The National Audit Office has described the difficulty young people and the employed sometimes face when trying to make local doctor appointments. This can be all the excuse people need to put off necessary visits, which leads to more costly treatments down the line. Simply put, weekend GP services are almost as important as round-the-clock hospital care.
And the costs won’t be as onerous as you think. Prevention – early diagnoses and changing behaviour to make people healthier – is what primary and community health care is best at and this saves secondary hospital costs in later years. Total primary health costs are currently a relatively small proportion of health care costs compared to hospital care.
Economies for the economy
And if we want another way to improve primary health care, perhaps we could look to a new form of partnership between employers and the NHS. Employers lose billions of pounds when their staff go off sick and this is made worse if employees have problems accessing primary care. Getting the right early help can be a big part of enabling reductions in sick leave. There may be something in it for employers to provide more primary health care support and advice? For example, providing flu immunisations to a large firm will most likely reduce winter absences. If the government provided incentives, it might even save the NHS money in the longer run.
The NHS is such a complex beast that it can only work with integrated and efficient services, helped along by a spark of quality leadership that aims to get the whole machine working to support common values. At the moment we’re not making the most of the part of the system most likely to set the tone for the entire enterprise. A successful NHS will be about collaboration above competition and should be creating local primary services that are large enough, broad enough and funded enough to make GPs not just gatekeepers to a strained hospital system, but powerful providers of first resort.