
Articles on Palliative care
Displaying 21 - 40 of 86 articles

Death-friendly communities that welcome mortality might help us live better lives and provide better care for people at the end of their lives.

Many Australians come to the end of their life while living in aged care. But damningly, the aged care royal commission found many residents have worse palliative care options than those living elsewhere.

Expanding access to medical assistance in dying (MAID) to those not terminally ill puts vulnerable people at risk of feeling pressured into MAID, and doctors at risk of being forced to facilitate it.

Preventing people from dying alone in a pandemic takes ingenuity and money, but it’s the right thing to do.
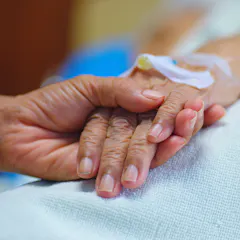
Lack of training and skills among those who work in the area may lead to LGBT people receiving poorer palliative care.

It’s time to talk to your loved ones about what care and treatment you’d want if you face death from COVID-19.

Ghana’s lack of a palliative care policy is posing a significant challenge to effective healthcare for cancer patients.

How we experience the moment of death may be influenced by a cocktail of brain chemicals and the manner in which our brains shut down.

The seriously ill and their families often want to protect each other from thoughts of death. Conversation about end-of-life choices are, however, essential to a good death.

Nurses who surround the process of medically assisted dying are an important source of insight into the real conversations our society needs to have about what it’s really like.

Western Australia might soon become the second state in Australia to legalise voluntary assisted dying. Its proposed law draws on the Victorian model, but has some important differences, too.

As we sit on the cusp of voluntary assisted dying becoming legal in Victoria, we expect it won’t always be simple for people who want it to access it – at least in the legislation’s early days.

It is not always easy to identify who needs palliative care.

Palliative radiation therapy can improve a cancer patient’s life, by alleviating pain and other symptoms. Unfortunately, some doctors associate the term with end-of-life care and fail to refer people.

One of the great success stories in healthcare, a quarter of the UK hospice sector is said to be close to collapse.

You’ve more than likely heard of birth doulas. But nowadays, death doulas are providing support at the end of life. How they fit into existing structures of care remains to be understood.

In the final days of life, it may be too late to choose how you want to die, who you want to be cared by, and how you’d like your symptoms managed.

New findings show what the public really thinks about how we prioritise treatments at the end of people’s lives.

The UK has one of the most developed palliative care services in the world, yet people still miss out.

Most elderly Canadians do not receive the end-of-life care they desire. A new study hopes to rectify this.
