Methotrexate, sold under the brand name Methoblastin, is an antifolate drug, which means it inhibits the activation of folic acid in the body.
It is taken once per week to treat a range of conditions. These include rheumatoid arthritis, the skin disorder psoriasis and inflammatory bowel disease. This weekly therapy is known as “low-dose methotrexate”.
Methotrexate was first developed in the 1950s as a cancer treatment and is still used for this in higher doses.

How it works
The methotrexate drug molecule is structurally similar to folic acid, which is important for making new cells. It inhibits the enzyme (dihydrofolate reductase) that turns folic acid into its active form. This reduces cell growth and is why methotrexate is used to treat some cancers.
The way methotrexate works for inflammatory conditions is less clear. But we know it has a range of effects on DNA synthesis and immune signalling, which are thought to reduce the inflammation.
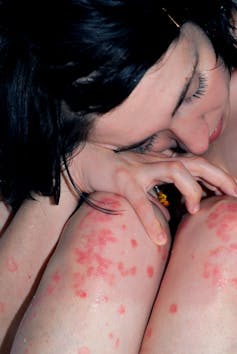
In rheumatoid arthritis, methotrexate reduces inflammation and damage to joints. Rather than just masking pain, methotrexate reduces it by reducing severity of the disease. For this reason, it’s known as a disease-modifying anti-rheumatic drug (DMARD).
History
Methotrexate was developed in the 1950s when researchers discovered that increased folic acid worsened leukaemia and that dietary deficiency of folic acid reduced the cancer cell count.
This inspired scientists to develop drugs structurally similar to folic acid that bound to its receptors in the body and inhibited its effects.
Methotrexate was synthesised in the 1950s and was shown to be effective for leukaemia and several types of solid tumours. Prior to this discovery, cancer treatments had been limited to surgery and radiotherapy.
What it’s used for
Methotrexate is still used intravenously in high doses to treat cancer. But its most common use now is in rheumatoid arthritis and other inflammatory conditions. Low-dose methotrexate (taken once a week) was shown to be effective in rheumatoid arthritis in 1985. It is now a drug of first choice for rheumatoid arthritis.
Methotrexate is also used as an intra-muscular injection to terminate ectopic pregnancy, as an alternative to surgery.
Use and cost
There were 260,000 scripts for methotrexate tablets dispensed on the Pharmaceutical Benefits Scheme (PBS) in 2015.
Methotrexate costs between A$0.73 and $1.87 per tablet on the PBS. Since it is taken only once per week, it is a very low-cost treatment.
How it makes you feel
The correct dose of methotrexate (commonly between 7.5mg to 25mg per week) will reduce inflammation and alleviate the condition it’s prescribed for, whether that’s rheumatoid arthritis, psoriasis, inflammatory bowel disease, and so on. But it can take one to two months to work.
The most common side effects include nausea and mouth ulcers, due to the drug’s inhibition of folate. This is because inhibiting folate targets rapidly dividing cells of the gastrointestinal tract.
Folic acid supplementation is used to prevent side effects associated with low-dose methotrexate therapy. Preferably, folic acid is not taken on the same day methotrexate is taken. Many studies have shown that folic acid supplements do not hinder the effectiveness of methotrexate.
If methotrexate is taken too frequently – daily instead of weekly, for instance – it can suppress bone marrow, reducing blood cell production and impairing the immune system. This can make the body susceptible to infections and, in the worst-case scenario, result in death.
In rare cases, this suppression of blood cell production can also occur at normal doses. This risk is higher in the elderly and in patients with reduced kidney function or dehydration.
Other severe (but rare) side effects include lung and liver damage with long-term usage. People prescribed methotrexate will be closely monitored by their doctor for these effects.
In addition to being an effective treatment for rheumatoid arthritis, methotrexate reduces the risk of death from heart disease. This may be because it reduces inflammation, a risk factor for heart disease, and because it affects the cellular mechanisms that lead to the deposition of fat in arterial walls.
Interactions
Low-dose methotrexate interacts with drugs that inhibit the way the body uses folic acid, such as the antibiotics trimethoprim with sulfamethoxazole (Bactrim, Resprim) and trimethoprim alone (Triprim, Alprim). Medicines that impair kidney function can increase levels of methotrexate in the body. Taking these medicines in combination with methotrexate increases the risk of bone marrow suppression.
The dangers of daily dosing
A study published in the Medical Journal of Australia detailed more than a decade’s worth of Australian data on methotrexate, looking at cases where people had accidentally taken methotrexate daily instead of weekly.
Taking methotrexate for as little as three days in a row is enough to cause serious consequences, including sepsis (infection of the blood) and death. Note that this is different to high-dose methotrexate in chemotherapy, where “rescue therapy” is used to prevent toxicity.
Since 2000, at least eight Australians have died and many more have been hospitalised after taking too much methotrexate. Methotrexate use is increasing, which has corresponded with an increase in accidental daily dosing reported to Australian Poisons Information Centres.
Given that most medicines are taken daily, these potentially fatal mistakes can be easy to make. Methotrexate is effective and safe if used correctly. Changes in packaging and labelling, and alerts in prescribing and dispensing software used by doctors and pharmacists, could help prevent overdosing.
If you have questions about your methotrexate treatment, speak with your doctor or pharmacist. For advice about dosing errors with methotrexate or any other medicine, contact the Poisons Information Centre, 13 11 26 (24 hours a day, 7 days a week), Australia-wide.

