There is increasing media interest about surgical procedures on new babies for tongue tie. Some hail it as a miracle cure, others view it as barbaric treatment, though adverse outcomes are rare.
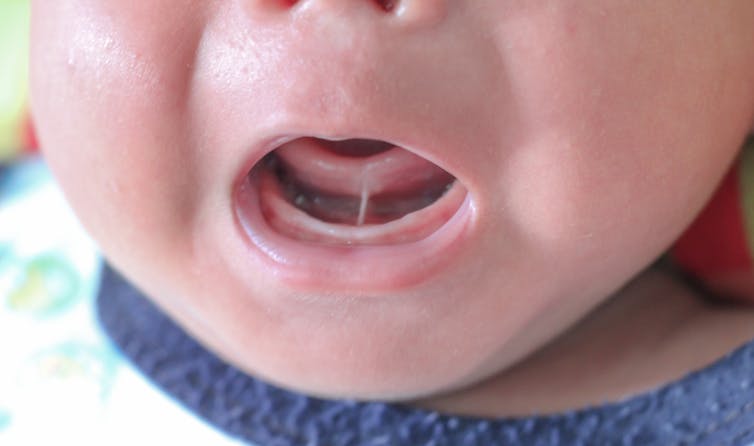
Tongue tie occurs when the tissue under the tongue is attached to the lower gum or floor of the mouth in a way that can restrict the movement or range of the tongue. This can impact early breastfeeding in babies. It affects an estimated 8% of children under one year of age.
While there has been an increase in tongue tie releases (also called division or frenotomy), it’s important to keep this in perspective relative to the increase in breastfeeding rates.
The World Health Organization recommends exclusive breastfeeding for the first six months of life, with breastfeeding recommended into the second year of life and beyond for the health of mother and baby as well as optimal growth. Global rates of breastfeeding infants for the first six months have increased from 38% to 48% over the past decade. So, it is not surprising there is also an increase in the number of babies being referred globally with breastfeeding challenges and potential tongue tie.
An Australian study published in 2023 showed that despite a 25% increase in referrals for tongue tie division between 2014 and 2018, there was no increase in the number of tongue tie divisions performed. Tongue tie surgery rates increased in Australia in the decade from 2006 to 2016 (from 1.22 per 1,000 population to 6.35) for 0 to 4 year olds. There is no data on surgery rates in Australia over the last eight years.
Tongue tie division isn’t always appropriate but it can make a big difference to the babies who need it. More referrals doesn’t necessarily mean more procedures are performed.
How tongue tie can affect babies
When tongue tie (ankyloglossia) restricts the movement of the tongue, it can make it more difficult for a baby to latch onto the mother’s breast and painlessly breastfeed.
Earlier this month, the International Consortium of oral Ankylofrenula Professionals released a tongue tie position statement and practice guideline. Written by a range of health professionals, the guidelines define tongue tie as a functional diagnosis that can impact breastfeeding, eating, drinking and speech. The guidelines provide health professionals and families with information on the assessment and management of tongue tie.
Tongue tie release has been shown to improve latch during breastfeeding, reduce nipple pain and improve breast and bottle feeding. Early assessment and treatment are important to help mothers breastfeed for longer and address any potential functional problems.
Where to get advice
If feeding isn’t going well, it may cause pain for the mother or there may be signs the baby isn’t attaching properly to the breast or not getting enough milk. Parents can seek skilled help and assessment from a certified lactation consultant or International Board-Certified Lactation Consultant who can be found via online registry.
Alternatively, a health professional with training and skills in tongue tie assessment and division can assist families. This may include a doctor, midwife, speech pathologist or dentist with extended skills, training and experience in treating babies with tongue tie.
When access to advice or treatment is delayed, it can lead to unnecessary supplementation with bottle feeds, early weaning from breastfeeding and increased parental anxiety.
Getting a tongue tie assessment
During assessment, a qualified health professional will collect a thorough case history, including pregnancy and birth details, do a structural and functional assessment, and conduct a comprehensive breastfeeding or feeding assessment.
They will view and thoroughly examine the mouth, including the tongue’s movement and lift. The appearance of where the tissue attaches to the underside of the tongue, the ability of the tongue to move and how the baby can suck also needs to be properly assessed.
Treatment decisions should focus on the concerns of the mother and baby and the impact of current feeding issues. Tongue tie division as a baby is not recommended for the sole purpose of avoiding speech problems in later life if there are no feeding concerns for the baby.

Treatment options
The Australian Dental Association’s 2020 guidelines provide a management pathway for babies diagnosed with tongue tie.
Once feeding issues are identified and if a tongue tie is diagnosed, non-surgical management to optimise positioning, latch and education for parents should be the first-line approach.
If feeding issues persist during follow-up assessment after non-surgical management, a tongue tie division may be considered. Tongue tie release may be one option to address functional challenges associated with breastfeeding problems in babies.
There are risks associated with any procedure, including tongue tie release, such as bleeding. These risks should be discussed with the treating practitioner before conducting any laser, scissor or scalpel tongue tie procedure.
Post-release support by a certified lactation consultant or feeding specialist is necessary after a tongue tie division. A post-release treatment plan should be developed by a team of health professionals including advice and support for breastfeeding to address both the mother and baby’s individual needs.
We would like to acknowledge the contribution of Raymond J. Tseng, DDS, PhD, (Paediatric Dentist) to the writing of this article.

