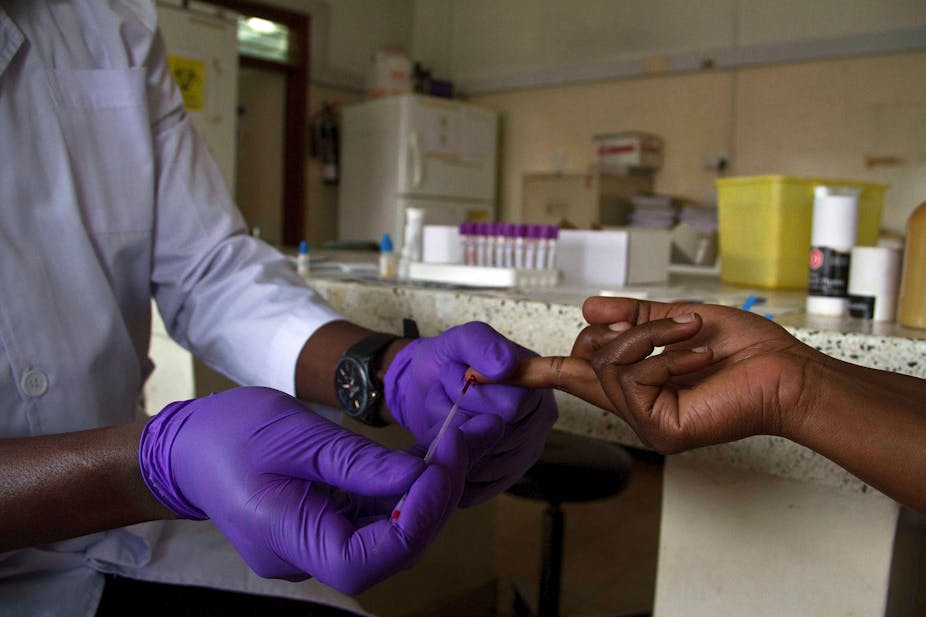
Some have dubbed it the collision of two pandemics. When the COVID pandemic hit two years ago, it was said that HIV was “de-prioritised” – in other words, forced to take a back seat.
The truth is that even before the advent of COVID, donors had begun to exit HIV programmes with increasing frequency.
I have been tracking decisions donors have been making around HIV programmes in Uganda, and conducting research on their impact for over seven years. The reason for this is that there has been limited research on understanding the impact of loss of donor support on HIV services in resource-limited settings.
The level of dependency on donor funding is very high in both low- and middle-income countries. For example, Pepfar the US government’s HIV and AIDS response programme, can account for as much as 70% of national HIV spending as is the case in Uganda.
In addition, Pepfar often hires additional personnel to help manage HIV medication supply chains in districts, frequently trains health workers in quality HIV care including on-site support supervision and invests in strengthening laboratory systems.
In Uganda, Pepfar is a major funder of HIV services. In a recent paper we looked at what happens to HIV services when countries heavily dependent on Pepfar lose some of this support.
Our findings indicate that basic services such as HIV testing and treatment were still available. But there were substantial reductions in the scope and quality of services provided. For example specialised peadiatric HIV services and nutrition support for people on antiretroviral therapy stopped. And patients felt that waiting times were longer and stock-outs more frequent.
HIV services must be comprehensive to ensure that people take their medication as prescribed and avoid onward transmission of the virus. Services such as child HIV care and ensuring medicine collection is seamless are a key part of ending HIV as a public health threat.
What’s changed in the donor landscape
Some of the biggest donors in health include Pepfar and the Global Fund to Fight AIDS, Tuberculosis and Malaria, an international funding mechanism.
Over the past decade it’s become clear that global health organisations were scaling down on HIV funding, or changing how their money is dispersed.
The Global Fund has been systematically weaning off countries attaining middle-income status from its HIV support programmes in the belief that they have improved per capita income and that, ideally, this translates into more investments in their national HIV responses.
Pepfar cut support to countries described as “middle income” such as Vietnam, Nigeria and South Africa. In August 2012, it announced it would halve its $500 million annual budget for South Africa.
Pepfar changed how it distributes HIV finances nationally in 15 focus countries. In Uganda, between 2015 and 2017, it implemented a policy known as “geographic prioritisation”. The aim was to use its aid more effectively. Instead of a generalised national response, it sought to align aid with HIV burden at sub-national level. The idea was that districts in Uganda that had a higher HIV burden would receive more support while those with lower HIV burden would receive significantly less support.
Some are predicting that the COVID-19 pandemic will further dent global HIV funding.
The Uganda experience
Our mixed-method study explored the impact of Pepfar’s change in policy on HIV services in the country. Our research showed that policy shifts meant less dollars for HIV services in some parts of Uganda.
The change in policy resulted in 734 “low volume” health facilities losing site-level support while 10 districts in Northern Uganda with a relatively low HIV burden were meant to transition to Uganda government support.
In our qualitative arm of the study, we found that the change in the way Pepfar provided aid to Uganda had important effects.
The scope of HIV services narrowed: The health workers and patients we talked to indicated that paediatric HIV services ceased, free HIV testing ceased at supported for-profit clinics. Patients decried the loss of nutrition support in food-insecure parts of Uganda.
Quality of HIV care declined: Patients were unequivocal in relaying the notion that the quality of HIV care had progressively declined since Pepfar changed its policy. They talked of health workers being preoccupied with “medicines dispensing” rather than patient-centred care. The frequency of stock-outs of medicines increased with loss of supply chain experts.
Patients also indicated that waiting times were longer and HIV clinics were less organised. This was because Pepfar paid regular monetary allowances to “expert patients” to help plug severe staffing gaps at HIV clinics such as to help in managing triage systems.
Community outreach activities: An important finding of our study was that community HIV outreach activities were heavily affected. Health workers and “expert patients” no longer received monetary allowances for making trips into communities for follow up of clients in their homes and for demand creation for HIV services, hence engagement in HIV care suffered. Pepfar’s changes meant that this was’t happening anymore.
Many of the effects described by health workers and patients were “negative”. But we also found that, in some cases, the loss of Pepfar support led to more integration of HIV with other services. For example, integrated community outreaches had combined immunisation and HIV testing. This prevents duplication and wastage inherent in disease-specific outreaches.
In addition, we found that a few districts in Uganda stepped up and increased funding for HIV such as providing fuel to transport samples to HIV labs.
But funding gaps remain. What’s clear is that further alternatives are needed.
Overall, the Uganda government hasn’t responded adequately, even though it knew that the cuts in funding were looming.
It is clear that increasing local ownership of HIV programmes is of paramount importance. In 2014, Uganda announced an “AIDS Trust Fund” to supplement donor aid to be financed through levies on soft drinks. This ought to be revived and fast tracked.