A particular focus will be Australia’s high use of antibiotics in general practice, which is 20% above the OECD average. – Minister for Health and Aged Care Sussan Ley, media release announcing implementation of the National Antimicrobial Resistance Strategy 2015-2019, November 10, 2016.
As she launched the implementation plan for Australia’s National Antimicrobial Resistance Strategy, Health Minister Sussan Ley said Australia’s use of antibiotics in general practice is 20% above the OECD average.
Is that right?
Checking the source
When asked for a source to support her statement, a spokesperson for Sussan Ley said:
This statement is based on information contained in the National Antimicrobial Resistance Strategy, page 11. This data comes from the OECD Health Statistics 2013.
Does Australia have ‘high use of antibiotics in general practice’, at 20% above the OECD average?
Yes, it is high; no, it is not 20% above the OECD average.
The data Ley quoted is out of date, and it includes antibiotic use in all human health sectors – not just general practice (that said, the lion’s share of antibiotic scripts written in Australia are written by GPs).
But her broader message is correct: it is true that Australia’s antibiotic use is high and it is well above the OECD average. This is dangerous because overuse of antibiotics can lead to antimicrobial resistance, which is where antibiotics that once worked effectively no longer do.
The minister sourced the figure of 20% to the 2013 OECD Health at a Glance report. Using data from 2010 or the nearest year, that report found Australia’s antibiotic use to be 17.5% above the OECD average. Ley rounded that up to 20%, which is fair enough.
But that figure is out of date. The most recent OECD Health at a Glance report, published in 2015, shows Australia’s antibiotic use has fallen slightly since 2013. It’s now 10% higher than the OECD average. (An improvement, but still dangerously high.)
And the figures in both the 2013 and 2015 OECD reports include antibiotics prescribed by all health practitioners – including dentists and optometrists, for example – not just GPs.
‘Defined daily doses’: findings from 2015 vs 2013
There is an internationally agreed measure for comparing the use of medicines: “defined daily doses per 1,000 people per day”. Defined daily doses are set and published by the World Health Organisation. The OECD used this method in its reports.
The 2015 OECD report found that, using data from 2013 or the nearest year, 22.8 defined daily doses of antibiotics were prescribed per 1,000 people in Australia every day. The OECD average is 20.7 defined daily doses per 1,000 people every day. That makes Australia’s prescription rate 10% higher than the OECD average. (Remember, this includes antibiotics prescribed by all health practitioners, not just GPs.)
The chart below is from the 2015 OECD report.
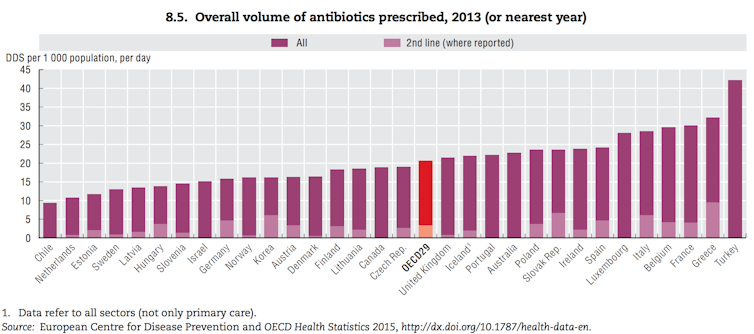
In the OECD chart above you will see the term “2nd line” in fine print (at the top). This refers to classes of antibiotics that medical experts say should be used conservatively to reduce the chance of germs developing resistance to them. These classes of antibiotics are called “quinolones” and “cephalosporins”. But Australia did not report the data for first and second line antibiotics separately, which is why Australia’s column in the first chart is all one colour.
The chart below shows Australia vs other OECD countries from the 2013 OECD report.
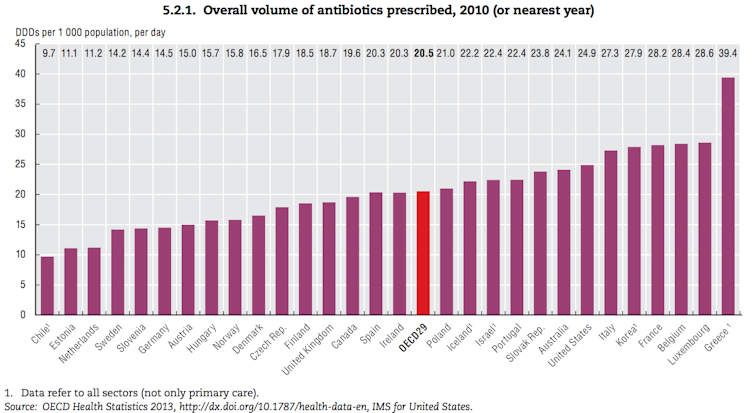
Experts often consider the benchmark countries to be those in Scandinavia and the Netherlands. Australian health practitioners prescribe antibiotics at a rate 25% higher than those in Finland, and 111% higher than the Netherlands.
Limitations of the OECD data
There are a number of drawbacks to using the “defined daily doses” measure for comparing antibiotic use.
The defined daily dose applies only to adults, yet there are quite high rates of antibiotics scripts written for children.
The measure also fails to account for variation in standard doses in different countries. This can result in a different value for the statistic, even when the same proportion of the population took the same number of courses of antibiotics in a year.
Australia now has a national surveillance system for antimicrobial use and resistance, and its first report was released in June. The report contains a more detailed look at antibiotic use in the Australian community, using 2014 data from the Pharmaceutical Benefits Scheme.
Apart from counting the “defined daily doses” there’s another way to assess antibiotic use: by counting prescription numbers per head of population.
In 2014, there were more than 30 million scripts dispensed for systemic and topical antibiotics in Australia. It was found that at least 45% of Australians took at least one course of antibiotics during that year.
Unfortunately, only a few countries report their primary care antibiotic prescription numbers per head of population. These are shown in the chart below, taken from the report.
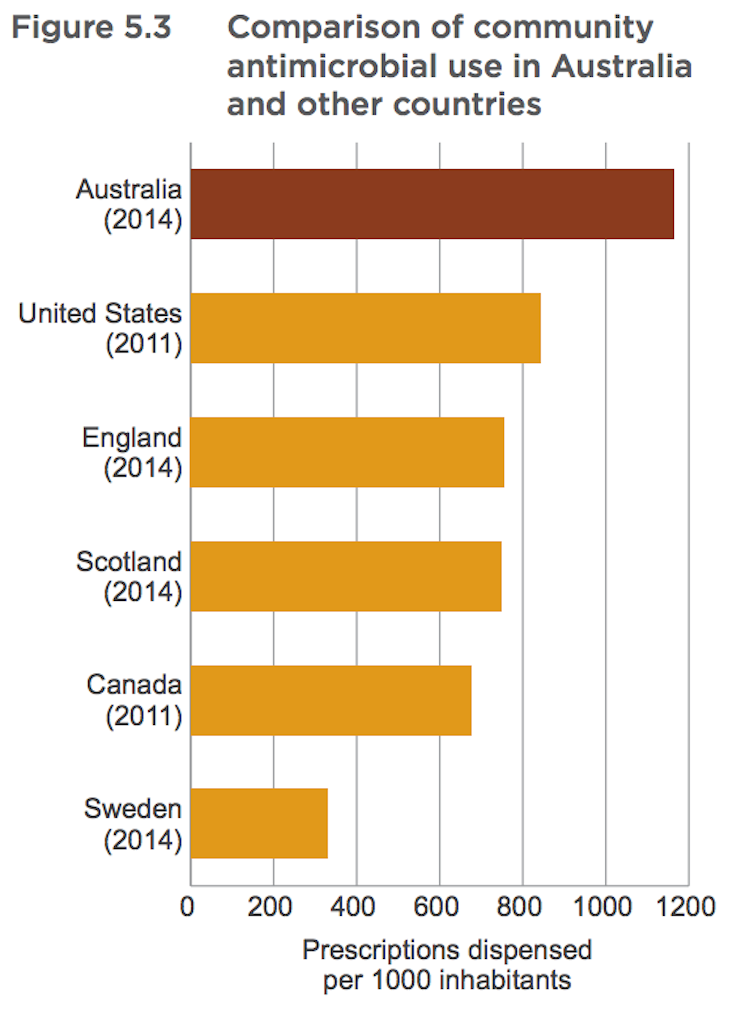
Overall, the point of the minister’s quote is clear: Australia’s antibiotic use in the community is unnecessarily high.
Evidence from Australia’s NPS MedicineWise, presented in the AURA report, makes it clear that antibiotics are often prescribed for infections when they’re not needed, particularly with respiratory viral infections like cold and flu.
Verdict
The data Sussan Ley quoted is a bit out of date – to be accurate, the statement should have said 10% above the OECD average, not 20% – and it refers to antibiotic use in all sectors, not just prescriptions by GPs.
But her broader message about Australia’s antibiotic use still being high compared to the OECD average is correct – and it’s an important point to make. Overuse of antibiotics is dangerous, as it can lead to situations where antibiotics that once worked effectively no longer do. – John Turnidge
Review
This analysis of Sussan Ley’s comments is accurate. I would further note that:
1) Government initiatives are helping to reduce antibiotic usage in other countries. For example, England just announced its first decrease in usage.
2) While this FactCheck focuses on antibiotic usage in humans, usage in animals is much less clear, often poorly documented, and also contributes to the increase in antimicrobial resistance. In the United States, 70% of antibiotics are consumed by animals.
Australia appears to have significantly lower antibiotic use in animals than other countries, as indicated in Australia’s first national antimicrobial resistance strategy. – Mark Blaskovich.

