Uganda is currently in a partial country-wide lockdown. The “second wave” of coronavirus infections has been especially unforgiving. There is no household in Uganda I know of that has not been touched by the COVID-19 pandemic. Social media posts are awash with reports of death. Hundreds of lives cut short in their prime. It is no longer a story about the elderly. The frequency of death announcements in the national newspapers is truly unprecedented.
Earlier this year, the world watched as funeral pyres burned across India. At the time, the ravages of the virus appeared a little distant. But with daily flights from New Delhi, Uganda was to have its own cases of the dreaded Delta variant, which was soon confirmed by the Uganda Virus Research Institute. Observers have also blamed Uganda’s recent presidential and parliamentary elections for the rise in infections, which had been initially admirably controlled.
Read more: What Uganda has got wrong – and right – in its struggle to contain COVID-19
Uganda announced its first total lockdown on 20 March 2020. Public and private transport was banned. Individual movement was restricted. People needed a special pass to travel about. The second 42-day lockdown was announced in mid-June 2021. This has now been eased. It appears that lockdowns will continue to be a reality of life in Uganda, which has vaccinated less than 1% of its population.
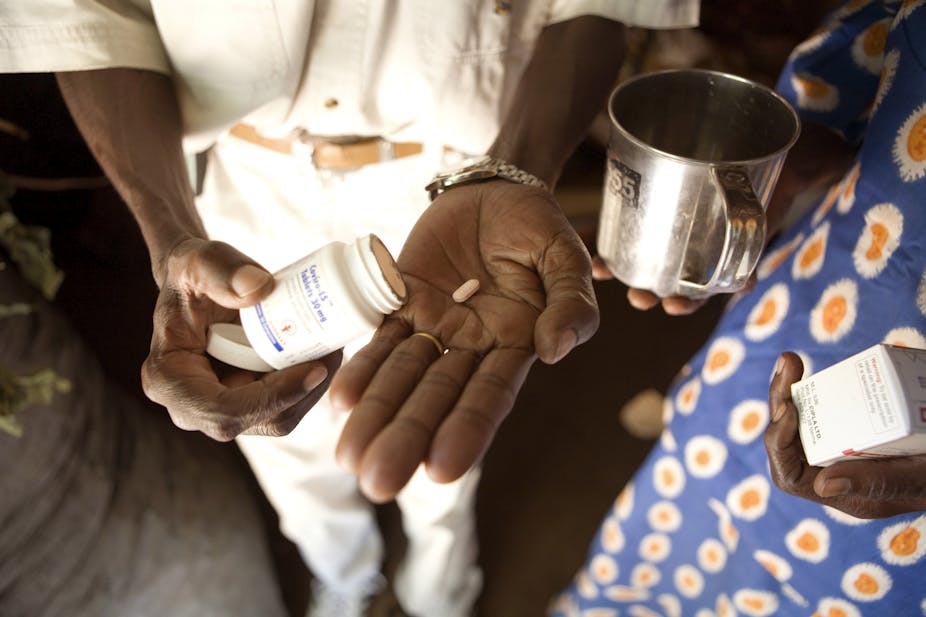
Much like March last year, people living with HIV are stuck in their homes and unable to visit their preferred health facilities to get their medication refills. Due to widespread HIV-related stigma, patients frequently seek HIV care at facilities several kilometres away from where they live. There are currently 1.2 million Ugandans enrolled on antiretroviral therapy (ART) – they are especially affected by the lockdown.
Studies suggest that people need to adhere strictly to antiretroviral therapy to suppress the virus. Interruptions in access to HIV medication can lead to treatment failure or drug resistance.
My colleagues and I conducted a study soon after the first lockdown in Uganda last year in eight districts from Eastern and Western Uganda. We found that HIV care providers used alternative ways to reach patients stuck in their homes by delivering HIV medications to their doorsteps. The identified innovations include decentralisation of ART distribution to community platforms, and six-monthly refills. These will be applicable beyond COVID-19.
Five strategies for distributing ARVs
Our study shows that districts and providers devised five key strategies to overcome lockdown restrictions in distributing antiretrovirals.
Home-based deliveries
Health facilities, supported by district health officers and organisations that implement PEPFAR (US President’s Emergency Plan for AIDS Relief) programmes, committed vehicle fleets to deliver medication refills door-to-door. These “mobile brigades” were frequently staffed by “expert patients” or HIV patients who serve as informal staff at the facilities they attend. They had the onerous task of locating homesteads deep in rural communities in Uganda.
Extending ART refill periods
Prior to the lockdown, the Uganda Ministry of Health was recommending that stable patients could be given three months’ supply of their medication at a time. During last year’s lockdown, dispensing was extended from three to six months for facilities with sufficient stock. The Ministry of Health also directed facilities to extend refills to “visitors” and not only to their registered patients.
Community-based ART distribution
Starting in 2017, Uganda permitted outreach sites where people with HIV could collect their medication. These are known as community drug distribution points. The collection points are designated venues such as the community hall or even the private pharmacy nearest your home where patients pick up their HIV medication. The AIDS Support Organisation, an HIV care provider group in Uganda, reported that it routed most of its refills through community distribution points.
Geospatial technologies
Locating patients’ homes in the predominantly rural settings of Uganda can be daunting. There is limited coverage of modern physical addresses, and many settlements are informal. These obstacles stood in the way of “mobile brigades” distributing ART refills in remote outposts. Tertiary hospitals reported relying on geospatial technologies to pinpoint geographic locations that could be linked with their roving “mobile brigades”. Facilities used the available information about their patients such as phone numbers or physical addresses to locate geographical points where patients reside. Due to fears of involuntary disclosure of HIV status, some patients in Uganda provide false phone numbers to care providers. This complicated ART refill distribution. The use of geospatial technologies helped overcome this barrier.
COVID-19 funding
District health officers reported that they took advantage of the funding they received from the Uganda government as part of the COVID-19 response to distribute ART refills during their community outreaches. It was reported that the vehicle fleet and fuel used during COVID-19 outreaches deep in rural communities also offered them an opportunity to distribute ART refills for patients living along those routes.
Beyond COVID-19
One of the positives of the lockdown was the unprecedented demand for community based ART delivery.
Before the pandemic, community-based ART models had registered relatively low uptake, mostly due to HIV-related stigma. These innovations in community ART distribution will continue to be important even beyond the COVID-19 pandemic, which may linger on in sub-Saharan Africa longer than in other parts of the world, due to delays in rolling out vaccines.