When my friend had her gall bladder out, the doctor said she was a “4F textbook case” because she had a family history and was female, fat and forty-plus.
You can’t change your genes, but there are some food and lifestyle factors you can target to lower your risk. Eat healthily, increase your fibre intake, eat more fruit and vegetables high in vitamin C and drink coffee.
Avoid weight gain and if you do try to lose weight, do it slowly.
What does the gallbladder do?
The gall bladder is a storage sac for bile, which is made in liver. After you eat, bile is squirted into the small intestine.
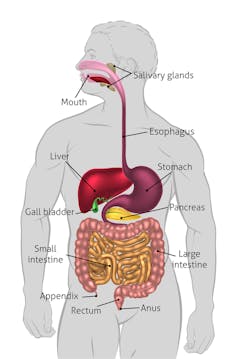
Bile emulsifies or breaks up the fat in the food we eat into tiny particles, a bit like washing-up detergent. This means that fat-digesting enzymes from the pancreas can mix with the fats from foods and break them down into smaller particles that can be absorbed.
What are gallstones?
Gallstones form in the gall bladder when components of bile, such as cholesterol and bilirubin (a breakdown product of red blood cells), aggregate and form stones.
These stones vary in size from single large hard stones about the size of an apricot and made mainly from cholesterol, to small pebble-sized stones made mainly from bilirubin. Gallstones can also be very tiny, like a grainy sludge.
How can you prevent gallstones?
The good news first. Having a healthy diet lowers your risk of getting gallstones.
In a US study that followed more than 13,000 adults over ten years, women with higher blood levels of vitamin C had a lower chance of developing gall bladder disease. This was not the case for men.
Foods high in vitamin C include capsicum, cabbage, Brussels sprouts, cauliflower, broccoli, green leafy vegetables, tomatoes, citrus fruits, pawpaw, kiwi fruit, strawberries and pineapple. You could try vitamin C supplements, but studies are inconsistent and taking vitamin C supplements can increase the risk of kidney stones.
A higher fibre intake is also associated with lower risk. There is no need to become vegetarian, but eating more legumes, pulses, wholegrains, vegetables and fruit boosts fibre intake.
A review of studies involving more than 200,000 people found people who drank a lot of coffee (four cups or more a day) had a a reduced risk of gallstone disease. However, some studies found this association in women only.
Having a moderate alcohol intake is also associated with a lower risk of gall bladder disease. But it’s wise to drink in line with current guidelines, which recommend no more than two standard drinks on any day.
Rapid weight loss
Losing weight at a rate of more than 1 to 1.5 kilograms a week is considered rapid and increases the risk of gall bladder disease.
When you markedly cut back your total food and fat intake, you need less bile. Your gall bladder doesn’t need to contract as much and bile salts become more concentrated. This means gallstones are more likely to form.
Cutting down on foods that contain large amounts of fat is a good idea because you reduce total kilojoule intake as a result and therefore lose weight. To ensure your gall bladder still contracts and keeps excreting bile, still consume some fat, around 20 grams, each day.
Other risk factors
Risk factors such as body weight, using hormone replacement therapy and number of pregnancies are theoretically modifiable. Others, such as age and being female, are not. Women are twice as likely as men to get gallstones, due to higher oestrogen levels.
Around the world, Pima Indians have the highest rate of gallstones at 70%, compared to 10-30% among Europeans and North Americans and less than 5% in Asian and African populations.
Treatment
Treatment for gall bladder disease depends on size and location of the gallstones, whether you have other symptoms such as pain and infection, and whether you have other medical conditions.
Silent gallstones are ones that cause no symptoms and generally are not treated. Other approaches include the dietary changes mentioned earlier, lithotripsy for small stones, or surgery to remover the gallbladder along with the stones. See your doctor for advice.
What happens after your gall bladder is removed?
Once your gall bladder is removed, bile can no longer be stored, but trickles constantly into the small intestine.
Your digestive tract will make some adjustment after the surgery, but if you eat a large fatty meal, your body is not able to squirt in extra bile. This means some undigested fat passes through the small intestine and travels into the large bowel where bacteria will try to break it down.
However, a lot of the fat will be malabsorbed, triggering steattorhoea, which means fatty diarrhoea. Some fat-soluble vitamin A and E will be lost in the stools as well.
Boost your intake of these vitamins by eating foods that are good sources of them. The vegetable form of vitamin A, called beta-carotene, is found in dark yellow, orange and dark green vegetables, such as pumpkin, carrots, sweet potato, spinach and broccoli.
Good sources of vitamin E include nuts, seeds, wholegrains, peanut butter, tahini, spinach, broccoli, tomato, avocado, kiwifruit and mango.
When it comes to gallstones, food should be part of prevention and treatment strategies.

