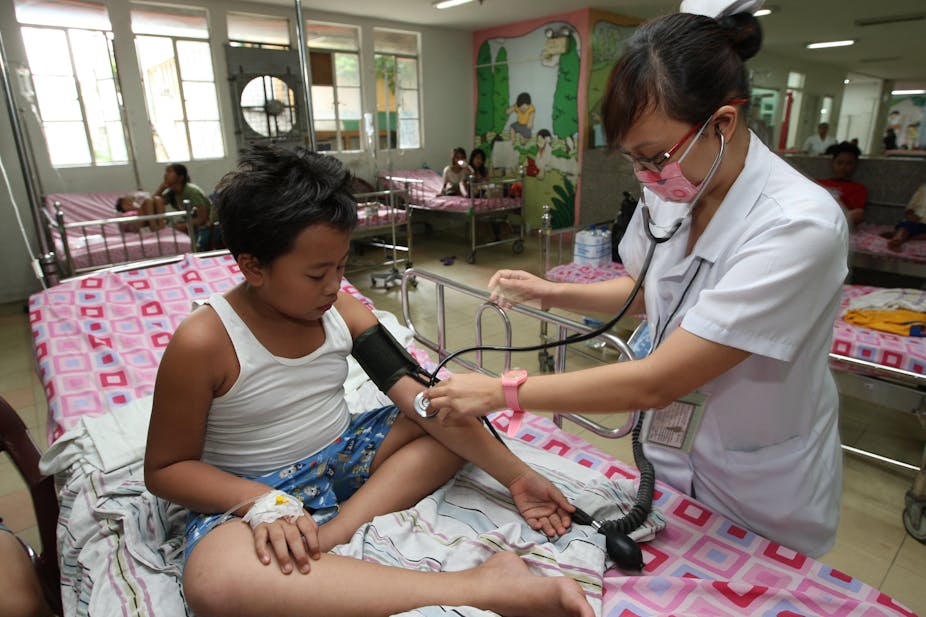
Thousands of foreign nurses could be forced out of the UK under new immigration rules, the Royal College of Nursing has warned. Changes to immigration policy under the government’s attempt to drive down migrant numbers mean that those earning less than £35,000 a year will have to leave the UK after 6 years. This means up to 3,365 nurses currently working in the UK, whose recruitment cost more than £20m in total, could be affected.
The Royal College has warned the consequences of an exodus of foreign nurses would be serious and could jeopardise the ability of the country’s National Health Service (NHS) to function. In London alone, nearly a quarter of doctors and half of nurses are from abroad.
This comes at a time when the NHS needs to change to meet the healthcare needs of a growing, ageing population and when the government is pushing for seven-day primary care services. Researchers estimate the demand for nurses is already outstripping supply by nearly 50,000 for the period between 2010 and 2016.
This problem is made worse by nursing’s high rate of turnover. An estimated 10% of the nursing workforce are seriously contemplating leaving for various reasons including burn-out. Nurse turnover rates tend to be higher in teaching trusts, in specialisms such as mental health and elderly care, and in inner cities – especially in London, where turnover rates can be as high as 38%.
This high turnover can reduce the quality of patient care and affect the ability of the NHS to meet demand. But it also costs the NHS a significant amount of money as turnover costs can cost up to double the salary of the nurse that left.
There has been at times unfair tabloid reporting that foreign healthcare workers take local jobs, draw on local benefits, offer substandard practice and take money out of the system. The reality is that many do jobs in areas that home-grown healthcare workers do not want. Many face a degree of discrimination and career glass ceilings, despite often being highly skilled. The fact of the matter is that foreign healthcare workers help keep the NHS going.
International competition
But there is also a much wider issue: that of the globalised trade of healthcare workers. It is estimated that around 53% of Indian medical graduates and up to half of South African medical graduates emigrate to developed countries. Similarly, more than 150,000 Filipino nurses and 18,000 Zimbabwean nurses emigrate to countries where pay and conditions are significantly better.
This is not a new phenomenon. Indeed, a previous survey carried out by the British General Medical Council in 2002 reported that 58% of newly registered doctors in the UK were trained abroad. This situation has improved somewhat, according to 2015 statistics which show that international medical graduates account for just over a quarter of all newly registered doctors. That said, the overall number of international medical graduates in the UK has been fairly static in the past decade.

There is also an issue of global inequity. Many of the countries that export doctors and nurses to high-income countries themselves face staffing shortages in the health sector and can ill afford to lose them. For example, India has just 171 registered nurses per 100,000 people and yet it exports many of the nurses it trains to the UK, which has nearly five times as many nurses (880) per 100,000 population. The healthcare brain drain deskills the donor health systems of other countries and threatens their viability. Ultimately this contributes to global health inequalities.
What’s more, not only are the countries of origin losing a valued and skilled human resource, but they are also losing the upfront investment costs required for training them. For example, each emigrating African doctor represents a loss of more than US$184,000 (£116,000) to the continent.
Cheap solution
In the UK it costs around £70,000 to train a nurse from scratch, £479,000 for a general practitioner, and £725,000 to train a hospital consultant. It is therefore not surprising that the UK health economy makes a considerable saving in recruiting foreign staff that are already trained. But there is an ethical dimension to international health worker recruitment and migration. It could be argued from a moral standpoint that high-income countries which recruit international healthcare workers – such as the UK – should recompense the countries of origin.
The NHS relies heavily on foreign staff and it is unlikely that it can wean itself off this need in the near future. Undoubtedly, the long-term solution will be to train more home-grown health care staff. But this strategy will come with significantly long lead times and require considerable investment in health education and training.
Careful cross-departmental planning by the government is essential to ensure a smooth and safe transition. Until such a time is reached when the UK is self-sufficient in healthcare staff, foreign workers will continue to be needed. This creates problems for an immigration policy that aims to prevent their arrival and might even send them home.