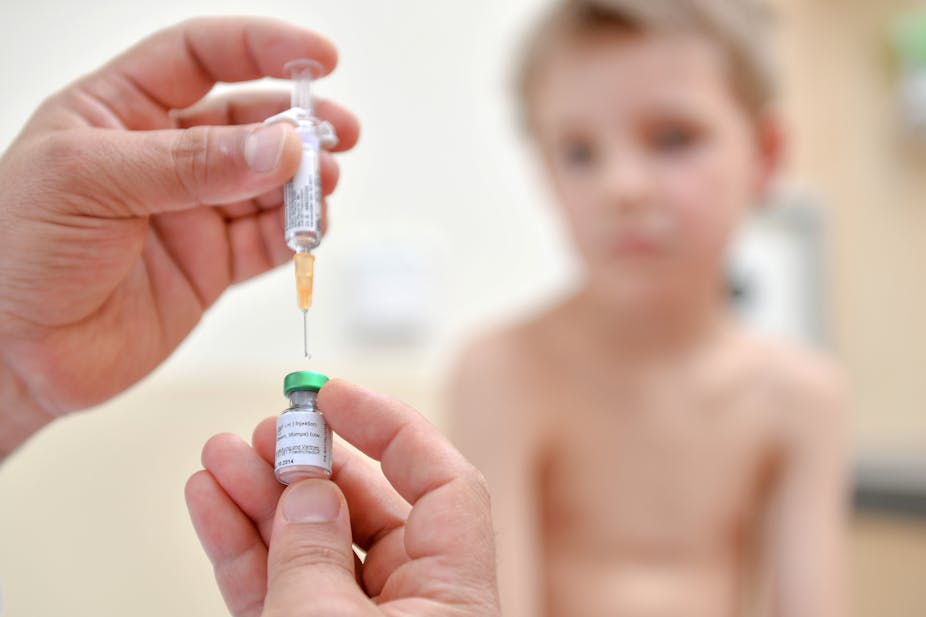
More than 30,000 children will have started school this term without being vaccinated against measles, mumps and rubella (MMR) amid a startling increase in cases of measles in England and Wales.
In 2018, there were 991 reported cases of measles in the UK, after which the World Health Organisation was obliged to withdraw the UK’s measles-free status, which was awarded in 2017. This raises questions about why some people are still choosing not to vaccinate their children.
Most people in the UK accept that vaccination is safe and effective at preventing the suffering associated with preventable disease. But the proportion of children in the UK who aren’t up to date with their MMR vaccinations seems to be increasing. This may have less to do with access to information than it does with social factors.
Many experts wonder why this is the case, given that there is abundant, clear and readily available evidence for the safety and effectiveness of routine vaccinations. There is no single answer to this question. Parents and guardians who don’t vaccinate their children are a mixed group with varying views on vaccination.
Some might not vaccinate due to a lack of engagement with healthcare services. Others might worry about the side effects of the vaccines. Vaccination might not be a part of their cultural or societal norms, or it might be at odds with their religious views. Others may mistrust expert opinions that advocate for vaccination – they may take the facts about vaccine effectiveness and safety to be fake truths.
Some of the people who reject the evidence for the benefits of vaccination become dedicated “anti-vaxxers”, people who eschew vaccination altogether. A larger group of people who are suspicious of vaccination become “hesitant” and delay or pick and choose from the vaccination programme.
It is often suggested that if only anti-vaxxers and vaccine-hesitant groups could be convinced of the evidence for vaccination they would be converted away from their position. But our latest research suggests that far from being the result of ignorance, vaccination hesitancy is found even among certain medical professionals.
Cliques of ‘yes’ and ‘no’
When we asked junior doctors about their thoughts about taking the seasonal flu vaccination, many had similar concerns to what we might expect from the general public. Some were worried about potential side effects or said they didn’t have time to vaccinate themselves, or even mentioned a dislike for needles.
Some junior doctors avoided vaccination because they previously experienced a physical reaction. Others were influenced by the practices of colleagues, or importantly, because their social group was against it.
One junior doctor said she would avoid the vaccination because her friends were avoiding it. She felt that, on vaccination “there are little cliques of the ‘yes’s and the 'no’s”.
So it seems that even some doctors, who are trained to be advocates of vaccination, and are more able than most to access the relevant scientific literature, can be hesitant about vaccination.
Whatever the reasons behind non-vaccination, the fall in MMR vaccine take up is worrying public health professionals. Measles, mumps and rubella can have serious health consequences, both for sufferers and for those they come into contact with. Not every child can be vaccinated, often because they have a compromised immune system. But if nearly everyone is vaccinated, the spread of the disease is effectively halted, a feature known as herd immunity. Because measles, in particular, is very contagious, at least 95% of the population needs to be vaccinated to gain this immunity.

Herd immunity is one reason why some vaccine-hesitant or vaccine-averse parents have children who, though never vaccinated, have not yet contracted the disease. It is not, as some parents claim, down to their use of alternative medical practices.
The average level of vaccination in the UK is likely to vary from place to place. Whereas in some places it may be above or at the 95% mark, in others it may be below. In these latter areas, outbreaks are more likely.
Some doctors are now calling for compulsory MMR jabs in schools to put a certain stop to the spread of measles. As our research shows, appealing to the rationality of parents doesn’t always work, and so this approach may only stir up more opposition.
To reach the anti-vaxxers and vaccine-hesitant parents, we need to understand the complex and varied reasons people avoid vaccination, rather than assuming they are ignorant.