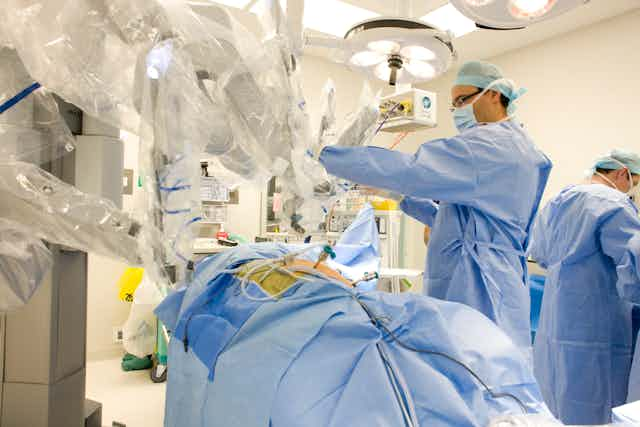
A spider-like robot moves over an anaesthetised patient, deftly making controlled incisions with flexible arms while a surgeon sitting a couple of metres away peers through a console offering highly-magnified, high definition, three-dimensional vision of internal organs and the operating field.
It may surprise you to learn that robot-assisted surgery is far from science fiction – in fact, robots have been used to perform surgical procedures in Australia now for 10 years.
Robotic assisted surgery uses the da Vinci surgical system, which replaces a standard 2D camera with 3D binocular vision, and offers articulating “wristed” instruments instead of the straight, rigid handheld instruments used for keyhole (laparoscopic) surgery.
Controlled from the surgical console, movements are finely scaled and any surgical tremor is filtered. Since 2003, robot-assisted surgery has replaced open and standard keyhole surgery for certain complex procedures in a number of hospitals, with more than 3,500 robotic procedures being performed in Australia in 2012 alone.
At a cost around A$3million per machine, the da Vinci allows surgeons the best possible vision, dexterity and ergonomics to reduce the operative risks and achieve the best possible results.
Advances in robotic surgery have given surgeons dexterity and control that would be impossible with human hands.
Rise of the machines
Robot-assisted surgery is predominantly used in Australia for the removal of prostate and kidney tumours as well as for uterine surgeries and cardiac procedures.
Other specialities are increasingly using this system for bowel tumours and, recently, operating deep down the throat on the base of tongue. Previously, to remove cancers from this area, the jawbone had to be split and opened like a book.
The advance of surgical robots coincided with the increasing prevalence of the prostate-specific antigen (PSA) test, which detects potential prostate cancers very early in their development. Previously, prostate cancers usually reached a more advanced stage before medical intervention.

Surgery to remove the prostate before PSA testing was risky and interfered with quality of life. Removing prostates is delicate due to the proximity of important tissues that control urinary and reproductive functions.
These are risks that patients accept when there is a bulky, aggressive tumour that could be life-threatening, but not for example if they are young men with an early cancer and no symptoms.
In the US, the majority of all prostate cancer operations are now performed robotically while in Australia, that number is around 25%.
The robots help surgeons with precision, control and visualisation. They use sophisticated instruments to scale movements millimetre by millimetre. The 3D camera gives an unsurpassed view of areas inside the patient and the flexible arms can reach tiny restricted areas with minimal cutting to other tissues.
Because of the reduced risk of infection and faster recovery, the robot changed surgical options for patients when it was introduced. Most patients could be discharged on the first or second day after surgery and were able to return to normal activities within a few weeks.
Pain was rarely a major problem, due to the small scars left by the keyhole procedure, and it was rare that patients required a blood transfusion after this type of surgery.
From a distance
This kind of machine was born from technology developed for two similar, yet different purposes:
- the need for astronauts to repair satellites from within the safety of a space shuttle
- an idea to operate on wounded soldiers in the battlefield without placing surgeons on the front line.
Both applications require instruments that can be minutely controlled from a distance as well as excellent images of the procedure sent back to the operator.
An added benefit for today’s surgeons is that the ergonomics of operating is kinder to their bodies.
Instead of many hours on their feet, bending awkwardly, the surgeon sits comfortably at the console away from the operating table. There, he or she controls the surgical instruments with sensitive thumb and finger grips. Foot pedals control the camera which, in the new generation of the da Vinci, can include ultrasound.

The system is calibrated to the surgeon so that his or her hand movements are robotically scaled down and translated into minute adjustments of the instruments working inside the patient.
There are more than 1,000 machines in operation around the world with 25 installations in Australia over the past 10 years. While initially used in the US for prostate and gynaecological surgeries, robots are now being used for increasing types of surgeries, including cardiac, colorectal, thoracic and ear, nose and throat procedures.
There is a question of cost when it comes to robotic-assisted surgery. For hospitals, the purchase price of each machine is one consideration, but there are ongoing refurbishment costs for one-use parts which, in the private hospital setting, are passed on to the patient if they elect to use the robot.
The next generation
There has been much debate regarding levels of training for surgeons using robotics, and it is critical to remember that the technology simply offers an interface for advanced vision and instrumentation; it is still the skill of the surgeon that is the biggest factor in determining whether the operation is a success.
In the case of prostate surgery, I estimate that a surgeon needs to perform up to 75 to 100 procedures in training before feeling comfortable to operate independently.
Most training takes place in the US, but at Epworth we have installed a dual console for training and collaborative surgery purposes. In 2012, Epworth and Peter Mac surgeons joined forces and introduced a mini-fellowship training program for urological surgeons to advance their skills here in Australia.
But the most amazing aspect is looking back 10 years, observing the revolution in keyhole surgery that has occurred, and realising this is only the beginning.
The 2013 Robotic Symposium is hosted by Epworth HealthCare on November 15 and 16.