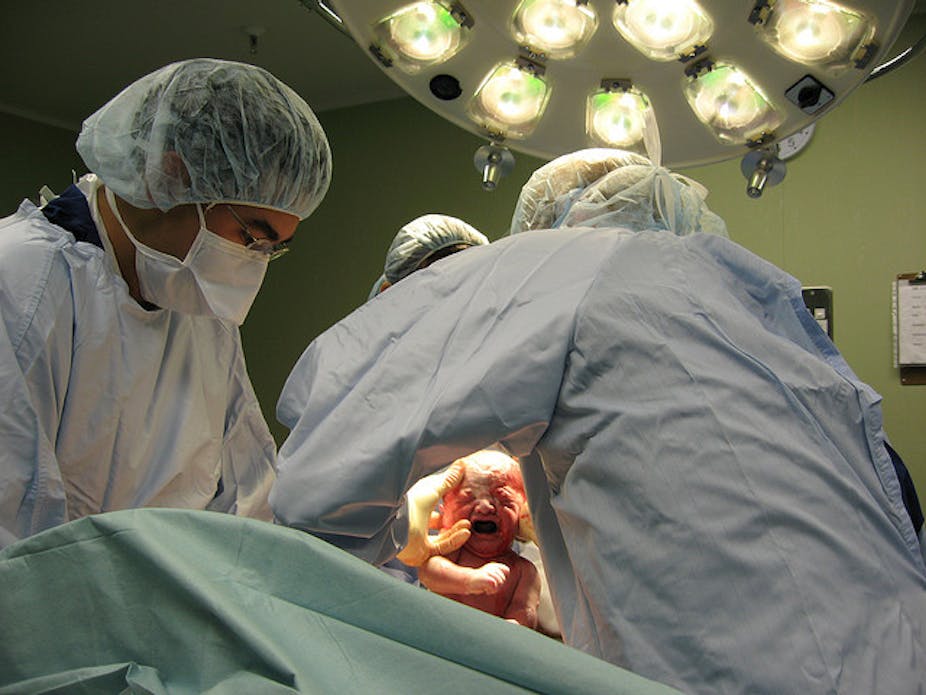
In Australia, as in most of the developed world, about one baby in three is now delivered by caesarean section. To put things in perspective, the rate of caesarean birth has almost doubled over the past 20 years. To say this is controversial is an understatement.
So what’s behind this remarkable change in the way women give birth?
Obstetricians are commonly “blamed” and perhaps there is some truth to this. The younger generation of obstetric specialists have less experience in complex vaginal births, such as breech deliveries, the use of rotational forceps and the delivery of twins.
In fact, many authorities and professional organisations actively try to dissuade specialists for undertaking such births.
Another important factor is the remarkable change in the demographics of women giving birth for the first time. Women having their first babies are now older and heavier than their counterparts 20 years ago.
Recent studies have revealed that the age at which a woman has her first baby has a dramatic effect on the efficiency of labour and her chance of requiring an emergency caesarean delivery.
Similarly, obesity – which is startlingly common now – decreases the chance of achieving a vaginal birth.
But these factors alone can’t account for the entire rise. It’s very likely that a small proportion of caesarean births are performed purely at the request of the woman, with no specific medical reason.
It’s been difficult to determine the proportion of such births, but some research my team did a couple of years ago estimated that 10,000 maternal-request caesarean sections are performed every year in Australia.
So why would a women request a caesarean birth?
It’s important to recognise that women who are aiming for a vaginal delivery won’t necessarily achieve it.
Benchmarking data from Australia reveal that slightly fewer than half of women in their first pregnancies will have a vaginal birth – about a quarter will need an instrumental delivery (with forceps or a vacuum extractor) and the other quarter will have an emergency caesarean section.
When we studied a small group of women who opted for planned caesarean delivery before they went into labour, we found that women were concerned about the welfare of their baby and issues such as genital prolapse and incontinence in the future.
When a woman asks her doctor for a caesarean birth, it’s important that she is counselled about the potential risks, and benefits, of the procedure.
The major problem for doctors is that there is, incredibly, little information about risks and benefits of maternal-request caesarean sections.
The information we have is usually retrospective, and largely extrapolated from studies of caesarean section for medical reasons – where the baby is in a breech position, or the mother is ill, or there is fetal distress, or a previous caesarean section.
No prospective study to date has directly compared the risks and benefits of a caesarean section in a healthy women with no obstetric problems, with women aiming for vaginal delivery (knowing that only about half will achieve a spontaneous vaginal birth). Clinicians have long recognised these limitations.
There is evidence to suggest some advantages in planned caesarean birth.
The nearest thing we have to a randomised study of the outcomes for women, the so-called “term breech trial”, actually shows that the short-term outcomes for the women themselves are almost equal.
The effect of caesarean sections on longer term outcomes such as prolapse remain a mystery.
Our new study is attempting to provide some information for both doctors and the women they care for.
It’s probably impossible to have a prospective trial where healthy women are randomised to have either a caesarean delivery, or to try for a vaginal birth.
The next best thing is a prospective trial where our study groups are taken from women who ask for caesarean birth and women who want a vaginal birth.
Our survey questions will be delivered to women by email, so that they can answer our questions on-line at a convenient time.
If we can recruit about 500 women into each of the two groups, we should have suitable statistical power to make a valid comparison of such things are satisfaction, breastfeeding rates, fatigue levels, pain levels, common complications, and longer-term outcomes such as the desire for more children.
But there are limitation on the data we’re able to collect, this includes rarer outcomes, such as embolus, or maternal death.
The study isn’t perfect, but it’s the first large-scale attempt to make the comparison, using modern research methods. So wish us luck!
For more information on the caesarean study visit the website.