A new legal template for fighting medicine crimes around the world is being developed by the United Nations. The first 39-page draft of the document was unveiled at a meeting in Vienna last month.
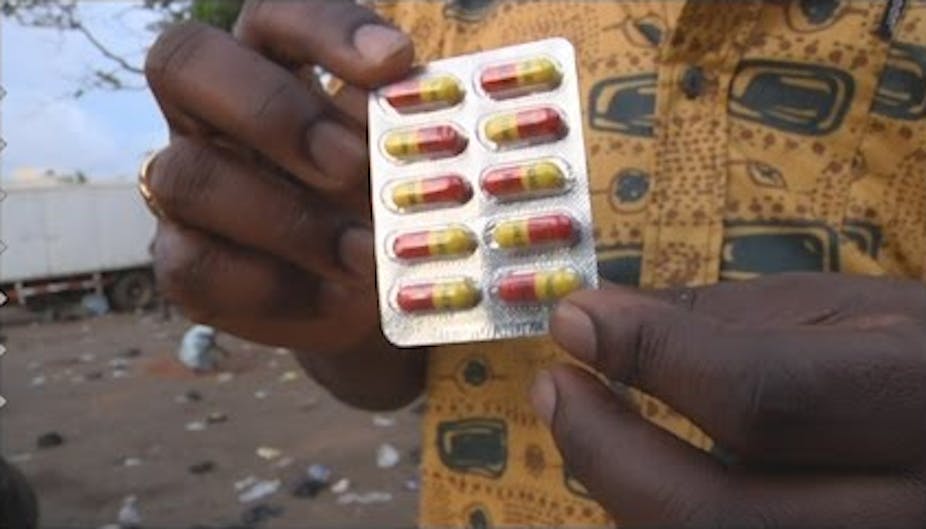
The aim of the proposed “model law” is to address the dangers of medicines that have been criminally falsified, often because they contain no active ingredient, and substandard medicines that have been recklessly made because drug manufacturers have cheated or cut corners.
Counterfeit medicine, which counts as brand or trademark theft, was originally excluded from the proposal on the recommendation of Amir Attaran, law professor and lead consultant to the UN Office on Drugs and Crime (UNODC), because it is widely seen as coming under intellectual property law – a matter usually dealt with by the World Trade Organization. Unfortunately, UNODC came up with different draft provisions that criminalise all sorts of medicine fraud, including counterfeiting trademarks.
Intellectual property
There has been much consternation among health advocates and certain countries like Brazil and India about conflating quality, safety and efficacy of medicines with intellectual property rights. For many, intellectual property is a tool used by pharmaceutical companies to limit access to affordable medicines. In lumping all sorts of medicine fraud together – some directly related to health (quality fraud) and some related to brand theft (trademark fraud) – UNODC is dabbling in intellectual property, creating confusion and setting up a clash with health advocates.
UNODC’s decision is one of a number of serious problems in how this model law has been forwarded, which includes a failure to take a stronger position on substandard medicines and worryingly, the exclusion of a whole host of key players from the consultation process – vital for this kind of law to be accepted by individual countries and translated into effective national laws.
Not just about criminal gangs
Falsified and recklessly made substandard medicines can kill because they fail to treat medical conditions and can even be directly toxic. There are no accurate estimates, but some experts have said that the cost may be as high as tens of thousands of lives a year.

Health advocates are naturally concerned about deliberately falsified medicines, but they are equally concerned about recklessly made substandard ones, regardless of who makes them. Yet the UNODC meetings on this issue and the legal draft have narrowly focused on the most obviously faked products produced by criminal gangs, and not the wider problem.
As recent findings from the US Food and Drug Administration (FDA) have shown, it is not just criminal gangs that act fraudulently – there are instances of large firms doing so too. Ranbaxy, for example, pleaded guilty in the US to falsifying testing data for its products, which it allegedly did on a massive scale, for 200 medicines in 40 countries. This included faking tests that proved the products could enter the human bloodstream and would remain stable in their packaging.
Elsewhere, in Pakistan, Efroze Chemical Industries made a series of reckless decisions that caused its workers negligently to insert the wrong ingredients into a heart medicine, which killed over 200 people.
UNODC would be wise to address these firms too. By focusing on obviously intentional offences of criminal gangs only, UNODC is downplaying the risks of rogue companies that cheat or act recklessly. UNODC is even departing from its own Bible, the UN Convention on Transnational Organised Crime, which states that intent can be inferred from “objective factual circumstances”.
It has long been true that gross negligence, while not the same as premeditated intent, can be criminal too, and this is especially the case in regulated industries like pharmaceuticals, food and automobiles, which makes UNODC’s refusal to take a broader focus very strange.
Lack of representation
The consultation process – which brought together more than 20 experts from different countries and organisations over three days in Vienna where the draft was unveiled – also raises questions over the UN’s understanding of balance and fair representation. More than 90% of participants came from Europe, with only one participant from Nigeria representing African interests, and no North Americans, South Americans or Asians – major countries such as the US, India, Brazil, Russia and China were not party to the discussions. From Europe, Germany and Italy were also not present.
European dominance probably explains why some of the draft provisions that UNODC drafted during the consultation copy whole passages directly from European law.

For an organisation that prides itself on representing 193 member states, one wonders if this situation represents a throwback to an age when a few of European countries ran the world. It is also especially curious given that Argentina, which sponsored the 2011 UNODC resolution that gave them the mandate to do this work, was also not present.
NGOs were also excluded from UNODC’s consultation, with one exception. UNODC invited and collaborated with the International Institute of Research Against Counterfeit Medicines (IRACM), a French NGO that is allied with a pharmaceutical company and describes itself as “an initiative of the Sanofi group”. Given that NGOs are key players in public health policy and often represent health professionals such as doctors and pharmacists it is worrying that they will not have had a say.
Like Attaran, I have raised concerns about this lack of sectoral and geographical representation – but these have gone unheeded. However, it certainly gives some insight into the complex politics of interests underlying UNODC’s consultation and legislative processes. Indeed, after Attaran suggested consulting the public health community before producing the next version of the model law, he was placed under a gag order by UNODC.
What is clear is that without input from people involved in public health, who are also widely trusted by the wider public, a model law like this is doomed not to find favour with legislators, and will fail.
UNODC - truly independent?
UNODC copied some of its draft provisions from yet-to-be-ratified legislation from the Council of Europe – specifically the Medicrime Convention aimed at combating the illegal trade in medical products – in the development of this model law. Also, the Council of Europe sent more representatives to the consultation meeting than even the World Health Organisation.
It seems UNODC is working closely with the Council of Europe to serve its interests in pushing forward the Medicrime Convention, which as many others have written in The Lancet and the British Medical Journal has serious problems, including unjustifiably criminalising some generic medicines.
In this regard one may legitimately wonder about UNODC independence.
The French government has also previously directly funded UNODC’s fight against fraudulent medicines. It is excellent that France cares to support UNODC’s work in this effort, but given that a good number of the experts involved in the consultation were French (working for UNODC, Council of Europe and Interpol) and/or representing French interests, including Sanofi, we need to be careful about how much influence this one player has and whether the entire world is willing to follow suit.
The UN’s stated aim is “to work together to help people live better lives”. But if UNODC alienates the health professionals and excludes most of the world’s population from the process – Asia and the Americas for example – then this model law will never be globally adopted, and nothing will change – and those tens of thousands of lives will not be saved.