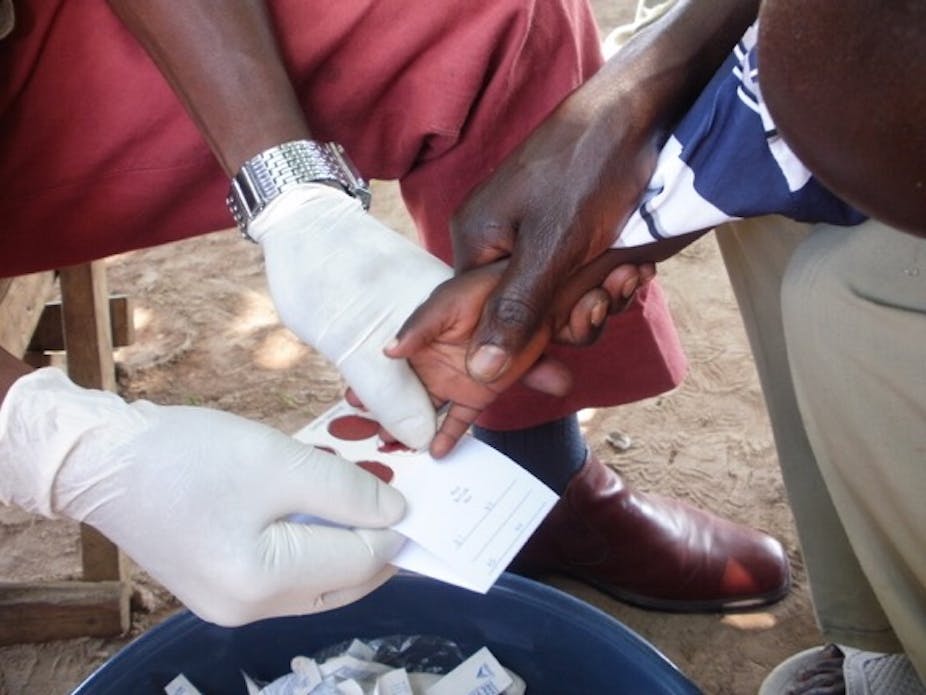
The current outbreak of Ebola in West Africa (and perhaps elsewhere) and now Marburg Fever, a related a hemorrhagic fever virus in Uganda, has generated much talk about the collective “failures” to pre-empt and control disease.
Alongside a slow international response, the blame has been placed on weak and ineffective health systems in sub-Saharan Africa. While largely true, this is of little help in thinking through what to do next? Effective systems that can ensure healthcare provision and disease surveillance would be ideal but remain a longer-term project in many parts of the world.
A further complication is that these zoonotic diseases where infections take places between humans and animals often have complex transmission patterns that are not always fully understood. What examples might guide future responses to complex, zoonotic and potentially global infections? A “One Health” approach – in which human health, animal health and environmental factors are monitored and addressed in an integrated manner has emerged as a policy aspiration – particularly following the Avian influenza outbreaks since 2003. What does it take, however, to make such co-ordination and planning a reality?
Important examples of success exist. Efforts to control and eliminate African Trypanosomiasis (known as “sleeping sickness”) in Uganda make an instructive case in tackling a highly complex disease. Sleeping sickness control is difficult because of the sheer intricacy of the disease: the vector (the tsetse fly) is difficult to control, what drugs are available to treat the disease are toxic and are thus dependent on a positive diagnosis, which in itself presents major technical problems.
Sleeping sickness
Trypanosomiasis is found across a large belt of Sub-Saharan Africa. There are two forms of the human disease, roughly separated by the Rift Valley: An acute, zoonotic form, found in eastern and southern Africa, and chronic, non-zoonotic form, found throughout western Africa. Uganda is the only country where both forms exist. This creates a huge problem as it is difficult to distinguish the two diseases and each requires a different treatment regime.
Tsetse and trypanosomiasis control and eradication programmes in Africa have a long history – and from the colonial period until the 1960s, simple control programmes based on active surveillance of human cases and ecological interventions in the tsetse habitat were largely successful. However, the disruption of the independence period and complacency driven by a relatively small number of cases led to a decline in attention – and, by the 1980s when the disease re-emerged with a vengeance, there was no capacity to control it. Further flare-ups occurred in the 1990s, from 30,000 cases reported annually, it was estimated that 300,000 cases went undiagnosed.
Today, the treatment of sleeping sickness is managed entirely through Uganda’s decentralised healthcare delivery system, which conducts diagnosis and treatment (with free drugs donated through a WHO donation scheme). Additionally, a government department that cuts across ministries is responsible for co-ordinating research and disease control projects.
If Uganda’s efforts to control the sleeping sickness of the 1980s and 1990s in some ways foreshadow the challenges West African nations will face in controlling a recurring and potentially endemic Ebola outbreaks, what lessons can be learned? This is a complex story, but one message is the importance of weaving international programmes into national structures.
International humanitarian responses
With its current caseload of several hundred sleeping sickness cases annually, Uganda is able to manage the disease without external assistance. In the past, when caseloads were much higher, humanitarian organisations including Médecins Sans Frontières (MSF) were called upon. MSF’s first involvement in Uganda coincided with the sleeping sickness epidemic of the late 1980s – the NGO initiated its first sleeping sickness programme in the Moyo district of northern Uganda in 1986 to provide mobile treatment on a mass scale.
Since then, various MSF missions have run finite programmes in the country, with notably differing aims and relationships with the national sleeping sickness infrastructure. The last mission left the country only in 2011. Today, despite maintaining no field presence in Uganda for sleeping sickness, MSF continues to play an important role in the supply of medication to Uganda.
Over recent decades, MSF’s work has become sustained, a role that contrasted with MSF’s traditional emphasis on tackling emergencies. Our interviews with senior Ugandan officials suggest that the combination of MSF’s mission creep along with a singular way of working meant that while the organisation provided crucial surveillance and treatment, it did not always co-ordinate with the Ugandan government or share protocols or training.
The re-emergence of the disease led to the setting up of a Co-ordinating Office for Control of Trypanosomiasis (COCTU) in Uganda. The office’s mandate is to co-ordinate the activities of all involved government departments, donors and non-governmental organisations. In many ways the MSF presence in Uganda in the 1980s was largely the spur for the organisation being set up. As one Ministry of Agriculture official recounted in April 2013:
Before the birth of COCTU, we had several players, I think over 15 [organisations], doing tsetse and trypanosomiasis … We had so many organisations when we had the epidemics here. And there was a need to have them controlled. You could find we had the French supporting trapping, we had ODA doing something, we had MSF-France, MSF-Swiss, MSF-what, all those.
Collaboration, crisis and co-ordination
Thus, the office was created to bring order to the post-conflict and mid-epidemic chaos of the late 1980s and early 1990s. Its activities in the two decades since its establishment are an attempt to coordinate and harmonise various external actors involved in trypanosomiasis control.
In many ways this represents a concrete, operating form of “One Health” co-ordination. Perhaps it also suggests a template for controlling Ebola or Marburg, once international attention and programmes begin to wane. This is not to say that sleeping sickness control in Uganda is a straightforward success story: many health resources are focused elsewhere – on HIV/Aids or malaria – or are spread too thinly and devolved too far. Still, sleeping sickness may be a neglected disease, forgotten and virtually unfunded, but Uganda’s coordination more or less keeps it in check.
Like Ebola, sleeping sickness is a killer. Also like Ebola, it is zoonotic so requires care and thought in designing a management and elimination plan. While we may know much more about the epidemiology of sleeping sickness, the fact that Ebola can so readily threaten the West means that will not remain the case for very long.
Tackling sleeping sickness in Uganda demonstrated that emergency humanitarian interventions may not be perfect or sustainable – and they can ruffle a few feathers. But such assistance is nonetheless useful and can be “tamed” and domesticated over time. Ultimately, sleeping sickness as a case study shows what is possible when national authorities embrace an ethos of multi-sectoral collaboration.
Ebola currently constitutes a far greater threat – and it is encouraging to know that possibilities exist between the reality of weakened health systems and the impossibility of simply and quickly “strengthening” them.