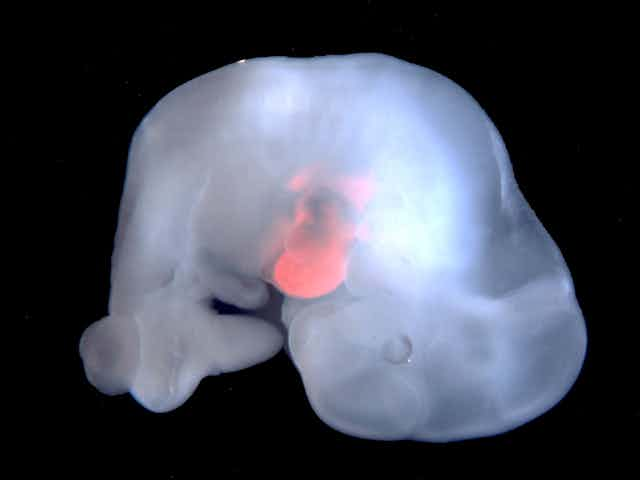
A team of scientists from the Salk Institute in the United States created a stir last week with the announcement that they had created hybrid human-pig foetuses.
The story was widely reported, although some outlets took a more hyperbolic or alarmed tone than others.
One might wonder why scientists are even creating human-animal hybrids – often referred to as “chimeras” after the Greek mythological creature with features of lion, goat and snake.
The intention is not to create new and bizarre creatures. Chimeras are incredibly useful for understanding how animals grow and develop. They might one day be used to grow life-saving organs that can be transplanted into humans.

Potent cells
The chimeric pig foetuses produced by Juan Izpisua Belmonte, Jun Wu and their team at the Salk Institute were not allowed to develop to term, and contained human cells in multiple tissues.
The actual proportion of human cells in the chimeras was quite low and their presence appeared to interfere with development. Even so, the study represents a first step in a new avenue of stem cell research which has great promise. But it also raises serious ethical concerns.
A chimera is an organism containing cells from two or more individuals and they do occur in nature, albeit rarely.
Marmoset monkeys often display chimerism in their blood and other tissues as a result of transfer of cells between twins while still in the womb. Following a successful bone marrow transplantation to treat leukaemia, patients have cells in their bone marrow from the donor as well as themselves.
Chimeras can be generated artificially in the laboratory through combining the cells from early embryos of the same or different species. The creation of chimeric mice has been essential for research in developmental biology, genetics, physiology and pathology.
This has been made possible by advances in gene targeting in mouse embryonic stem cells, allowing scientists to alter the cells to express or silence certain genes. Along with the ability to use those cells in the development of chimeras, this has enabled researchers to produce animals that can be used to study how genes influence health and disease.
The pioneers of this technology are Oliver Smithies, Mario Cappechi and Martin Evans, who received a Nobel Prize in Physiology or Medicine in 2007 for their work.
More recently, researchers have become interested in investigating the ability of human pluripotent stem cells – “master cells” – obtained from human embryos or created in the laboratory from body cells, to contribute to the tissues of chimeric animals.
Human pluripotent stem cells can be grown indefinitely in the laboratory, and like their mouse counterparts, they can form all the tissues of the body.
Many researchers have now shown they can make functional human tissues of medical significance from human pluripotent cells, such as nerve, heart, liver and kidney cells.
Indeed, cellular therapeutics derived from human pluripotent stem cells are already in clinical trials for spinal cord injury, diabetes and macular degeneration.
However, since 2007 it has been clear that there is not one type of pluripotent stem cell. Rather, a range of different types of pluripotent stem cells have been generated in mice and humans using different techniques.
These cells appear to correspond to cells at different stages of embryonic development, and therefore are likely to have different properties, raising the question about which source of cells is best.
Creating a chimeras has long been the gold standard used by researchers to determine the potential of pluripotent stem cells. While used extensively in animal stem cell research, chimeric studies using human pluripotent stem cells have proved challenging as few human cells survive in human-animal chimeras.
Medical possibilities
Although the number of human cells in the chimera was low, the findings by the Salk Institute researchers provide a new avenue to address two important goals. The first is the possibility of creating “humanised” animals for use in biomedical research.
While it is already possible to produce mice with human blood, providing an invaluable insight into how our blood and immune system functions, these animals rely on the use of human fetal tissue and are difficult to make.

The use of pluripotent stem cells in human-animal chimeras might facilitate the efficient production of mice with human blood cells, or other tissues such as liver or heart, on a larger scale. This could greatly enhance our ability to study the development of diseases and to develop new drugs to treat them.
The second potential application of human-animal chimeras comes from some enticing studies performed in Japan in 2010. These studies were able to generate interspecies chimeras following the introduction of rat pluripotent stem cells into a mouse embryo that lacked a key gene for pancreas development.
As a result, the live born mice had a fully functional pancreas comprised entirely of rat cells. If a similar outcome could be achieved with human stem cells in a pig chimera, this would represent a new source of human organs for transplantation.
Ethical boundaries
While scientifically achieving such goals remains a long way off, it is almost certain that progress in pluripotent stem cell biology will enable successful experimentation along these lines. But how much of this work is ethically acceptable, and where do the boundaries lie?
Many people condone the use of pigs for food or as a source of replacement heart valves. They might also be content to use pig embryos and foetuses as incubators to manufacture human pancreas or hearts for those waiting on the transplant list. But the use of human-monkey chimeras may be more contested.
Studies have shown that early cells of the central nervous system made from human embryonic stem cells can engraft and colonise the brain of a newborn mouse. This provides a proof of concept for possible cellular therapies.
But what if human cells were injected into monkey embryos? What would be the ethical and cognitive status of a newborn rhesus monkey whose brain consists of predominantly human nerves?
It may be possible to genetically engineer the cells so that human cells can effectively grow into replacement parts. But what safeguards do we need to ensure that the human cells don’t also contribute to other organs of the host, such as the reproductive organs?
While the announcement of a human-pig chimera may have taken many by surprise, regulators and medical researchers well recognise that chimeric research may raise issues in addition to the those already posed by animal research.
However, rather than call for a blanket ban or restricting funding for this area of medical research, it requires careful case-by-case consideration by independent oversight committees fully aware of animal welfare considerations and recognising existing standards.
For example, The 2016 Guidelines for Clinical Research and Translation from the International Society for Stem Cell Research call for research where human gametes could be generated from human-animal chimeras to be prohibited, but supports research using human-animal chimeras conducted under appropriate review and oversight.
Chimeric research will and needs to continue. But equally scientists involved in this field need to continue to discuss and consider the implications of their research with the broader community. Chimeras can all too readily be dismissed as mythological monsters engendering fear.