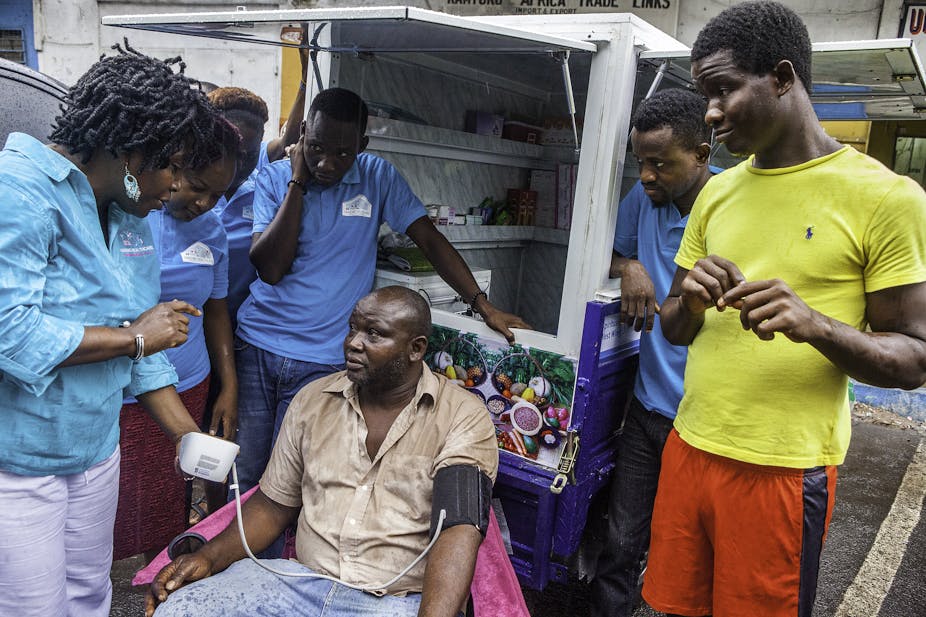Cardiovascular diseases and their risk factors, such as diabetes and high blood pressure, are major causes of death and disability globally. Noncommunicable diseases such as these arise mainly from lifestyle transitions towards a high-calorie diet and low-activity living.
These conditions were previously regarded as a problem for high-income countries. But low- and middle-income countries have followed the same trend. Now more than three quarters of deaths due to cardiovascular disease are in low- and middle-income countries.
Despite this large disease burden, research funding and aid budgets for low- and middle-income countries are still concentrated around infectious diseases, and maternal and child health. The prevalence and treatment outcomes of cardiovascular disease risk factors, such as diabetes and hypertension, are relatively unexplored in these regions.
Our study is one of the first to report that cardiovascular disease risk factors in Sierra Leone are highly prevalent, and the first study to report on access to care for people with these conditions.
Cardiovascular risk factors are preventable or relatively easy to treat with inexpensive medication. But cardiovascular diseases – such as heart attacks and stroke – can’t be reversed and often require intensive and expensive treatment.
Poor countries, such as Sierra Leone, with limited health services can’t treat large numbers of people with cardiovascular diseases. Therefore people with these conditions are likely to die or be permanently disabled as a result. This is a tragedy for the individuals and the families who have to care for them.
Prevalence and access to care
Sierra Leone is one of the least developed and poorest countries in the world. It ranks 181 out of 189 countries in terms of human development. Almost 65% of people in the country are defined as poor on the multidimensional poverty index. Poverty, combined with civil war and the Ebola epidemic, have hindered the development of the health system, leaving services unable to deal with complex cardiovascular diseases.
The country has seen some growth in the economy in recent years. But this might increase the demand for health services in Sierra Leone. In other settings, economic growth has been associated with lifestyle changes that lead to cardiovascular disease risk factors. These lifestyle changes include poor diets and lower levels of physical activity.
If these trends persist, Sierra Leone is likely also seeing an increase in cardiovascular disease risk factors. But there’s been very little evidence to show whether this was the case – until our study was done.
We conducted a household survey from September to November 2018. The participants were over 40 years old and lived in the district of Bo, located in the southern province of Sierra Leone. Survey questions asked about sociodemographic information such as age and gender, and about previous history of cardiovascular disease risk factors. Data was also collected on weight, height, blood pressure, blood sugar, and cholesterol.
We found that over three quarters of people older than 40 in Sierra Leone had at least one cardiovascular disease risk factor. Almost 50% of our study population over the age of 40 had hypertension. Smoking was also common –around 25% of the population – especially in young men.
It was shocking that the prevalence of cardiovascular disease risk factors is so high. We also found that access to care for individuals with diabetes and hypertension was very low – fewer than 10% of sufferers are adequately treated for these conditions.
In order to plan strategies to prevent or treat cardiovascular disease risk factors, it is necessary to show that they are a problem. Until now, there was not enough strong data to do that. The high prevalence of these conditions shown by our study should act as a trigger for health service planners and the people that fund these services to act.
A large proportion of the health system funding in Sierra Leone comes from international aid. In 2017, the country received around $170 million in development assistance for health; $30 million for HIV/AIDS (population prevalence is under 2%), $21 million for child and newborn health, and $14 million for maternal and reproductive health. It only received $510,000 for all noncommunicable diseases, which include cardiovascular disease risk factors. Our study clearly shows that the burden of cardiovascular disease risk factors is disproportionately higher than the amount of funding that goes to the health system to manage this.
Hopefully by showing this information and working with policy makers in Sierra Leone, more attention will be given to preventing and treating cardiovascular disease risk factors.
The way forward
To save lives and promote economic wealth, health system planners and funders need to recognise the extent of the problem and prioritise noncommunicable diseases and cardiovascular disease risk factors in Sierra Leone and other low- and middle-income countries, urgently.
Meanwhile, initiatives to reduce the burden of these conditions are imperative to ensure that individuals, communities, and societies do not suffer from their devastating adverse health and economic consequences.