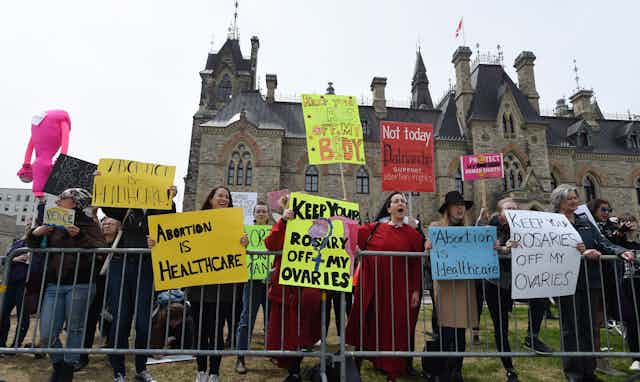This federal election season, abortion is undeniably a campaign issue, with media coverage routinely suggesting abortion rights are tenuous or up for debate.
Conservative Leader Andrew Scheer has declared that he is “personally pro-life,” while insisting that his cabinet will not “reopen the issue.” This does, however, leave the door open for individual MPs to put forward anti-abortion private member bills.

At an NDP town hall on health care in Halifax, NDP Leader Jagmeet Singh criticized abortion access as “abysmal” and vowed to enforce the Canada Health Act to improve it.
Green Party Leader Elizabeth May continues to argue that a woman has a right to a safe, legal abortion while candidates in the party may have conflicting views. Justin Trudeau, leader of the Liberal Party, is “deeply disappointed about "backsliding on abortion rights.”
As a registered nurse who provides abortion care, and as a researcher of abortion access, I worry these news stories create confusion about the reality and legality of access in Canada. Furthermore, news of anti-abortion legislation in the United States seeps north and clouds understanding of our needs and concerns.
The medical abortion pill
In Canada, abortion is unrestricted by criminal law and protected by Constitutional rights to security of the person and protection from sex and gender discrimination.
It is a health service governed by the rules health professional organizations create for self-regulation. Abortion is common. There are around 100,000 abortions annually in Canada and one in three Canadian women will seek an abortion in their lifetime.
Abortion is safe for patients, and most abortion providers in Canada feel safe providing it. The vast majority of procedures take place in the first trimester. Abortion is publicly insured and in the majority of cases is free for the patient.
In 2015, Health Canada approved Mifegymiso, the medical abortion pill. It has been available since 2017 and is effective for use up to nine weeks gestation. Mifegymiso is also publicly insured by all the provinces and territories.
Mifegymiso actually comprises two medications: mifepristone and misoprostol, taken over the course of 24 hours. A week after taking Mifegymiso, patients repeat their blood work. A large decrease in the pregnancy hormone beta HCG confirms a successful pregnancy termination.
Just as some spontaneous miscarriages may need further care, in a small portion of cases, a surgical procedure may be required to complete a medical abortion. Although providers are not required to take specialized training to prescribe Mifegymiso, comprehensive training is easily available.
Lack of ultrasound availability should also not be a barrier, although ultrasound remains valuable for dating a pregnancy and to rule out ectopic pregnancy.
Persistent inequities across Canada
The greatest practical barrier to abortion in Canada is geographic: there are too few providers living in too few places. Surveys of abortion providers here have found most live in large urban centres.
The introduction of Mifegymiso could change this. All physicians and nurse practitioners could prescribe Mifegymiso (there are exceptions in Québec). In theory, every primary care office in the country could be providing this care. This means abortion is potentially more accessible in Canada than in any other country in the world.

But for now, there is stigma and misinformation to contend with. A few persistent inequities complicate matters, making the access landscape seem unintelligible or mystical. For example, New Brunswick does not insure surgical procedures in a clinic outside of hospital. Ontario will not pay for Mifegymiso if you are living outside the province or if you are a non-Ontario resident. Québec will not allow nurse practitioners to prescribe Mifegymiso.
Unlike in the United States, in Canada, nurse practitioners can carry out medical abortion, but not surgical.
Public education is critical
We need to retire all mention of abortion debates and focus on achieving clarity, and universality. The Canada Health Act requires it.
Aligning irregular policies across Canada is the first obvious step. The next is simplifying the path to access by enhancing self-referral processes and reducing wait times for primary care and ultrasound. Expanding the scope of practice of nurse practitioners and midwives to provide both surgical and medical abortion could boost the number of providers.
Most important, however, is increasing factual education about abortion. The public need to know what abortion is and how to get one. Health-care students and professionals need to learn how to include abortion in their practice and how to swiftly and easily refer a patient to the care they need.
Finally, abortion needs to be understood as critical but inadequate for reproductive health. Menstrual health, consent, contraception, trans health services and reproductive mental health all need to make it onto the news, the party platforms and the agenda for our next government.
[ You’re smart and curious about the world. So are The Conversation’s authors and editors. You can read us daily by subscribing to our newsletter. ]