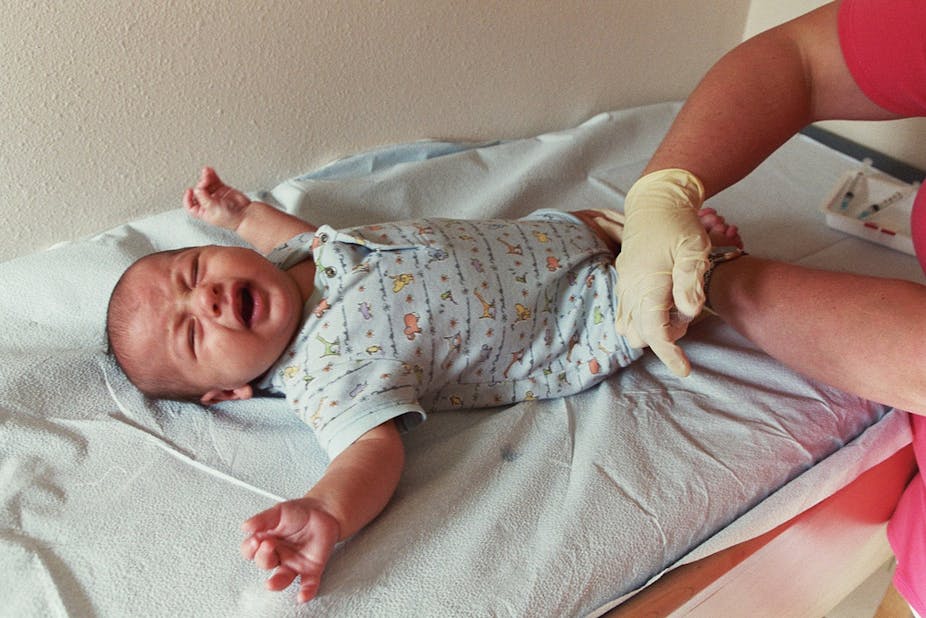
Reports on people suffering an adverse reaction to immunisation focus on the suffering of one over the safety of many. But immunisation benefits the whole community so we should all bear responsibility for those few who experience an adverse reaction to it.
Immunisation works and to the extent that we no longer see people suffering from diseases we immunise against, it is a victim of its own success. Until polio was effectively eradicated through the use of a vaccine, it was not uncommon to see its residual effect among the population. Such sights often motivated parents to immunise their children.
Another worthy example of the positive impact of immunisation is the story of measles in Australia. Only about half of all Australian children received measles vaccines in the 1980s and the illness circulated freely. From 1976 to 1995, 94 children (nearly five children a year) died from severe measles pneumonia or encephalitis (brain inflammation).
But since the 1990s, the proportion of children immunised against measles has risen to over 90%, and there’s only been one death from the illness since 1995 (in 2004). What’s more, there are now only occasional cases of measles in Australia imported from overseas.
About one in every thousand children who catches measles will develop encephalitis. This is fatal for about 5% to 10% and leaves 15% with brain damage. In contrast, only about one in a million children immunised with live measles vaccine (or the measles-mumps-rubella vaccine – MMR) develops encephalitis, which is one child every four years.

In Australia, immunisation is not and doesn’t need to be compulsory because high rates of immunisation are already maintained voluntarily. Most parents recognise that the benefits of measles immunisation far outweigh the risks. Immunisation benefits individual children and the community because a large number of immunised kids means those who have contraindications to measles immunisation, such as those with immune deficiency or whose parents are conscientious objectors to immunisation, are also protected.
This protection is called “herd immunity” and it means when immunisation levels are high, a virus can no longer circulate so even unimmunised children will not be exposed and catch measles.
But suppose a child is unlucky enough to develop severe brain damage as a result of measles immunisation. Their family would inevitably incur out-of-pocket expenses for special needs, such as wheelchairs and modifications to their house and car. Is it fair that a family suffers because their child was inadvertently injured, through neither their fault nor health-care workers’, by a vaccine endorsed and paid for by the community?
By 2010, 19 countries around the world had accepted that society owes a duty of care (or of gratitude) to the very few individuals damaged by a vaccine and had introduced no-fault vaccine compensation schemes. Germany has had such a scheme for 50 years; New Zealand, the United States, Britain and most European countries have compensation schemes – Australia does not.
So what are the barriers to introducing a no-fault compensation scheme for vaccine injury? Would large numbers of people suddenly try to get vaccine compensation? This has not been the case in other countries, which generally appoint expert committees to consider whether cases of possible vaccine injury justify compensation.
Overseas schemes are funded by one of four methods:
a vaccine tax;
special funding for the scheme from general taxes;
industry contribution; or
compensation as part of a broader national compensation scheme (as in New Zealand).
In the United States, where compensation is funded through a vaccine levy, over 2,500 claimants have received compensation since 1989 and the compensation fund is in surplus by about US$3 billion.
Australia is proud of its emphasis on justice and the principle of giving people a “fair go”. It seems only fair someone injured by a vaccine offered and accepted in good faith to benefit the community should be compensated by that community. It’s certainly a better solution than having people not immunise their children and so expose the whole community to a virus.
High rates of immunisation reflect public trust in its benefits and such trust would only be strengthened by the knowledge that the community will look after the few unfortunate casualties of a highly successful immunisation program.