This is part of our series on hidden or stigmatised health conditions in men. Read the other articles in the series here.
Although breast cancer is usually seen as a woman’s disease, around 145 Australian men were diagnosed with breast cancer in 2015, and around 25 died from it. A little under 1% of all breast cancers occur in men, so it is more common than most people think.
There are ethnic differences in the incidence of male breast cancer. In sub-Saharan Africa, 7-14% of breast cancer cases occur in men. In the United States, rates are highest in African-American men, intermediate in non-Hispanic Caucasian men and Asian-Pacific Islanders, and lowest in Hispanic men.
So why do men get breast cancer?
Men also have breast tissue, but usually much smaller amounts than women, and it is exposed to much lower levels of oestrogen and progesterone hormones. We know that men who have relatively high female hormone levels are at increased risk of developing breast cancer.
In rare cases, male breast cancer can be due to specific conditions that result in higher oestrogen levels. Examples include the chromosomal disorder Klinefelter’s syndrome where sufferers can’t produce sufficient testosterone, or taking oestrogens for gender re-assignment, or due to chronic liver disease or obesity, or following loss of a testicle.
What is Klinefelter’s syndrome?
These conditions can also cause benign male breast enlargement (gynecomastia). It may be important for older men with this condition to have it investigated, especially if it’s only on one side.
Men who have had chest radiotherapy are more at risk, and breast cancer usually occurs in men over 70, with a median age of 65 years. Although only two-thirds of breast cancers in women are driven by the female hormone oestrogen positive (known as oestrogen receptor positive or ER+), all male breast cancers are ER+.
A very small proportion of the population carry an inherited predisposition to breast cancer. In families with the breast cancer gene (BRCA1 or 2), breast cancer is more common in the male family members than it is in the general population.
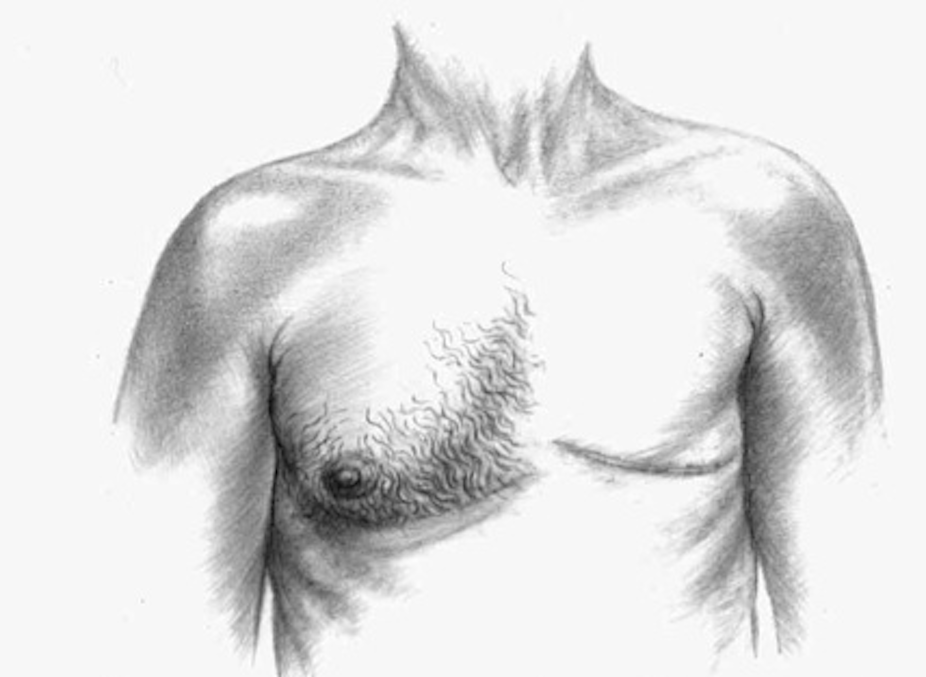
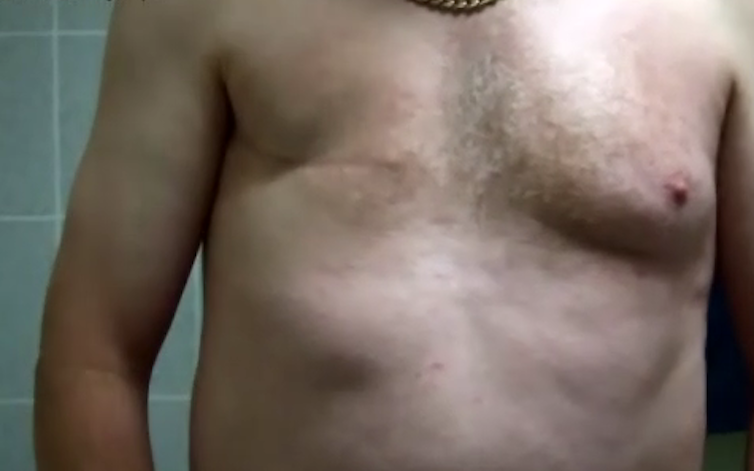
As in women, most breast cancers in men are felt as a hard lump, but other changes can herald cancer. These include nipple discharge or other nipple changes, a change in the shape of the breast, or lumps (lymph nodes) under the arm. These changes need investigations including a mammogram, ultrasound and biopsy.
The survival rate for ER+ cancers is very good. On average, more than 85% of these people are alive and well ten years after diagnosis.
However, breast cancer in men is often diagnosed when larger and at a more advanced stage than in women. This is probably because it is not recognised for what it is, or perhaps because there remains considerable stigma around male breast cancer.
How is male breast cancer treated?
Most men will need a mastectomy, where all the breast tissue is surgically removed, as the tumours can be quite large. Many will also need radiotherapy after mastectomy. Otherwise treatments are very similar to those for breast cancer in women – chemotherapy is recommended for some, especially if the lymph glands are involved, and all are recommended to have the anti-oestrogen drug Tamoxifen.
New breast cancer drugs used in women rely on getting oestrogen levels to almost zero by blocking the production of oestrogen. However, these are not effective in men because testosterone, which is much higher in men, continues to be partly converted to oestrogen, so tumour growth may not be properly blocked.
Why is there a stigma?
Part of the delay in identifying breast cancer symptoms could relate to men’s reluctance to seek medical care in general. However, there are likely to be specific additional issues related to malignancy in an organ that men are not meant to have and may feel embarrassed or in denial about.
Specific differences have been reported in the attitudes and decision-making by men and women in relation to carrying the breast cancer predisposition genes, which are responsible for about 10% of male breast cancers.
Stigma is likely exacerbated by our many “pink” campaigns to raise breast cancer awareness and improve outcomes for women.
Men are as likely as women to experience side effects of treatments – even hot flushes from Tamoxifen – and may have problems coming to terms with their diagnosis, body image, changed sexuality and other effects of treatments such as fatigue. Education about the incidence, risk factors and self-screening methods are important to reduce the delay that causes men’s breast cancers to be detected later, and thus to be more advanced than women’s breast cancers.
All should be offered the support of a breast cancer nurse and counselling where needed. Breast Cancer Network Australia has guidelines and advice on male breast cancers, and an excellent booklet, Men get breast cancer too, as does Cancer Australia: Not just a woman’s disease: Information about breast cancer in men.
Further reading:
Dads get postnatal depression too
Men more reluctant to go to the doctor - and it’s putting them at risk